MR Imaging in Diagnosis of Pelvic Floor Descent: Supine versus Sitting Position
- PMID: 26880893
- PMCID: PMC4737448
- DOI: 10.1155/2016/6594152
MR Imaging in Diagnosis of Pelvic Floor Descent: Supine versus Sitting Position
Abstract
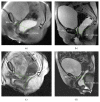
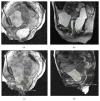
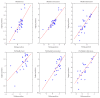
Introduction. Functional disorders of the pelvic floor represent have a significant impact on the quality of life. The advent of open-configuration systems allowed for the evaluation of defecation with MR imaging in sitting position. The purpose of the present study is to compare the results of static and dynamic pelvic MR performed in supine position versus sitting position, using a new MR prototype machine, in the diagnosis of pelvic floor descent. Materials and Methods. Thirty-one patients with pelvic floor disorders were enrolled, and underwent MR Defecography in supine position with 1.5 T closed magnet (MAGNETOM Symphony, Siemens, Germany) and in sitting position with a 0.25-Tesla open magnet system (G-Scan ESAOTE, Italy). Results. In rest and squeezing phases, positions of bladder, vagina, and ARJ were significantly different when the patient was imaged in supine versus sitting position. In the defecation phase, a significant difference for the bladder and vagina position was detected between the two exams whereas a significant difference for the ARJ was not found. A statistically significant difference exists when the pelvic floor descent is evaluated in sitting versus supine position. Conclusion. Our results show that MR Defecography in sitting position may represent a useful tool to correctly diagnose and grade the pelvic organ descent.
Figures





Similar articles
-
Dynamic MR imaging of the pelvic floor performed with patient sitting in an open-magnet unit versus with patient supine in a closed-magnet unit.Radiology. 2002 May;223(2):501-8. doi: 10.1148/radiol.2232010665. Radiology. 2002. PMID: 11997560
-
Dynamic MR defecography with an open-configuration, low-field, tilting MR system in patients with pelvic floor disorders.Radiol Med. 2011 Jun;116(4):620-33. doi: 10.1007/s11547-011-0660-2. Epub 2011 Mar 19. Radiol Med. 2011. PMID: 21424567 English, Italian.
-
MR imaging of pelvic floor continence mechanisms in the supine and sitting positions.AJR Am J Roentgenol. 1998 Dec;171(6):1607-10. doi: 10.2214/ajr.171.6.9843296. AJR Am J Roentgenol. 1998. PMID: 9843296
-
[Dynamic magnetic resonance imaging of the pelvic floor: Technical aspects].Radiologie (Heidelb). 2023 Nov;63(11):793-798. doi: 10.1007/s00117-023-01212-w. Epub 2023 Oct 13. Radiologie (Heidelb). 2023. PMID: 37831100 Review. German.
-
Comparison between dynamic cystocolpoproctography and dynamic pelvic floor MRI: pros and cons: which is the "functional" examination for anorectal and pelvic floor dysfunction?Abdom Imaging. 2013 Oct;38(5):952-73. doi: 10.1007/s00261-012-9870-x. Abdom Imaging. 2013. PMID: 22446896 Review.
Cited by
-
Static and Dynamic Magnetic Resonance Imaging in Female Pelvic Floor Dysfunction: Correlation With Pelvic Organ Prolapse Quantification.Cureus. 2023 Sep 8;15(9):e44915. doi: 10.7759/cureus.44915. eCollection 2023 Sep. Cureus. 2023. PMID: 37814774 Free PMC article.
-
Magnetic Resonance Imaging of the Gastrointestinal Tract: Current Role, Recent Advancements and Future Prospectives.Diagnostics (Basel). 2023 Jul 19;13(14):2410. doi: 10.3390/diagnostics13142410. Diagnostics (Basel). 2023. PMID: 37510154 Free PMC article. Review.
-
Current diagnostic tools and treatment modalities for rectal prolapse.World J Clin Cases. 2023 Jun 6;11(16):3680-3693. doi: 10.12998/wjcc.v11.i16.3680. World J Clin Cases. 2023. PMID: 37383136 Free PMC article. Review.
-
Clinical applications of pelvic floor imaging: opinion statement endorsed by the society of abdominal radiology (SAR), American Urological Association (AUA), and American Urogynecologic Society (AUGS).Abdom Radiol (NY). 2021 Apr;46(4):1451-1464. doi: 10.1007/s00261-021-03017-8. Epub 2021 Mar 27. Abdom Radiol (NY). 2021. PMID: 33772614
-
Radiological Assessment After Pancreaticoduodenectomy for a Precision Approach to Managing Complications: A Narrative Review.J Pers Med. 2025 May 28;15(6):220. doi: 10.3390/jpm15060220. J Pers Med. 2025. PMID: 40559083 Free PMC article. Review.
References
-
- Cappabianca S., Reginelli A., Iacobellis F., et al. Dynamic MRI defecography vs. entero-colpo-cysto-defecography in the evaluation of midline pelvic floor hernias in female pelvic floor disorders. International Journal of Colorectal Disease. 2011;26(9):1191–1196. doi: 10.1007/s00384-011-1218-4. - DOI - PubMed
-
- Bertschinger K. M., Hetzer F. H., Roos J. E., Treiber K., Marincek B., Hilfiker P. R. Dynamic MR imaging of the pelvic floor performed with patient sitting in an open-magnet unit versus with patient supine in a closed-magnet unit. Radiology. 2002;223(2):501–508. doi: 10.1148/radiol.2232010665. - DOI - PubMed
LinkOut - more resources
Full Text Sources
Other Literature Sources

