Efficacy of CD34+ Stem Cell Therapy in Nonischemic Dilated Cardiomyopathy Is Absent in Patients With Diabetes but Preserved in Patients With Insulin Resistance
- PMID: 27025690
- PMCID: PMC4835245
- DOI: 10.5966/sctm.2015-0172
Efficacy of CD34+ Stem Cell Therapy in Nonischemic Dilated Cardiomyopathy Is Absent in Patients With Diabetes but Preserved in Patients With Insulin Resistance
Abstract
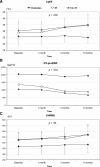
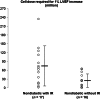
We evaluated the association of diabetes and insulin resistance with the response to cell therapy in patients with nonischemic dilated cardiomyopathy (DCM). A total of 45 outpatients with DCM received granulocyte colony-stimulating factor for 5 days. CD34(+) cells were then collected by apheresis and injected transendocardially. Twelve patients had diabetes mellitus (DM group), 17 had insulin resistance (IR group), and 16 displayed normal glucose metabolism (no-IR group). After stimulation, we found higher numbers of CD34(+) cells in the IR group (94 ± 73 × 10(6) cells per liter) than in the no-IR group (54 ± 35 × 10(6) cells per liter) or DM group (31 ± 20 × 10(6) cells per liter; p = .005). Similarly, apheresis yielded the highest numbers of CD34(+) cells in the IR group (IR group, 216 ± 110 × 10(6) cells; no-IR group, 127 ± 82 × 10(6) cells; DM group, 77 ± 83 × 10(6) cells; p = .002). Six months after cell therapy, we found an increase in left ventricular ejection fraction in the IR group (+5.6% ± 6.9%) and the no-IR group (+4.4% ± 7.2%) but not in the DM group (-0.9% ± 5.4%; p = .035). The N-terminal pro-brain natriuretic peptide levels decreased in the IR and no-IR groups, but not in the DM group (-606 ± 850 pg/ml; -698 ± 1,105 pg/ml; and +238 ± 963 pg/ml, respectively; p = .034). Transendocardial CD34(+) cell therapy appears to be ineffective in DCM patients with diabetes. IR was associated with improved CD34(+) stem cell mobilization and a preserved clinical response to cell therapy.
Significance: The present study is the first clinical study directly evaluating the effects of altered glucose metabolism on the efficacy of CD34(+) stem cell therapy in patients with nonischemic dilated cardiomyopathy. The results offer critical insights into the physiology of stem cell mobilization in heart failure and possibly an explanation for the often conflicting results obtained with stem cell therapy for heart failure. These results demonstrate that patients with dilated cardiomyopathy and diabetes do not benefit from autologous CD34(+) cell therapy. This finding could serve as a useful tool when selecting heart failure patients for future clinical studies in the field of stem cell therapy.
Keywords: Diabetes; Dilated cardiomyopathy; Insulin resistance; Stem cells.
©AlphaMed Press.
Figures

References
-
- Vrtovec B, Poglajen G, Lezaic L, et al. Comparison of transendocardial and intracoronary CD34+ cell transplantation in patients with nonischemic dilated cardiomyopathy. Circulation. 2013;128(suppl 1):S42–S49. - PubMed
-
- Vrtovec B, Poglajen G, Lezaic L, et al. Effects of intracoronary CD34+ stem cell transplantation in nonischemic dilated cardiomyopathy patients: 5-year follow-up. Circ Res. 2013;112:165–173. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

