The effect of visceral obesity on clinicopathological features in patients with endometrial cancer: a retrospective analysis of 200 Chinese patients
- PMID: 26968382
- PMCID: PMC4788937
- DOI: 10.1186/s12885-016-2230-4
The effect of visceral obesity on clinicopathological features in patients with endometrial cancer: a retrospective analysis of 200 Chinese patients
Abstract
Background: To assess the effect of visceral adiposity on clinical and pathological characteristics in patients with endometrial cancer.
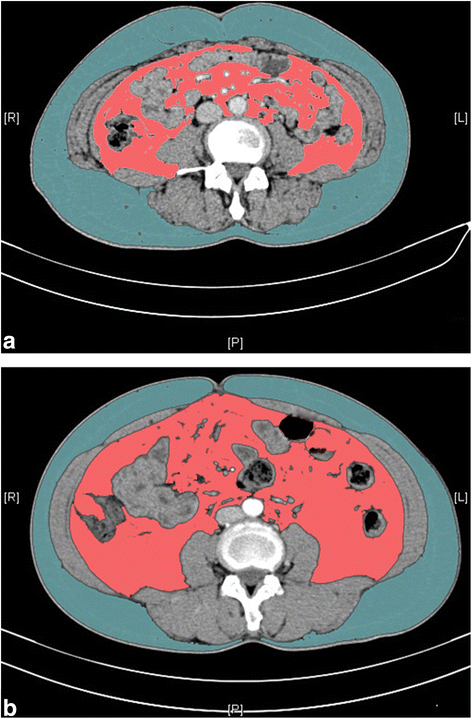
Methods: A retrospective review of medical documentation was performed in surgically treated endometrial cancer patients from January to November 2015 in our institution. The visceral adipose tissue (VAT) and subcutaneous adipose tissue (SAT) were measured at the level of umbilicus on single-slice computerized tomography. Visceral adiposity (VAT%) was calculated as VAT/(VAT + SAT).
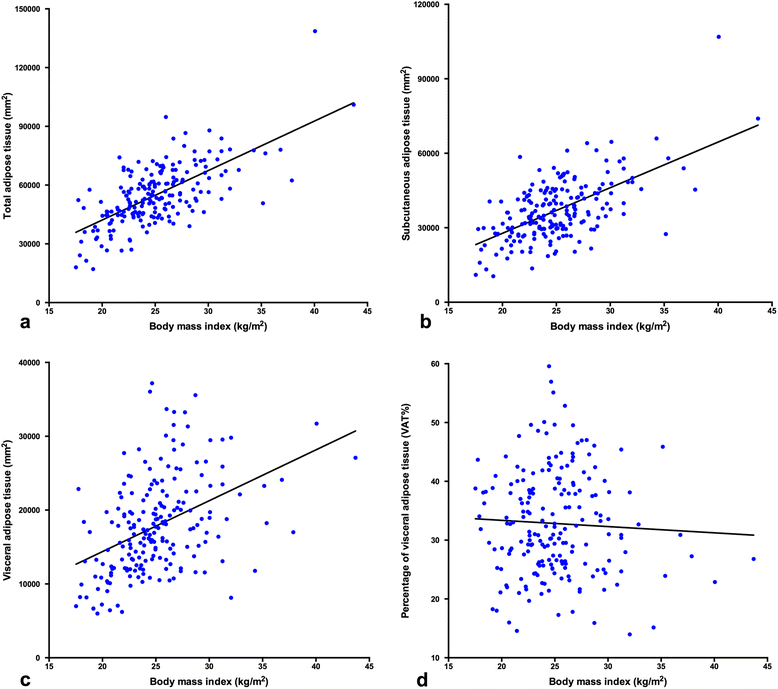
Results: A total of 200 cases were included in the study. Median age at diagnosis was 54 years old. Most patients presented with early-stage tumor (86.0% for I + II) and endometrioid histology (90.5%). Positive lymph node occurred in 11.0% (22/200) of the patients with the median number of retrieved nodes as 25 (range, 4-56). The entire population had a median body mass index (BMI) of 24.7 kg/m(2) and median VAT% of 31.89%. BMI correlated with total adipose tissue (correlation coefficient = 0.667, P < 0.001), but not with VAT% (P = 0.495). Viscerally obese patients tended to be old and post-menopausal (P < 0.001; P = 0.003). Nodal metastasis and extrauterine disease were more commonly reported in patients with high VAT% (6.0% vs. 16.0%, P = 0.024; 9.0% vs. 19.0%, P = 0.042, respectively). Univariate and multivariate logistic regressions were performed to discern the contribution of variable factors on the lymph node metastasis. Grade (HR = 15.41, 95% CI = 1.60-148.76; P = 0.018), lympho-vascular invasion (HR = 449.61, 95% CI = 31.27-6463.93; P < 0.001) and high VAT% (HR = 6.37, 95% CI = 1.42-28.69; P = 0.016) retained statistical significance for predicting lymph node metastasis.
