Auxiliary partial liver transplantation for acute liver failure using "high risk" grafts: Case report
- PMID: 26855552
- PMCID: PMC4724624
- DOI: 10.3748/wjg.v22.i5.1919
Auxiliary partial liver transplantation for acute liver failure using "high risk" grafts: Case report
Abstract
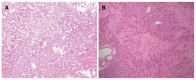
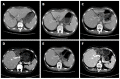
Acute liver failure (ALF) is a reversible disorder that is associated with an abrupt loss of hepatic mass, rapidly progressive encephalopathy and devastating complications. Despite its high mortality, an emergency liver transplantation nowadays forms an integral part in ALF management and has substantially improved the outcomes of ALF. Here, we report the case of a 32-year-old female patient who was admitted with grade IV hepatic encephalopathy (coma) following drug-induced ALF. We performed an emergency auxiliary partial orthotopic liver transplantation with a "high risk" graft (liver macrovesicular steatosis approximately 40%) from a living donor. The patient was discharged on postoperative day 57 with normal liver function. Weaning from immunosuppression was achieved 9 mo after transplantation. A follow-up using CT scan showed a remarkable increase in native liver volume and gradual loss of the graft. More than 6 years after the transplantation, the female now has a 4-year-old child and has returned to work full-time without any neurological sequelae.
Keywords: Acute liver failure; Auxiliary partial orthotopic liver transplantation; Fatty liver graft.
Figures
References
-
- Trey C, Davidson CS. The management of fulminant hepatic failure. Prog Liver Dis. 1970;3:282–298. - PubMed
-
- Bernal W, Wendon J. Acute liver failure. N Engl J Med. 2014;370:1170–1171. - PubMed
-
- Shaw BW. Auxiliary liver transplantation for acute liver failure. Liver Transpl Surg. 1995;1:194–200. - PubMed
-
- Gubernatis G, Pichlmayr R, Kemnitz J, Gratz K. Auxiliary partial orthotopic liver transplantation (APOLT) for fulminant hepatic failure: first successful case report. World J Surg. 1991;15:660–665; discussion 665-666. - PubMed
-
- van Hoek B, de Boer J, Boudjema K, Williams R, Corsmit O, Terpstra OT. Auxiliary versus orthotopic liver transplantation for acute liver failure. EURALT Study Group. European Auxiliary Liver Transplant Registry. J Hepatol. 1999;30:699–705. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

