Endoscopic Submucosal Dissection of an Inverted Early Gastric Cancer-Forming False Gastric Diverticulum
- PMID: 26855930
- PMCID: PMC4743731
- DOI: 10.5946/ce.2016.49.1.86
Endoscopic Submucosal Dissection of an Inverted Early Gastric Cancer-Forming False Gastric Diverticulum
Abstract
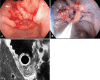
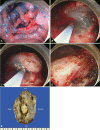
Endoscopic submucosal dissection (ESD) is a standard treatment for early gastric cancer (EGC) that does not have any risk of lymph node or distant metastases. Here, we report a case of EGC resembling a diverticulum. Diverticular formation makes it difficult for endoscopists to determine the depth of invasion and to subsequently perform ESD. Because the false diverticulum does not have a muscular layer, this lesion can be treated with ESD. Our case was successfully treated with ESD. After ESD, the EGC was confined to the submucosal layer without vertical and lateral margin involvement. This is the first case in which ESD was successfully performed for a case of EGC that coexisted with a false gastric diverticulum. An additional, larger study is needed to determine the efficacy of ESD in various types of EGC, such as a false gastric diverticulum.
Keywords: Diverticulum, stomach; Endoscopy, digestive system; Stomach neoplasms.
Conflict of interest statement
Figures

Similar articles
-
[Efficacy comparison between surgical resection and endoscopic submucosal dissection of early gastric cancer in a domestic single center].Zhonghua Wei Chang Wai Ke Za Zhi. 2018 Feb 25;21(2):190-195. Zhonghua Wei Chang Wai Ke Za Zhi. 2018. PMID: 29492919 Chinese.
-
AGA Institute Clinical Practice Update: Endoscopic Submucosal Dissection in the United States.Clin Gastroenterol Hepatol. 2019 Jan;17(1):16-25.e1. doi: 10.1016/j.cgh.2018.07.041. Epub 2018 Aug 2. Clin Gastroenterol Hepatol. 2019. PMID: 30077787 Review.
-
Endoscopic Submucosal Dissection of Early Gastric Cancer with Mixed-Type Histology: A Systematic Review.Dig Dis Sci. 2020 Jan;65(1):276-291. doi: 10.1007/s10620-019-05761-w. Epub 2019 Jul 31. Dig Dis Sci. 2020. PMID: 31367880
-
Feasibility of endoscopic treatment and predictors of lymph node metastasis in early gastric cancer.World J Gastroenterol. 2019 Sep 21;25(35):5344-5355. doi: 10.3748/wjg.v25.i35.5344. World J Gastroenterol. 2019. PMID: 31558878 Free PMC article.
-
[Predictive factors for lymph node metastasis in patients with poorly differentiated early gastric cancer].Zhonghua Wei Chang Wai Ke Za Zhi. 2019 May 25;22(5):446-450. doi: 10.3760/cma.j.issn.1671-0274.2019.05.010. Zhonghua Wei Chang Wai Ke Za Zhi. 2019. PMID: 31104430 Chinese.
Cited by
-
A disconcerting false gastric diverticulum mimicking malignancy.Pan Afr Med J. 2019 Feb 14;32:80. doi: 10.11604/pamj.2019.32.80.18075. eCollection 2019. Pan Afr Med J. 2019. PMID: 31223371 Free PMC article.
-
A rare case of perforated gastric duplication cyst associated with gastric diverticulum.BMJ Case Rep. 2021 Mar 1;14(3):e239971. doi: 10.1136/bcr-2020-239971. BMJ Case Rep. 2021. PMID: 33649025 Free PMC article.
-
Gastric Diverticulum: A Comprehensive Review.Inflamm Intest Dis. 2019 Apr;3(4):161-166. doi: 10.1159/000495463. Epub 2019 Jan 10. Inflamm Intest Dis. 2019. PMID: 31111031 Free PMC article. Review.
-
Upper Gastrointestinal Manifestation of Bezoars and the Etiological Factors: A Literature Review.Gastroenterol Res Pract. 2019 Jul 15;2019:5698532. doi: 10.1155/2019/5698532. eCollection 2019. Gastroenterol Res Pract. 2019. PMID: 31396274 Free PMC article. Review.
References
-
- Japanese Gastric Cancer Association Japanese classification of gastric carcinoma: 3rd English edition. Gastric Cancer. 2011;14:101–112. - PubMed
-
- Sano T, Aiko T. New Japanese classifications and treatment guidelines for gastric cancer: revision concepts and major revised points. Gastric Cancer. 2011;14:97–100. - PubMed
-
- Gotoda T. Endoscopic resection of early gastric cancer. Gastric Cancer. 2007;10:1–11. - PubMed
-
- Moses WR. Diverticula of the stomach. Arch Surg. 1946;52:59–65. - PubMed
LinkOut - more resources
Full Text Sources
Other Literature Sources
Miscellaneous

