Management of peri-implantitis: a systematic review, 2010-2015
- PMID: 26877903
- PMCID: PMC4735040
- DOI: 10.1186/s40064-016-1735-2
Management of peri-implantitis: a systematic review, 2010-2015
Abstract
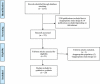
Peri-implantitis or Periimplantitis is characterized as an inflammatory reaction that affects the hard and soft tissue, which results in loss of supporting bone and pocket formation surrounding the functioning osseointegrated implant. This review aimed to evaluate the effectiveness of surgical and non-surgical treatment of peri-implantitis. The data sources used was PubMed. Searches of this database were restricted to English language publications from January 2010 to June 2015. All Randomized Controlled Trials describing the treatments of peri-implantitis of human studies with a follow up of at least 6 months were included. Eligibility and quality were assessed and two reviewers extracted the data. Data extraction comprised of type, intensity provider, and location of the intervention. A total of 20 publications were included (10 involving surgical and 10 involving non-surgical mechanical procedure). The non-surgical approach involves the mechanical surface debridement using carbon or titanium currettes, laser light, and antibiotics whereas, surgical approach involves implantoplasty, elevation of mucoperiosteal flap and removal of peri-inflammatory granulation tissue followed by surface decontamination and bone grafting. This study reveals that non-surgical therapy tends to remove only the local irritant from the peri-implantitis surface with or without some additional adjunctive therapies agents or device. Hence, non-surgical therapy is not helpful in osseous defect. Surgical therapy in combination with osseous resective or regenerative approach removes the residual sub-gingival deposits additionally reducing the peri-implantitis pocket. Although there is no specific recommendation for the treatment of peri-implantitis, surgical therapy in combination with osseous resective or regenerative approach showed the positive outcome.
Keywords: Dental implant bone loss; Peri-implantitis treatment; Surgical and non-surgical therapy.
References
-
- Froum SJ, Rosen PS. A proposed classification for peri-implantitis. Int J Periodontics Restorative Dent. 2012;32(5):533–540. - PubMed
Publication types
LinkOut - more resources
Full Text Sources
Other Literature Sources