Diagnostic accuracy of peripheral venous lactate and the 2009 WHO warning signs for identifying severe dengue in Thai adults: a prospective observational study
- PMID: 26832147
- PMCID: PMC4736485
- DOI: 10.1186/s12879-016-1386-5
Diagnostic accuracy of peripheral venous lactate and the 2009 WHO warning signs for identifying severe dengue in Thai adults: a prospective observational study
Abstract
Background: Dengue is the most common mosquito-borne viral disease in humans. However, the sensitivities of warning signs (WSs) for identifying severe dengue in adults are low, and the utility of lactate levels for identifying severe dengue in adults has not been verified. Therefore, we aimed to evaluate the diagnostic accuracy of using peripheral venous lactate levels (PVL), as well as WSs established by the World Health Organization, for identifying severe dengue.
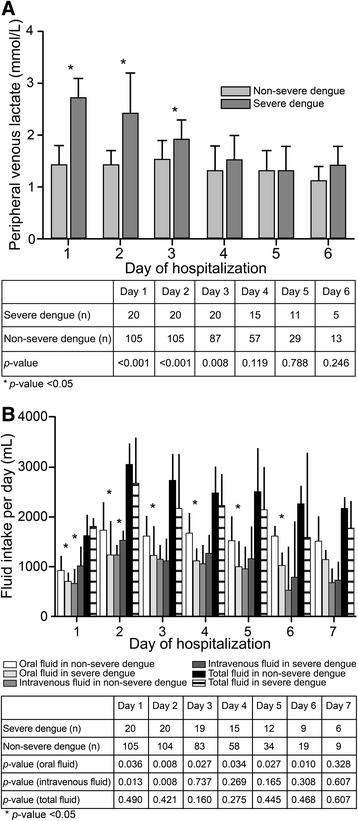
Methods: We prospectively evaluated individuals hospitalized for dengue who were admitted to the Hospital for Tropical Diseases in Thailand between May 2013 and January 2015. Blood samples to evaluate PVL levels were collected at admission and every 24 h until the patient exhibited a body temperature of <37.8 °C for at least 24 h. Data were recorded on a pre-defined case report form, including baseline characteristics, clinical parameters, and laboratory findings.
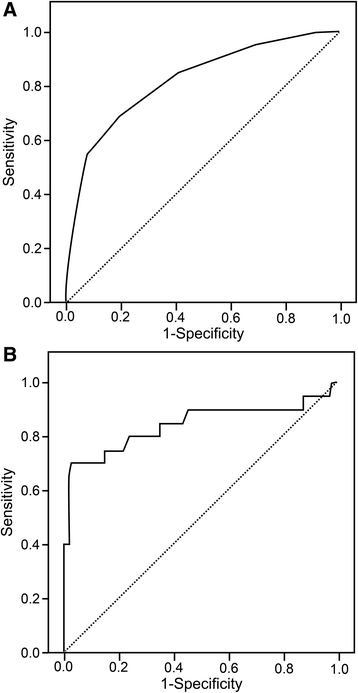
Results: Among 125 patients with confirmed dengue, 105 (84.0%) patients had non-severe dengue, and 20 (16.0%) patients had severe dengue. The presence of clinical fluid accumulation as a WS provided high sensitivity (75.0%, 95% confidence interval [CI]: 50.9-91.3%) and specificity (90.5%, 95% CI: 83.2-95.3%). The PVL level at admission was used to evaluate its diagnostic value, and receiver operating characteristic curve analysis revealed an area under the curve of 0.84 for identifying severe dengue. At the optimal cutoff value (PVL: 2.5 mmol/L), the sensitivity and specificity were 65.0% (95% CI: 40.8-84.6%) and 96.2% (95% CI: 90.5-99.0%), respectively. A combined biomarker comprising clinical fluid accumulation and/or PVL of ≥2.5 mmol/L provided the maximum diagnostic accuracy for identifying severe dengue, with a sensitivity of 90.0% (95% CI: 68.3-98.8%) and a specificity of 87.6% (95% CI: 79.8-93.2%).
Conclusions: Clinical fluid accumulation and/or PVL may be used as a diagnostic biomarker of severe dengue among adults. This biomarker may facilitate early recognition and timely treatment of patients with severe dengue, which may reduce dengue-related mortality and hospital burden.
Figures

References
-
- World Health Organization . Global strategy for dengue prevention and control 2012–2020. Geneva: WHO; 2012.
-
- World Health Organization . Comprehensive guidelines for prevention and control of dengue and dengue hemorrhagic fever. India: WHO; 2011.
-
- Wichmann O, Hongsiriwon S, Bowonwatanuwong C, Chotivanich K, Sukthana Y, Pukrittayakamee S. Risk factors and clinical features associated with severe dengue infection in adults and children during the 2001 epidemic in Chonburi, Thailand. Trop Med Int Health. 2004;9:1022–9. doi: 10.1111/j.1365-3156.2004.01295.x. - DOI - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Research Materials

