Harnessing publicly available genetic data to prioritize lipid modifying therapeutic targets for prevention of coronary heart disease based on dysglycemic risk
- PMID: 26946290
- PMCID: PMC4835528
- DOI: 10.1007/s00439-016-1647-9
Harnessing publicly available genetic data to prioritize lipid modifying therapeutic targets for prevention of coronary heart disease based on dysglycemic risk
Abstract
Therapeutic interventions that lower LDL-cholesterol effectively reduce the risk of coronary artery disease (CAD). However, statins, the most widely prescribed LDL-cholesterol lowering drugs, increase diabetes risk. We used genome-wide association study (GWAS) data in the public domain to investigate the relationship of LDL-C and diabetes and identify loci encoding potential drug targets for LDL-cholesterol modification without causing dysglycemia. We obtained summary-level GWAS data for LDL-C from GLGC, glycemic traits from MAGIC, diabetes from DIAGRAM and CAD from CARDIoGRAMplusC4D consortia. Mendelian randomization analyses identified a one standard deviation (SD) increase in LDL-C caused an increased risk of CAD (odds ratio [OR] 1.63 (95 % confidence interval [CI] 1.55, 1.71), which was not influenced by removing SNPs associated with diabetes. LDL-C/CAD-associated SNPs showed consistent effect directions (binomial P = 6.85 × 10(-5)). Conversely, a 1-SD increase in LDL-C was causally protective of diabetes (OR 0.86; 95 % CI 0.81, 0.91), however LDL-cholesterol/diabetes-associated SNPs did not show consistent effect directions (binomial P = 0.15). HMGCR, our positive control, associated with LDL-C, CAD and a glycemic composite (derived from GWAS meta-analysis of four glycemic traits and diabetes). In contrast, PCSK9, APOB, LPA, CETP, PLG, NPC1L1 and ALDH2 were identified as "druggable" loci that alter LDL-C and risk of CAD without displaying associations with dysglycemia. In conclusion, LDL-C increases the risk of CAD and the relationship is independent of any association of LDL-C with diabetes. Loci that encode targets of emerging LDL-C lowering drugs do not associate with dysglycemia, and this provides provisional evidence that new LDL-C lowering drugs (such as PCSK9 inhibitors) may not influence risk of diabetes.
Trial registration: ClinicalTrials.gov NCT01475825 NCT02160899.
Conflict of interest statement
DIS is a consultant to Pfizer.
Figures
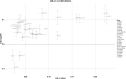


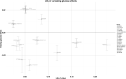

References
-
- Akdim F, Stroes ES, Sijbrands EJ, Tribble DL, Trip MD, Jukema JW, Flaim JD, Su J, Yu R, Baker BF, Wedel MK, Kastelein JJ. Efficacy and safety of mipomersen, an antisense inhibitor of apolipoprotein B, in hypercholesterolemic subjects receiving stable statin therapy. J Am Coll Cardiol. 2010;55:1611–1618. doi: 10.1016/j.jacc.2009.11.069. - DOI - PubMed
-
- Baigent C, Collins R, Appleby P, Parish S, Sleight P, Peto R. ISIS-2: 10 year survival among patients with suspected acute myocardial infarction in randomised comparison of intravenous streptokinase, oral aspirin, both, or neither. The ISIS-2 (Second International Study of Infarct Survival) Collaborative Group. BMJ. 1998;316:1337–1343. doi: 10.1136/bmj.316.7141.1337. - DOI - PMC - PubMed
-
- Bloomfield D, Carlson GL, Sapre A, Tribble D, McKenney JM, Littlejohn TW, 3rd, Sisk CM, Mitchel Y, Pasternak RC. Efficacy and safety of the cholesteryl ester transfer protein inhibitor anacetrapib as monotherapy and coadministered with atorvastatin in dyslipidemic patients. Am Heart J. 2009;157(352–360):e2. - PubMed
Publication types
MeSH terms
Substances
Associated data
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Miscellaneous

