WAT apoC-I secretion: role in delayed chylomicron clearance in vivo and ex vivo in WAT in obese subjects
- PMID: 27040450
- PMCID: PMC4878191
- DOI: 10.1194/jlr.P064170
WAT apoC-I secretion: role in delayed chylomicron clearance in vivo and ex vivo in WAT in obese subjects
Abstract
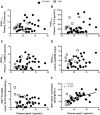
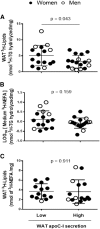
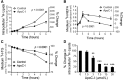
Reduced white adipose tissue (WAT) LPL activity delays plasma clearance of TG-rich lipoproteins (TRLs). We reported the secretion of apoC-I, an LPL inhibitor, from WAT ex vivo in women. Therefore we hypothesized that WAT-secreted apoC-I associates with reduced WAT LPL activity and TRL clearance. WAT apoC-I secretion averaged 86.9 ± 31.4 pmol/g/4 h and 74.1 ± 36.6 pmol/g/4 h in 28 women and 11 men with BMI ≥27 kg/m(2), respectively, with no sex differences. Following the ingestion of a (13)C-triolein-labeled high-fat meal, subjects with high WAT apoC-I secretion (above median) had delayed postprandial plasma clearance of dietary TRLs, assessed from plasma (13)C-triolein-labeled TGs and apoB48. They also had reduced hydrolysis and storage of synthetic (3)H-triolein-labeled ((3)H)-TRLs in WAT ex vivo (i.e., in situ LPL activity). Adjusting for WAT in situ LPL activity eliminated group differences in chylomicron clearance; while adjusting for plasma apoC-I, (3)H-NEFA uptake by WAT, or body composition did not. apoC-I inhibited in situ LPL activity in adipocytes in both a concentration- and time-dependent manner. There was no change in postprandial WAT apoC-I secretion. WAT apoC-I secretion may inhibit WAT LPL activity and promote delayed chylomicron clearance in overweight and obese subjects. We propose that reducing WAT apoC-I secretion ameliorates postprandial TRL clearance in humans.
Keywords: adipocytes; apolipoprotein C-I; cardiometabolic risk; fat storage; lipase/lipoprotein; lipolysis and fatty acid metabolism; obesity; triglyceride-rich lipoprotein; triglycerides; white adipose tissue.
Copyright © 2016 by the American Society for Biochemistry and Molecular Biology, Inc.
Figures


Similar articles
-
Enrichment of Triglyceride-Rich Lipoproteins with Apolipoprotein C-I Is Positively Associated with Their Delayed Plasma Clearance Independently of Other Transferable Apolipoproteins in Postmenopausal Overweight and Obese Women.J Nutr. 2017 May;147(5):754-762. doi: 10.3945/jn.116.242750. Epub 2017 Mar 29. J Nutr. 2017. PMID: 28356429
-
White adipose tissue apolipoprotein C-I secretion in relation to delayed plasma clearance of dietary fat in humans.Arterioscler Thromb Vasc Biol. 2012 Nov;32(11):2785-93. doi: 10.1161/ATVBAHA.112.300306. Epub 2012 Sep 20. Arterioscler Thromb Vasc Biol. 2012. PMID: 22995522
-
Low density lipoprotein delays clearance of triglyceride-rich lipoprotein by human subcutaneous adipose tissue.J Lipid Res. 2013 May;54(5):1466-76. doi: 10.1194/jlr.P023176. Epub 2013 Feb 17. J Lipid Res. 2013. PMID: 23417739 Free PMC article.
-
Omega-3 fatty acids eicosapentaenoic acid and docosahexaenoic acid and their mechanisms of action on apolipoprotein B-containing lipoproteins in humans: a review.Lipids Health Dis. 2017 Aug 10;16(1):149. doi: 10.1186/s12944-017-0541-3. Lipids Health Dis. 2017. PMID: 28797250 Free PMC article. Review.
-
Apolipoprotein C-II: New findings related to genetics, biochemistry, and role in triglyceride metabolism.Atherosclerosis. 2017 Dec;267:49-60. doi: 10.1016/j.atherosclerosis.2017.10.025. Epub 2017 Oct 20. Atherosclerosis. 2017. PMID: 29100061 Free PMC article. Review.
Cited by
-
The Association of Polyunsaturated Fatty Acid δ-5-Desaturase Activity with Risk Factors for Type 2 Diabetes Is Dependent on Plasma ApoB-Lipoproteins in Overweight and Obese Adults.J Nutr. 2019 Jan 1;149(1):57-67. doi: 10.1093/jn/nxy238. J Nutr. 2019. PMID: 30535058 Free PMC article.
-
Lower plasma PCSK9 in normocholesterolemic subjects is associated with upregulated adipose tissue surface-expression of LDLR and CD36 and NLRP3 inflammasome.Physiol Rep. 2021 Feb;9(3):e14721. doi: 10.14814/phy2.14721. Physiol Rep. 2021. PMID: 33527668 Free PMC article.
-
Diabetes and dyslipidemia: characterizing lipoprotein metabolism.Diabetes Metab Syndr Obes. 2017 Jul 28;10:333-343. doi: 10.2147/DMSO.S115855. eCollection 2017. Diabetes Metab Syndr Obes. 2017. PMID: 28814891 Free PMC article. Review.
-
Role of apolipoprotein C1 in lipoprotein metabolism, atherosclerosis and diabetes: a systematic review.Cardiovasc Diabetol. 2022 Dec 5;21(1):272. doi: 10.1186/s12933-022-01703-5. Cardiovasc Diabetol. 2022. PMID: 36471375 Free PMC article.
-
Plasma proteoforms of apolipoproteins C-I and C-II are associated with plasma lipids in the Multi-Ethnic Study of Atherosclerosis.J Lipid Res. 2022 Sep;63(9):100263. doi: 10.1016/j.jlr.2022.100263. Epub 2022 Aug 9. J Lipid Res. 2022. PMID: 35952903 Free PMC article.
References
-
- Genest J., McPherson R., Frohlich J., Anderson T., Campbell N., Carpentier A., Couture P., Dufour R., Fodor G., Francis G. A., et al. . 2009. 2009 Canadian Cardiovascular Society/Canadian guidelines for the diagnosis and treatment of dyslipidemia and prevention of cardiovascular disease in the adult - 2009 recommendations. Can. J. Cardiol. 25: 567–579. - PMC - PubMed
-
- Miller M., Stone N. J., Ballantyne C., Bittner V., Criqui M. H., Ginsberg H. N., Goldberg A. C., Howard W. J., Jacobson M. S., Kris-Etherton P. M., et al. . 2011. Triglycerides and cardiovascular disease: a scientific statement from the American Heart Association. Circulation. 123: 2292–2333. - PubMed
-
- Sarwar N., Danesh J., Eiriksdottir G., Sigurdsson G., Wareham N., Bingham S., Boekholdt S. M., Khaw K. T., and Gudnason V.. 2007. Triglycerides and the risk of coronary heart disease: 10,158 incident cases among 262,525 participants in 29 Western prospective studies. Circulation. 115: 450–458. - PubMed
-
- Murad M. H., Hazem A., Coto-Yglesias F., Dzyubak S., Gupta S., Bancos I., Lane M. A., Erwin P. J., Berglund L., Elraiyah T., et al. . 2012. The association of hypertriglyceridemia with cardiovascular events and pancreatitis: a systematic review and meta-analysis. BMC Endocr. Disord. 12: 2. - PMC - PubMed
-
- Bansal S., Buring J. E., Rifai N., Mora S., Sacks F. M., and Ridker P. M.. 2007. Fasting compared with nonfasting triglycerides and risk of cardiovascular events in women. JAMA. 298: 309–316. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Miscellaneous

