The sympathetic nervous system and catecholamines metabolism in obstructive sleep apnoea
- PMID: 26904265
- PMCID: PMC4739957
- DOI: 10.3978/j.issn.2072-1439.2015.11.14
The sympathetic nervous system and catecholamines metabolism in obstructive sleep apnoea
Abstract
Obstructive sleep apnoea (OSA) is the most common sleep disorder of breathing in middle-aged and overweight subjects. It features recurrent episodes of upper airway total (apnoea) o partial (hypopnea) collapse during sleep, which are associated with a reduction in blood oxygen saturation and with arousal from sleep to re-establish airway patency. An association of OSA with dysregulation of the autonomous nervous system (ANS) and altered catecholamines (CAs) metabolism has been contended for years. However, the pathophysiology mechanisms underlying these alterations remain to be fully clarified. Nonetheless, these alterations are deemed to play a key pathogenic role in the established association of OSA with several conditions besides arterial hypertension (HT), including coronary artery disease, stroke, and, more in general, with increased risk of cardiovascular (CV) events. Hence, in this review we will analyse the relationship between the sleep disturbances associated with OSA and the altered function of the ANS, including CAs metabolism.
Keywords: Obstructive sleep apnoea (OSA); cardiovascular risk (CV risk); catecholamines (CAs); sympathetic nervous system (SNS).
Conflict of interest statement
Figures

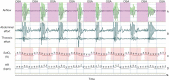
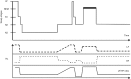
References
-
- American Academy of Sleep Medicine. The international classification of sleep disorders, revised Diagnostic and Coding Manual. Library of Congress Catalog No. 97-71405.
-
- Somers VK, White DP, Amin R, et al. Sleep apnea and cardiovascular disease: an American Heart Association/American College Of Cardiology Foundation Scientific Statement from the American Heart Association Council for High Blood Pressure Research Professional Education Committee, Council on Clinical Cardiology, Stroke Council, and Council On Cardiovascular Nursing. In collaboration with the National Heart, Lung, and Blood Institute National Center on Sleep Disorders Research (National Institutes of Health). Circulation 2008;118:1080-111. - PubMed
-
- Steier J, Lunt A, Hart N, et al. Observational study of the effect of obesity on lung volumes. Thorax 2014;69:752-9. - PubMed
-
- Young T, Palta M, Dempsey J, et al. The occurrence of sleep-disordered breathing among middle-aged adults. N Engl J Med 1993;328:1230-5. - PubMed
Publication types
LinkOut - more resources
Full Text Sources
