Neurolymphomatosis in a cat
- PMID: 26960326
- PMCID: PMC4937145
- DOI: 10.1292/jvms.15-0553
Neurolymphomatosis in a cat
Abstract
A 9-year-old male mixed breed cat showed chronic progressive neurological symptoms, which are represented by ataxia and seizures. At necropsy, spinal roots and spinal ganglions at the level of sixth cervical nerve to second thoracic nerve were bilaterally swollen and replaced by white mass lesions. Right brachial plexus and cranial nerves (III, V and VII) were also swollen. A mass lesion was found in the right frontal lobe of the cerebrum. Histologically, neoplastic lymphocytes extensively involved the peripheral nerves, and they infiltrated into the cerebral and spinal parenchyma according to the peripheral nerve tract. Immunohistochemically, most neoplastic lymphocytes were positive for CD20. The clinical and histological features in this case resemble those of neurolymphomatosis in humans.
Figures
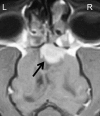





References
-
- Kosari F., Shishehbor F., Saffar H., Sadeghipour A.2013. PCR-based clonality analysis in diffuse large B-cell lymphoma using BIOMED-2 primers of IgH (FR3) on formalin-fixed paraffin-embedded tissue. Arch. Iran Med. 16: 526–529. - PubMed
-
- Grisariu S., Avni B., Batchelor T. T., van den Bent M. J., Bokstein F., Schiff D., Kuittinen O., Chamberlain M. C., Roth P., Nemets A., Shalom E., Ben-Yehuda D., Siegal T., International Primary CNS Lymphoma Collaborative Group2010. Neurolymphomatosis: an International Primary CNS Lymphoma Collaborative Group report. Blood 115: 5005–5011. doi: 10.1182/blood-2009-12-258210 - DOI - PMC - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Miscellaneous

