Non-intubated video-assisted thoracoscopic surgery under loco-regional anaesthesia for thoracic surgery: a meta-analysis
- PMID: 26984963
- PMCID: PMC4986734
- DOI: 10.1093/icvts/ivw055
Non-intubated video-assisted thoracoscopic surgery under loco-regional anaesthesia for thoracic surgery: a meta-analysis
Abstract
Objectives: The short-term feasibility and safety of non-intubated video-assisted thoracoscopic surgery under loco-regional anaesthesia for thoracic surgery remains unknown. Therefore, we conducted a meta-analysis to provide evidence for the short-term efficacy and safety profile of non-intubated video-assisted thoracoscopic surgery under loco-regional anaesthesia for thoracic surgery.
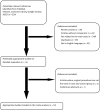
Methods: We performed a systematic literature search in PubMed, Embase, Cochrane Library databases and Google Scholar, as well as American Society of Clinical Oncology to identify relevant studies comparing non-intubated video-assisted thoracoscopic surgery under loco-regional anaesthesia with conventionally intubated video-assisted thoracoscopic surgery under general anaesthesia, dated up to 31 August 2015. Data concerning global in-operating room time, hospital stays, rate of postoperative complications and perioperative mortality were extracted and analysed. We conducted a meta-analysis of the overall results and two subgroup analyses based on study design (a meta-analysis of randomized controlled trials and a second meta-analysis of observational studies).
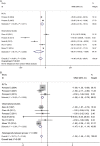
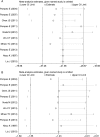
Results: Four randomized controlled trials and six observational studies with a total of 1283 patients were included. We found that in the overall analysis, patients treated with non-intubated video-assisted thoracoscopic surgery under loco-regional anaesthesia achieved significantly shorter global in-operating room time [weighted mean difference = -41.96; 95% confidence interval (CI) = (-57.26, -26.67); P < 0.001] and hospital stays [weighted mean difference = -1.24; 95% CI = (-1.46, -1.02); P < 0.001] as well as a lower rate of postoperative complications [relative risk = 0.55; 95% CI = (0.40, 0.74); P < 0.001] than patients treated with intubated video-assisted thoracoscopic surgery under general anaesthesia. Subgroup meta-analyses based on study design achieved the same outcomes as overall analysis. In our meta-analysis, no perioperative mortality was observed in patients treated with non-intubated video-assisted thoracoscopic surgery under loco-regional anaesthesia.
Conclusions: Non-intubated video-assisted thoracoscopic surgery under loco-regional anaesthesia for thoracic surgery proved to be feasible and safe. Future multicentre and well-designed randomized controlled trials with longer follow-up are needed to confirm and update the findings of our study, as well as the long-term efficacy of non-intubated video-assisted thoracoscopic surgery under loco-regional anaesthesia.
Keywords: Anaesthesia; Meta-analysis; Non-intubated; Thoracic surgery; Video-assisted thoracoscopic surgery.
© The Author 2016. Published by Oxford University Press on behalf of the European Association for Cardio-Thoracic Surgery. All rights reserved.
Figures


Similar articles
-
Non-intubated spontaneous ventilation in video-assisted thoracoscopic surgery: a meta-analysis.Eur J Cardiothorac Surg. 2020 Mar 1;57(3):428-437. doi: 10.1093/ejcts/ezz279. Eur J Cardiothorac Surg. 2020. PMID: 31725158
-
Comparison of non-intubated and intubated video-assisted thoracoscopic surgery for perioperative complications-a systematic review and meta-analysis.BMC Anesthesiol. 2025 May 29;25(1):272. doi: 10.1186/s12871-025-03154-3. BMC Anesthesiol. 2025. PMID: 40442616 Free PMC article.
-
Non-intubated thoracoscopic lobectomies for lung cancer: an exploratory systematic review and meta-analysis.Interact Cardiovasc Thorac Surg. 2020 Oct 1;31(4):499-506. doi: 10.1093/icvts/ivaa141. Interact Cardiovasc Thorac Surg. 2020. PMID: 32918464
-
A comparison of non-intubated video-assisted thoracic surgery with spontaneous ventilation and intubated video-assisted thoracic surgery: a meta-analysis based on 14 randomized controlled trials.J Thorac Dis. 2021 Mar;13(3):1624-1640. doi: 10.21037/jtd-20-3039. J Thorac Dis. 2021. PMID: 33841954 Free PMC article.
-
Postoperative pulmonary complications and hospital stay after lung resection surgery: A meta-analysis comparing nonintubated and intubated anesthesia.Medicine (Baltimore). 2018 May;97(21):e10596. doi: 10.1097/MD.0000000000010596. Medicine (Baltimore). 2018. PMID: 29794734 Free PMC article. Review.
Cited by
-
Epidural for mini-invasive thoracic surgery: do we need a sledgehammer to crack a nut?J Thorac Dis. 2018 Jul;10(Suppl 18):S2223-S2224. doi: 10.21037/jtd.2018.06.117. J Thorac Dis. 2018. PMID: 30123569 Free PMC article. No abstract available.
-
A glance at the history of uniportal video-assisted thoracic surgery.J Vis Surg. 2017 Nov 7;3:157. doi: 10.21037/jovs.2017.10.11. eCollection 2017. J Vis Surg. 2017. PMID: 29302433 Free PMC article. Review.
-
Developing a minimally-invasive anaesthesiological approach to non-intubated uniportal video-assisted thoracoscopic surgery in minor and major thoracic surgery.J Thorac Dis. 2020 Dec;12(12):7202-7217. doi: 10.21037/jtd-20-2122. J Thorac Dis. 2020. PMID: 33447409 Free PMC article.
-
Risk Factors for the Development of Intraoperative Hypoxia in Patients Undergoing Nonintubated Video-Assisted Thoracic Surgery: A Retrospective Study from a Single Center.Med Sci Monit. 2021 Apr 26;27:e928965. doi: 10.12659/MSM.928965. Med Sci Monit. 2021. PMID: 33901163 Free PMC article.
-
Non-Intubated Thoracic Surgery: Standpoints and Perspectives.Front Surg. 2022 Jul 1;9:937633. doi: 10.3389/fsurg.2022.937633. eCollection 2022. Front Surg. 2022. PMID: 36034396 Free PMC article.
References
-
- Gonzalez-Rivas D, Bonome C, Fieira E, Aymerich H, Fernandez R, Delgado M et al. . Non-intubated video-assisted thoracoscopic lung resections: the future of thoracic surgery? Eur J Cardiothorac Surg 2016;49:721–31. - PubMed
-
- Sugasawa Y, Yamaguchi K, Kumakura S, Murakami T, Kugimiya T, Suzuki K et al. . The effect of one-lung ventilation upon pulmonary inflammatory responses during lung resection. J Anesth 2011;25:170–7. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

