Long-term financing needs for HIV control in sub-Saharan Africa in 2015-2050: a modelling study
- PMID: 26948960
- PMCID: PMC4785296
- DOI: 10.1136/bmjopen-2015-009656
Long-term financing needs for HIV control in sub-Saharan Africa in 2015-2050: a modelling study
Abstract
Objectives: To estimate the present value of current and future funding needed for HIV treatment and prevention in 9 sub-Saharan African (SSA) countries that account for 70% of HIV burden in Africa under different scenarios of intervention scale-up. To analyse the gaps between current expenditures and funding obligation, and discuss the policy implications of future financing needs.
Design: We used the Goals module from Spectrum, and applied the most up-to-date cost and coverage data to provide a range of estimates for future financing obligations. The four different scale-up scenarios vary by treatment initiation threshold and service coverage level. We compared the model projections to current domestic and international financial sources available in selected SSA countries.
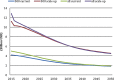
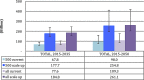
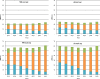
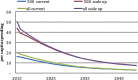
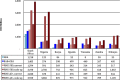
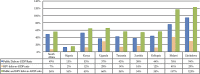
Results: In the 9 SSA countries, the estimated resources required for HIV prevention and treatment in 2015-2050 range from US$98 billion to maintain current coverage levels for treatment and prevention with eligibility for treatment initiation at CD4 count of <500/mm(3) to US$261 billion if treatment were to be extended to all HIV-positive individuals and prevention scaled up. With the addition of new funding obligations for HIV--which arise implicitly through commitment to achieve higher than current treatment coverage levels--overall financial obligations (sum of debt levels and the present value of the stock of future HIV funding obligations) would rise substantially.
Conclusions: Investing upfront in scale-up of HIV services to achieve high coverage levels will reduce HIV incidence, prevention and future treatment expenditures by realising long-term preventive effects of ART to reduce HIV transmission. Future obligations are too substantial for most SSA countries to be met from domestic sources alone. New sources of funding, in addition to domestic sources, include innovative financing. Debt sustainability for sustained HIV response is an urgent imperative for affected countries and donors.
Keywords: PUBLIC HEALTH.
Published by the BMJ Publishing Group Limited. For permission to use (where not already granted under a licence) please go to http://www.bmj.com/company/products-services/rights-and-licensing/
Figures
Similar articles
-
The HIV Treatment Gap: Estimates of the Financial Resources Needed versus Available for Scale-Up of Antiretroviral Therapy in 97 Countries from 2015 to 2020.PLoS Med. 2015 Nov 24;12(11):e1001907; discussion e1001907. doi: 10.1371/journal.pmed.1001907. eCollection 2015 Nov. PLoS Med. 2015. PMID: 26599990 Free PMC article.
-
Funding AIDS programmes in the era of shared responsibility: an analysis of domestic spending in 12 low-income and middle-income countries.Lancet Glob Health. 2015 Jan;3(1):e52-61. doi: 10.1016/S2214-109X(14)70342-0. Lancet Glob Health. 2015. PMID: 25539970
-
The future of financing for HIV services in Uganda and the wider sub-Saharan Africa region: should we ask patients to contribute to the cost of their care?BMC Public Health. 2016 Aug 27;16(1):896. doi: 10.1186/s12889-016-3573-0. BMC Public Health. 2016. PMID: 27567669 Free PMC article.
-
Public and private donor financing for health in developing countries.Infect Dis Clin North Am. 1991 Jun;5(2):221-34. Infect Dis Clin North Am. 1991. PMID: 1869807 Review.
-
Innovative approaches to HIV/AIDS financing: lessons learned from the Sustainable Financing Initiative (SFI).BMC Health Serv Res. 2025 May 28;24(Suppl 1):1669. doi: 10.1186/s12913-025-12529-8. BMC Health Serv Res. 2025. PMID: 40437408 Free PMC article. Review.
Cited by
-
Individual and healthcare supply-related HIV transmission factors in HIV-positive patients enrolled in the antiretroviral treatment access program in the Centre and Littoral regions in Cameroon (ANRS-12288 EVOLCam survey).PLoS One. 2022 Apr 6;17(4):e0266451. doi: 10.1371/journal.pone.0266451. eCollection 2022. PLoS One. 2022. PMID: 35385535 Free PMC article.
-
Innovative financing to fund surgical systems and expand surgical care in low-income and middle-income countries.BMJ Glob Health. 2020 Jun;5(6):e002375. doi: 10.1136/bmjgh-2020-002375. BMJ Glob Health. 2020. PMID: 32546586 Free PMC article. Review.
-
Getting resources to those who need them: the evidence we need to budget for underserved populations in sub-Saharan Africa.J Int AIDS Soc. 2021 Jul;24 Suppl 3(Suppl 3):e25707. doi: 10.1002/jia2.25707. J Int AIDS Soc. 2021. PMID: 34189873 Free PMC article.
-
Can differentiated care models solve the crisis in HIV treatment financing? Analysis of prospects for 38 countries in sub-Saharan Africa.J Int AIDS Soc. 2017 Jul 21;20(Suppl 4):21648. doi: 10.7448/IAS.20.5.21648. J Int AIDS Soc. 2017. PMID: 28770597 Free PMC article.
-
The impact of community health worker-led home delivery of antiretroviral therapy on virological suppression: a non-inferiority cluster-randomized health systems trial in Dar es Salaam, Tanzania.BMC Health Serv Res. 2017 Feb 22;17(1):160. doi: 10.1186/s12913-017-2032-7. BMC Health Serv Res. 2017. PMID: 28228134 Free PMC article. Clinical Trial.
References
-
- Coker R, Atun RA, McKee M. Health systems and communicable disease control. McGraw Hill, Open University Press, 2008.
-
- IOM (Institute of Medicine). Investing in global health systems: sustaining gains, transforming lives. Washington DC: The National Academies Press, 2014. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Research Materials
Miscellaneous