Conclusions: Viscerally obese patients were more likely to be old and have positive lymph node as well as extrauterine disease. Grade, lympho-vascular invasion presence and visceral adiposity were predictors of nodal disease.
Keywords: Body mass index; Clinicopathological features; Endometrial cancer; Lymph node metastasis; Visceral adiposity.
Figures

Similar articles
-
Visceral adiposity and inflammatory bowel disease.Int J Colorectal Dis. 2021 Nov;36(11):2305-2319. doi: 10.1007/s00384-021-03968-w. Epub 2021 Jun 9. Int J Colorectal Dis. 2021. PMID: 34104989 Review.
-
Visceral abdominal obesity is associated with an increased risk of irritable bowel syndrome.Am J Gastroenterol. 2015 Feb;110(2):310-9. doi: 10.1038/ajg.2014.422. Epub 2015 Jan 13. Am J Gastroenterol. 2015. PMID: 25583325
-
Increased Abdominal Adiposity in Adolescents and Young Adults With Classical Congenital Adrenal Hyperplasia due to 21-Hydroxylase Deficiency.J Clin Endocrinol Metab. 2015 Aug;100(8):E1153-9. doi: 10.1210/jc.2014-4033. Epub 2015 Jun 10. J Clin Endocrinol Metab. 2015. PMID: 26062016 Free PMC article.
-
Influence of motor complete spinal cord injury on visceral and subcutaneous adipose tissue measured by multi-axial magnetic resonance imaging.J Spinal Cord Med. 2011;34(1):99-109. doi: 10.1179/107902610X12911165975106. J Spinal Cord Med. 2011. PMID: 21528633 Free PMC article. Clinical Trial.
-
Visceral fat and cardiometabolic future in children and adolescents: a critical update.Pediatr Res. 2023 Nov;94(5):1639-1647. doi: 10.1038/s41390-023-02709-9. Epub 2023 Jul 4. Pediatr Res. 2023. PMID: 37402844 Review.
Cited by
-
Visceral-to-subcutaneous fat ratio is a possible prognostic factor for type 1 endometrial cancer.Int J Clin Oncol. 2022 Feb;27(2):434-440. doi: 10.1007/s10147-021-02060-1. Epub 2021 Oct 30. Int J Clin Oncol. 2022. PMID: 34716844 Free PMC article.
-
Association Between Abdominal Adipose Tissue Distribution and Risk of Endometrial Cancer: A Case-Control Study.Clin Med Insights Oncol. 2022 Dec 9;16:11795549221140776. doi: 10.1177/11795549221140776. eCollection 2022. Clin Med Insights Oncol. 2022. PMID: 36519031 Free PMC article.
-
Abdominal fat distribution in endometrial cancer: from diagnosis to follow-up.BMC Cancer. 2025 May 15;25(1):879. doi: 10.1186/s12885-025-14155-3. BMC Cancer. 2025. PMID: 40375215 Free PMC article.
-
Correlation between abdominal visceral fat and the risk of endometrial cancer in patients with polycystic ovary syndrome.Afr Health Sci. 2024 Sep;24(3):180-187. doi: 10.4314/ahs.v24i3.22. Afr Health Sci. 2024. PMID: 40777932 Free PMC article.
-
Mechanism of PTPN18 for regulating the migration and invasion of endometrial cancer cells via the MYC/PI3K/AKT pathway.Histol Histopathol. 2025 Feb;40(2):215-223. doi: 10.14670/HH-18-767. Epub 2024 May 27. Histol Histopathol. 2025. PMID: 38855855
References
-
- Popkin BM. The nutrition transition and obesity in the developing world. J Nutr. 2001;131(3):871s–3. - PubMed
-
- Friedenreich C, Cust A, Lahmann PH, Steindorf K, Boutron-Ruault MC, Clavel-Chapelon F, et al. Anthropometric factors and risk of endometrial cancer: the European prospective investigation into cancer and nutrition. Cancer Causes Control. 2007;18(4):399–413. doi: 10.1007/s10552-006-0113-8. - DOI - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Research Materials

