Rationing tests for drug-resistant tuberculosis - who are we prepared to miss?
- PMID: 27005771
- PMCID: PMC4804634
- DOI: 10.1186/s12916-016-0576-8
Rationing tests for drug-resistant tuberculosis - who are we prepared to miss?
Abstract
Background: Early identification of patients with drug-resistant tuberculosis (DR-TB) increases the likelihood of treatment success and interrupts transmission. Resource-constrained settings use risk profiling to ration the use of drug susceptibility testing (DST). Nevertheless, no studies have yet quantified how many patients with DR-TB this strategy will miss.
Methods: A total of 1,545 subjects, who presented to Lima health centres with possible TB symptoms, completed a clinic-epidemiological questionnaire and provided sputum samples for TB culture and DST. The proportion of drug resistance in this population was calculated and the data was analysed to demonstrate the effect of rationing tests to patients with multidrug-resistant TB (MDR-TB) risk factors on the number of tests needed and corresponding proportion of missed patients with DR-TB.
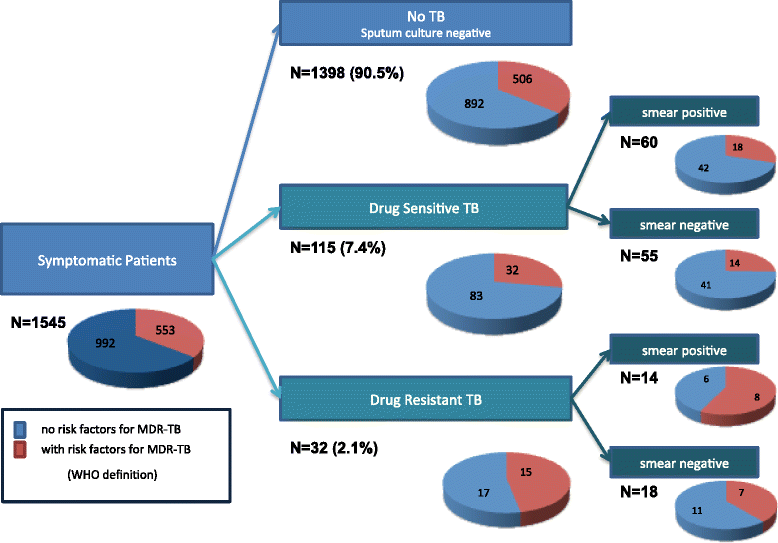
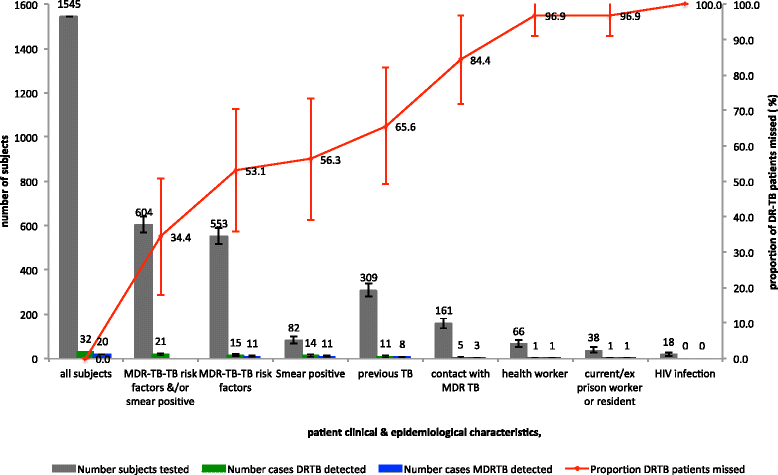
Results: Overall, 147/1,545 (9.5%) subjects had culture-positive TB, of which 32 (21.8%) had DR-TB (MDR, 13.6%; isoniazid mono-resistant, 7.5%; rifampicin mono-resistant, 0.7%). A total of 553 subjects (35.8%) reported one or more MDR-TB risk factors; of these, 506 (91.5%; 95% CI, 88.9-93.7%) did not have TB, 32/553 (5.8%; 95% CI, 3.4-8.1%) had drug-susceptible TB, and only 15/553 (2.7%; 95% CI, 1.5-4.4%) had DR-TB. Rationing DST to those with an MDR-TB risk factor would have missed more than half of the DR-TB population (17/32, 53.2%; 95% CI, 34.7-70.9).
Conclusions: Rationing DST based on known MDR-TB risk factors misses an unacceptable proportion of patients with drug-resistance in settings with ongoing DR-TB transmission. Investment in diagnostic services to allow universal DST for people with presumptive TB should be a high priority.
Keywords: Drug Susceptibility Testing; Microscopic-observation drug-susceptibility assay; Multidrug-resistant tuberculosis; Tuberculosis.
Figures
Similar articles
-
Evaluation of microscopic observation drug susceptibility assay for diagnosis of multidrug-resistant tuberculosis in Viet Nam.BMC Infect Dis. 2012 Mar 1;12:49. doi: 10.1186/1471-2334-12-49. BMC Infect Dis. 2012. PMID: 22375832 Free PMC article.
-
MDR/XDR-TB Colour Test for drug susceptibility testing of Mycobacterium tuberculosis, Northwest Ethiopia.Int J Infect Dis. 2020 Jan;90:213-218. doi: 10.1016/j.ijid.2019.10.041. Epub 2019 Nov 2. Int J Infect Dis. 2020. PMID: 31689528
-
Drug susceptibility patterns of Mycobacterium tuberculosis from adults with multidrug-resistant tuberculosis and implications for a household contact preventive therapy trial.BMC Infect Dis. 2021 Feb 24;21(1):205. doi: 10.1186/s12879-021-05884-4. BMC Infect Dis. 2021. PMID: 33627075 Free PMC article.
-
Management of drug-resistant tuberculosis.Int J Tuberc Lung Dis. 2010 Jun;14(6):672-82. Int J Tuberc Lung Dis. 2010. PMID: 20487603 Review.
-
Evolutionary journey of programmatic services and treatment outcomes among drug resistant tuberculosis (DR-TB) patients under National TB Elimination Programme in India (2005-2020).Expert Rev Respir Med. 2021 Jul;15(7):885-898. doi: 10.1080/17476348.2021.1850277. Epub 2021 Jan 21. Expert Rev Respir Med. 2021. PMID: 33307889 Review.
Cited by
-
Diagnosis of opportunistic infections: HIV co-infections - tuberculosis.Curr Opin HIV AIDS. 2017 Mar;12(2):129-138. doi: 10.1097/COH.0000000000000345. Curr Opin HIV AIDS. 2017. PMID: 28059955 Free PMC article. Review.
-
Uniting to end the TB epidemic: advances in disease control from prevention to better diagnosis and treatment.BMC Med. 2016 Mar 23;14:47. doi: 10.1186/s12916-016-0599-1. BMC Med. 2016. PMID: 27004971 Free PMC article.
-
Evaluation of Xpert MTB-RIF guided diagnosis and treatment of rifampicin-resistant tuberculosis in Indonesia: A retrospective cohort study.PLoS One. 2019 Feb 28;14(2):e0213017. doi: 10.1371/journal.pone.0213017. eCollection 2019. PLoS One. 2019. PMID: 30818352 Free PMC article.
References
-
- World Health Organization . Global tuberculosis report. Geneva: WHO; 2015.
-
- Laboratory Services in TB Control. Parts I, II, and III. Publication No. WHO/tb/98.258. Geneva: WHO; 1998
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical