Effect of restrictive versus liberal transfusion strategies on outcomes in patients with cardiovascular disease in a non-cardiac surgery setting: systematic review and meta-analysis
- PMID: 27026510
- PMCID: PMC4817242
- DOI: 10.1136/bmj.i1351
Effect of restrictive versus liberal transfusion strategies on outcomes in patients with cardiovascular disease in a non-cardiac surgery setting: systematic review and meta-analysis
Abstract
Objective: To compare patient outcomes of restrictive versus liberal blood transfusion strategies in patients with cardiovascular disease not undergoing cardiac surgery.
Design: Systematic review and meta-analysis.
Data sources: Randomised controlled trials involving a threshold for red blood cell transfusion in hospital. We searched (to 2 November 2015) CENTRAL, Medline, Embase, CINAHL, PubMed, LILACS, NHSBT Transfusion Evidence Library, ClinicalTrials.gov, WHO International Clinical Trials Registry Platform, ISRCTN Register, and EU Clinical Trials Register. Authors were contacted for data whenever possible.
Trial selection: Published and unpublished randomised controlled trials comparing a restrictive with liberal transfusion threshold and that included patients with cardiovascular disease.
Data extraction and synthesis: Data extraction was completed in duplicate. Risk of bias was assessed using Cochrane methods. Relative risk ratios with 95% confidence intervals were presented in all meta-analyses. Mantel-Haenszel random effects models were used to pool risk ratios.
Main outcome measures: 30 day mortality, and cardiovascular events.
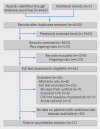
Results: 41 trials were identified; of these, seven included data on patients with cardiovascular disease. Data from a further four trials enrolling patients with cardiovascular disease were obtained from the authors. In total, 11 trials enrolling patients with cardiovascular disease (n=3033) were included for meta-analysis (restrictive transfusion, n=1514 patients; liberal transfusion, n=1519). The pooled risk ratio for the association between transfusion thresholds and 30 day mortality was 1.15 (95% confidence interval 0.88 to 1.50, P=0.50), with little heterogeneity (I(2)=14%). The risk of acute coronary syndrome in patients managed with restrictive compared with liberal transfusion was increased (nine trials; risk ratio 1.78, 95% confidence interval 1.18 to 2.70, P=0.01, I(2)=0%).
Conclusions: The results show that it may not be safe to use a restrictive transfusion threshold of less than 80 g/L in patients with ongoing acute coronary syndrome or chronic cardiovascular disease. Effects on mortality and other outcomes are uncertain. These data support the use of a more liberal transfusion threshold (>80 g/L) for patients with both acute and chronic cardiovascular disease until adequately powered high quality randomised trials have been undertaken in patients with cardiovascular disease.
Registration: PROSPERO CRD42014014251.
Published by the BMJ Publishing Group Limited. For permission to use (where not already granted under a licence) please go to http://group.bmj.com/group/rights-licensing/permissions.
Conflict of interest statement
Competing interests: All authors have completed the ICMJE uniform disclosure form at
Figures


Similar articles
-
Transfusion thresholds for guiding red blood cell transfusion.Cochrane Database Syst Rev. 2021 Dec 21;12(12):CD002042. doi: 10.1002/14651858.CD002042.pub5. Cochrane Database Syst Rev. 2021. PMID: 34932836 Free PMC article.
-
Restrictive versus liberal red blood cell transfusion strategies for people with haematological malignancies treated with intensive chemotherapy or radiotherapy, or both, with or without haematopoietic stem cell support.Cochrane Database Syst Rev. 2017 Jan 27;1(1):CD011305. doi: 10.1002/14651858.CD011305.pub2. Cochrane Database Syst Rev. 2017. Update in: Cochrane Database Syst Rev. 2024 May 23;5:CD011305. doi: 10.1002/14651858.CD011305.pub3. PMID: 28128441 Free PMC article. Updated.
-
Non-pharmacological interventions for preventing delirium in hospitalised non-ICU patients.Cochrane Database Syst Rev. 2021 Jul 19;7(7):CD013307. doi: 10.1002/14651858.CD013307.pub2. Cochrane Database Syst Rev. 2021. PMID: 34280303 Free PMC article.
-
Transfusion thresholds and other strategies for guiding allogeneic red blood cell transfusion.Cochrane Database Syst Rev. 2016 Oct 12;10(10):CD002042. doi: 10.1002/14651858.CD002042.pub4. Cochrane Database Syst Rev. 2016. Update in: Cochrane Database Syst Rev. 2021 Dec 21;12:CD002042. doi: 10.1002/14651858.CD002042.pub5. PMID: 27731885 Free PMC article. Updated.
-
Preoperative blood transfusions for sickle cell disease.Cochrane Database Syst Rev. 2016 Apr 6;4(4):CD003149. doi: 10.1002/14651858.CD003149.pub3. Cochrane Database Syst Rev. 2016. Update in: Cochrane Database Syst Rev. 2020 Jul 2;7:CD003149. doi: 10.1002/14651858.CD003149.pub4. PMID: 27049331 Free PMC article. Updated.
Cited by
-
Liberal versus restrictive red blood cell transfusion strategy in sepsis or septic shock: a systematic review and meta-analysis of randomized trials.Crit Care. 2019 Jul 25;23(1):262. doi: 10.1186/s13054-019-2543-1. Crit Care. 2019. PMID: 31345236 Free PMC article.
-
Systematic reviews and meta-analyses comparing mortality in restrictive and liberal haemoglobin thresholds for red cell transfusion: protocol for an overview of systematic reviews.BMJ Open. 2019 Aug 24;9(8):e029828. doi: 10.1136/bmjopen-2019-029828. BMJ Open. 2019. PMID: 31446415 Free PMC article.
-
Impact of blood transfusion on mortality and rebleeding in gastrointestinal bleeding: an 8-year cohort from a tertiary care center.Ann Gastroenterol. 2024 May-Jun;37(3):303-312. doi: 10.20524/aog.2024.0877. Epub 2024 Apr 10. Ann Gastroenterol. 2024. PMID: 38779640 Free PMC article.
-
Alternative blood transfusion triggers: a narrative review.BMC Anesthesiol. 2024 Feb 23;24(1):71. doi: 10.1186/s12871-024-02447-3. BMC Anesthesiol. 2024. PMID: 38395758 Free PMC article. Review.
-
Management of Patient with Simultaneous Overt Gastrointestinal Bleeding and Myocardial Infarction with ST-Segment Elevation - Priority Endoscopy.Vasc Health Risk Manag. 2021 Mar 31;17:123-133. doi: 10.2147/VHRM.S292253. eCollection 2021. Vasc Health Risk Manag. 2021. PMID: 33833517 Free PMC article.
References
-
- British Heart Foundation. Cardiovascular Disease Statistics 2015. Oxford; 2015. https://www.bhf.org.uk/publications/statistics/cvd-stats-2015
-
- Vincent JL, Baron J-F, Reinhart K, et al. ABC (Anemia and Blood Transfusion in Critical Care) Investigators. Anemia and blood transfusion in critically ill patients. JAMA 2002;288:1499-507. 10.1001/jama.288.12.1499. pmid:12243637. - DOI - PubMed
-
- Carson J, Duff A, Poses R, et al. Effect of anaemia and cardiovascular disease on surgical mortality and morbidity. Lancet 1996;348:1055-60. 10.1016/S0140-6736(96)04330-9. pmid:8874456. - DOI - PubMed
-
- Wu W-C, Rathore SS, Wang Y, Radford MJ, Krumholz HM. Blood transfusion in elderly patients with acute myocardial infarction. N Engl J Med 2001;345:1230-6. 10.1056/NEJMoa010615. pmid:11680442. - DOI - PubMed
-
- Horwich TB, Fonarow GC, Hamilton MA, MacLellan WR, Borenstein J. Anemia is associated with worse symptoms, greater impairment in functional capacity and a significant increase in mortality in patients with advanced heart failure. J Am Coll Cardiol 2002;39:1780-6. 10.1016/S0735-1097(02)01854-5. pmid:12039491. - DOI - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
