The influence of biofilm formation and multidrug resistance on environmental survival of clinical and environmental isolates of Acinetobacter baumannii
- PMID: 26851196
- PMCID: PMC6993530
- DOI: 10.1016/j.ajic.2015.12.012
The influence of biofilm formation and multidrug resistance on environmental survival of clinical and environmental isolates of Acinetobacter baumannii
Abstract
Background: Acinetobacter baumannii is a gram-negative, opportunistic pathogen. Its ability to form biofilm and increasing resistance to antibiotic agents present challenges for infection control. A better understanding of the influence of biofilm formation and antibiotic resistance on environmental persistence of A baumannii in hospital settings is needed for more effective infection control.
Methods: A baumannii strains isolated from patients and the hospital environment were identified via Matrix Assisted Laser Desorption Ionization Time-of-Flight (MALDI-TOF) mass spectrometry (Bruker Daltonics, Bellerica, MA), repetitive extragenic palindromic polymerase chain reaction genotyped, and antibiotic resistance was determined using Vitek 2 (bioMérieux, Inc, Durham NC). Biofilm mass was quantified via microtiter plate method and desiccation tolerance determined up to 56 days.
Results: High biofilm forming, clinical, multidrug-resistant- (MDR) positive strains were 50% less likely to die of desiccation than low biofilm, non-MDR strains. In contrast, environmental, MDR-positive, low biofilm forming strains had a 2.7 times increase in risk of cell death due to desiccation compared with their MDR-negative counterparts. MDR-negative, high biofilm forming environmental strains had a 60% decrease in risk compared with their low biofilm forming counterparts.
Conclusion: The MDR-positive phenotype was deleterious for environmental strains and the high biofilm phenotype was critical for survival. This study provides evidence of the trade-off between antibiotic resistance and desiccation tolerance, driven by condition-dependent adaptation, and establishes rationale for research into the genetic basis of the variation in fitness cost between clinical and environmental isolates.
Keywords: Condition-dependent adaptation; Desiccation tolerance; Environmental transmission; Fitness cost; Hospital; Infection control.
Copyright © 2016 Association for Professionals in Infection Control and Epidemiology, Inc. Published by Elsevier Inc. All rights reserved.
Conflict of interest statement
Figures


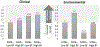
Similar articles
-
Correlation between ability of biofilm formation with their responsible genes and MDR patterns in clinical and environmental Acinetobacter baumannii isolates.Microb Pathog. 2017 Jul;108:122-128. doi: 10.1016/j.micpath.2017.04.039. Epub 2017 Apr 27. Microb Pathog. 2017. PMID: 28457900
-
Clinical isolates of Acinetobacter baumannii from a Portuguese hospital: PFGE characterization, antibiotic susceptibility and biofilm-forming ability.Comp Immunol Microbiol Infect Dis. 2016 Apr;45:29-33. doi: 10.1016/j.cimid.2016.02.002. Epub 2016 Feb 17. Comp Immunol Microbiol Infect Dis. 2016. PMID: 27012918
-
Correlation of biofilm formation and antibiotic resistance among clinical and soil isolates of Acinetobacter baumannii in Iraq.Acta Microbiol Immunol Hung. 2020 Oct 21;67(3):161-170. doi: 10.1556/030.66.2019.026. Acta Microbiol Immunol Hung. 2020. PMID: 31833386
-
Quorum-sensing system in Acinetobacter baumannii: a potential target for new drug development.J Appl Microbiol. 2020 Jan;128(1):15-27. doi: 10.1111/jam.14330. Epub 2019 Jun 26. J Appl Microbiol. 2020. PMID: 31102552 Review.
-
Current treatment strategies for targeting virulence factors and biofilm formation in Acinetobacter baumannii.Future Microbiol. 2024 Jul 2;19(10):941-961. doi: 10.2217/fmb-2023-0263. Epub 2024 Apr 29. Future Microbiol. 2024. PMID: 38683166 Free PMC article. Review.
Cited by
-
An Entomopathogenic Nematode Extends Its Niche by Associating with Different Symbionts.Microb Ecol. 2017 Jan;73(1):211-223. doi: 10.1007/s00248-016-0829-2. Epub 2016 Aug 20. Microb Ecol. 2017. PMID: 27543560
-
Evaluating the Effectiveness of Hospital Antiseptics on Multidrug-Resistant Acinetobacter baumannii: Understanding the Relationship between Microbicide and Antibiotic Resistance.Antibiotics (Basel). 2022 May 3;11(5):614. doi: 10.3390/antibiotics11050614. Antibiotics (Basel). 2022. PMID: 35625258 Free PMC article.
-
Medical Device-Associated Biofilm Infections and Multidrug-Resistant Pathogens.Pathogens. 2024 May 8;13(5):393. doi: 10.3390/pathogens13050393. Pathogens. 2024. PMID: 38787246 Free PMC article. Review.
-
The global epidemiology of carbapenem-resistant Acinetobacter baumannii.JAC Antimicrob Resist. 2025 Jul 29;7(4):dlaf134. doi: 10.1093/jacamr/dlaf134. eCollection 2025 Aug. JAC Antimicrob Resist. 2025. PMID: 40735512 Free PMC article. Review.
-
In vitro and in vivo activities of scutellarein, a novel polyphosphate kinase 1 inhibitor against Acinetobacter baumannii infection.Microb Cell Fact. 2024 Oct 8;23(1):269. doi: 10.1186/s12934-024-02540-9. Microb Cell Fact. 2024. PMID: 39379932 Free PMC article.
References
-
- Weber DJ, Rutala WA, Miller MB, Huslage K, Sickbert-Bennett E. Role of hospital surfaces in the transmission of emerging health care-associated pathogens: norovirus, Clostridium difficile, and Acinetobacter species. Am J Infect Control 2010;38(5 Suppl 1):S25–33. - PubMed
-
- Tacconelli E, Cataldo MA, De Pascale G, Manno D, Spanu T, Cambieri A, et al. Prediction models to identify hospitalized patients at risk of being colonized or infected with multidrug-resistant Acinetobacter baumannii calcoaceticus complex. J Antimicrobial Chemother 2008;62(5):1130–7. - PubMed
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Molecular Biology Databases

