Results from the Survey of Antibiotic Resistance (SOAR) 2009-11 in Vietnam
- PMID: 27048586
- PMCID: PMC4890351
- DOI: 10.1093/jac/dkw069
Results from the Survey of Antibiotic Resistance (SOAR) 2009-11 in Vietnam
Abstract
Objectives: To investigate the susceptibility of respiratory tract infection pathogens collected between 2009 and 2011 from the SOAR study in Vietnam.
Methods: MICs were determined using Etest(®) and susceptibility was assessed using CLSI, EUCAST and pharmacokinetic/pharmacodynamic (PK/PD) breakpoints.
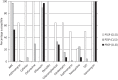
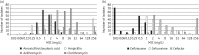
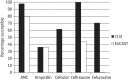
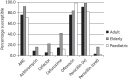
Results: Two hundred and eighty-nine Streptococcus pneumoniae and 195 Haemophilus influenzae were collected from 11 centres. Overall, 4.8% of S. pneumoniae were penicillin susceptible (CLSI oral and EUCAST breakpoints). Using CLSI intravenous breakpoints, 86.9% were penicillin susceptible. Susceptibility to high-dose amoxicillin/clavulanic acid (or amoxicillin) using PK/PD breakpoints, cefuroxime (using CLSI or PK/PD breakpoints), cefaclor (CLSI breakpoint) and azithromycin (CLSI breakpoint) was 96.9%, 18.7%, 8% and 4.2%, respectively. Ofloxacin susceptibility was 93.4% by CLSI but 0% by EUCAST. All S. pneumoniae were fully vancomycin susceptible. S. pneumoniae from children were significantly less susceptible to most antimicrobials than those from the elderly. For ofloxacin, however, the reverse was true.Among H. influenzae isolates, 40.5% produced β-lactamase and 13.8% were β-lactamase negative but ampicillin resistant (BLNAR) by CLSI. H. influenzae were highly susceptible (97.4%) in vitro to amoxicillin/clavulanic acid and also to ceftriaxone by CLSI and PK/PD breakpoints but not EUCAST breakpoints. However, BLNAR isolates should be considered clinically resistant, with susceptibility reduced to 84.1%. With EUCAST breakpoints, amoxicillin/clavulanic acid susceptibility was lower, at 63.1%. Azithromycin susceptibility was 79.5% (CLSI).
Conclusions: Resistance to antibacterials in Vietnam was high, with amoxicillin/clavulanic acid being the most active agent. Ceftriaxone was highly active against H. influenzae while ofloxacin appeared highly active against S. pneumoniae using CLSI but not by EUCAST breakpoints. Ongoing surveillance through SOAR will further assist in understanding susceptibility trends over time.
© The Author 2016. Published by Oxford University Press on behalf of the British Society for Antimicrobial Chemotherapy. All rights reserved. For Permissions, please e-mail: journals.permissions@oup.com.
Figures


References
-
- Clinical and Laboratory Standards Institute. Performance Standards for Antimicrobial Disk Susceptibility Tests—Eleventh Edition: Approved Standard M02-A11. CLSI, Wayne, PA, USA, 2012.
-
- Clinical and Laboratory Standards Institute. Performance Standards for Antimicrobial Susceptibility Testing: Twenty-fourth Informational Supplement M100-S24. CLSI, Wayne, PA, USA, 2014.
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Molecular Biology Databases

