Hepatic and Extrahepatic Insulin Clearance Are Differentially Regulated: Results From a Novel Model-Based Analysis of Intravenous Glucose Tolerance Data
- PMID: 26993071
- PMCID: PMC4878413
- DOI: 10.2337/db15-1373
Hepatic and Extrahepatic Insulin Clearance Are Differentially Regulated: Results From a Novel Model-Based Analysis of Intravenous Glucose Tolerance Data
Abstract
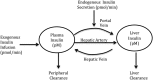
Insulin clearance is a highly variable and important factor that affects circulating insulin concentrations. We developed a novel model-based method to estimate both hepatic and extrahepatic insulin clearance using plasma insulin and C-peptide profiles obtained from the insulin-modified frequently sampled intravenous glucose tolerance test. Data from 100 African immigrants without diabetes (mean age 38 years, body weight 81.7 kg, fasting plasma glucose concentration 83 mg/dL, and fasting insulin concentration 37 pmol/L) were used. Endogenous insulin secretion (calculated by C-peptide deconvolution) and insulin infusion rates were used as inputs to a new two-compartment model of insulin kinetics and hepatic and extrahepatic clearance parameters were estimated. Good agreement between modeled and measured plasma insulin profiles was observed (mean normalized root mean square error 6.8%), and considerable intersubject variability in parameters of insulin clearance among individuals was identified (the mean [interquartile range] for hepatic extraction was 25.8% [32.7%], and for extrahepatic insulin clearance was 20.7 mL/kg/min [11.7 mL/kg/min]). Parameters of insulin clearance were correlated with measures of insulin sensitivity and acute insulin response to glucose. The method described appears promising for future research aimed at characterizing variability in insulin clearance and the mechanisms involved in the regulation of insulin clearance.
Trial registration: ClinicalTrials.gov NCT00001853.
© 2016 by the American Diabetes Association. Readers may use this article as long as the work is properly cited, the use is educational and not for profit, and the work is not altered.
Figures



References
-
- Kahn SE. The relative contributions of insulin resistance and beta-cell dysfunction to the pathophysiology of type 2 diabetes. Diabetologia 2003;46:3–19 - PubMed
-
- DeFronzo RA, Tobin JD, Andres R. Glucose clamp technique: a method for quantifying insulin secretion and resistance. Am J Physiol 1979;237:E214–E223 - PubMed
-
- Kahn SE, Prigeon RL, McCulloch DK, et al. . Quantification of the relationship between insulin sensitivity and beta-cell function in human subjects. Evidence for a hyperbolic function. Diabetes 1993;42:1663–1672 - PubMed
-
- Mittelman SD, Van Citters GW, Kim SP, et al. . Longitudinal compensation for fat-induced insulin resistance includes reduced insulin clearance and enhanced beta-cell response. Diabetes 2000;49:2116–2125 - PubMed
MeSH terms
Substances
Associated data
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

