Increased Intraoperative Fluid Administration Is Associated with Severe Primary Graft Dysfunction After Lung Transplantation
- PMID: 26991618
- PMCID: PMC4800821
- DOI: 10.1213/ANE.0000000000001163
Increased Intraoperative Fluid Administration Is Associated with Severe Primary Graft Dysfunction After Lung Transplantation
Abstract
Background: Severe primary graft dysfunction (PGD) is a major cause of early morbidity and mortality in patients after lung transplantation. The etiology and pathophysiology of PGD is not fully characterized and whether intraoperative fluid administration increases the risk for PGD remains unclear from previous studies. Therefore, we tested the hypothesis that increased total intraoperative fluid volume during lung transplantation is associated with the development of grade-3 PGD.
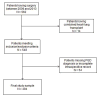
Methods: This retrospective cohort analysis included patients who had lung transplantation at the Cleveland Clinic between January 2009 and June 2013. We used multivariable logistic regression with adjustment for donor, recipient, and perioperative confounding factors to examine the association between total intraoperative fluid administration and development of grade-3 PGD in the initial 72 postoperative hours. Secondary outcomes included time to initial extubation and intensive care unit length of stay.
Results: Grade-3 PGD occurred in 123 of 494 patients (25%) who had lung transplantation. Patients with grade-3 PGD received a larger volume of intraoperative fluid (median 5.0 [3.8, 7.5] L) than those without grade-3 PGD (3.9 [2.8, 5.2] L). Each intraoperative liter of fluid increased the odds of grade-3 PGD by approximately 22% (adjusted odds ratio, 1.22; 95% confidence interval [CI], 1.12-1.34; P <0.001). The volume of transfused red blood cell concentrate was associated with grade-3 PGD (1.1 [0.0, 1.8] L for PGD-3 vs 0.4 [0.0, 1.1 for nongrade-3 PGD] L; adjusted odds ratio, 1.7; 95% CI, 1.08-2.7; P = 0.002). Increased fluid administration was associated with longer intensive care unit stay (adjusted hazard ratio, 0.92; 97.5% CI, 0.88-0.97; P < 0.001) but not with time to initial tracheal extubation (hazard ratio, 0.97; 97.5% CI, 0.93-1.02; P = 0.17).
Conclusions: Increased intraoperative fluid volume is associated with the most severe form of PGD after lung transplant surgery. Limiting fluid administration may reduce the risk for development of grade-3 PGD and thus improve early postoperative morbidity and mortality after lung transplantation.
Conflict of interest statement
The authors declare no conflicts of interest.
Figures
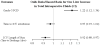
Comment in
-
Lung Transplantation Is Much More Than Lungs and Fluids.Anesth Analg. 2016 Sep;123(3):794-5. doi: 10.1213/ANE.0000000000001375. Anesth Analg. 2016. PMID: 27258071 No abstract available.
-
In Response.Anesth Analg. 2016 Sep;123(3):795-6. doi: 10.1213/ANE.0000000000001374. Anesth Analg. 2016. PMID: 27537765 Free PMC article. No abstract available.
References
-
- Christie J, Sager J, Kimmel S, Vivek A, Gaughan C, Blumental N, Kotloff R. Impact of primary graft failure on outcomes following lung transplantation. Chest. 2005;127:161–165. - PubMed
-
- Christie JD, Carby M, Bag R, Corris P, Hertz M, Weill D. Report of the ISHLT working group on primary lung graft dysfunction: Part II Definition. J Heart Lung Transplant. 2005;24:1454–1459. - PubMed
-
- Prekker M, Nath D, Walker A, Johnson A, Hertz M, Herrington C, Radosevich D, Dahlberg P. Validation of the Proposed International Society for Heart and Lung Transplantation Grading System for Primary Graft Dysfunction After Lung Transplantation. The J Heart and Lung Transplant. 2006;25(4):371–78. - PubMed
-
- Christie J, Bellamy S, Ware L, Lederer D, Hadjiliadis D, Lee J, Robinson N, Localio A, Wille K, Lama V, Palmer S, Orens J, Weinacher A, Crespo M, Demissie E, Kimmel S, Kawut S. Construct validity of the primary graft dysfunction after lung transplantation. J Heart Lung Transplant. 2010;29:1231–9. - PMC - PubMed
-
- Whitson B, Prekker M, Herrington C, Whelan T, Radosevich D, Hertz M, Dahlberg P. Primary graft dysfunction and long-term pulmonary function after lung transplantation. J Heart Lung Transplant. 2007;26:1004–11. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Miscellaneous

