Activity of 8F4, a T-cell receptor-like anti-PR1/HLA-A2 antibody, against primary human AML in vivo
- PMID: 27055866
- PMCID: PMC4935597
- DOI: 10.1038/leu.2016.57
Activity of 8F4, a T-cell receptor-like anti-PR1/HLA-A2 antibody, against primary human AML in vivo
Abstract
The PR1 peptide, derived from the leukemia-associated antigens proteinase 3 and neutrophil elastase, is overexpressed on HLA-A2 in acute myeloid leukemia (AML). We developed a high-affinity T-cell receptor-like murine monoclonal antibody, 8F4, that binds to the PR1/HLA-A2 complex, mediates lysis of AML and inhibits leukemia colony formation. Here, we explored whether 8F4 was active in vivo against chemotherapy-resistant AML, including secondary AML. In a screening model, coincubation of AML with 8F4 ex vivo prevented engraftment of all tested AML subtypes in immunodeficient NSG (NOD scid IL-2 receptor γ-chain knockout) mice. In a treatment model of established human AML, administration of 8F4 significantly reduced or eliminated AML xenografts and extended survival compared with isotype antibody-treated mice. Moreover, in secondary transfer experiments, mice inoculated with bone marrow from 8F4-treated mice showed no evidence of AML engraftment, supporting the possible activity of 8F4 against the subset of AML with self-renewing potential. Our data provide evidence that 8F4 antibody is highly active in AML, including chemotherapy-resistant disease, supporting its potential use as a therapeutic agent in patients with AML.
Conflict of interest statement
Dr. Jeffrey Molldrem and Dr. Anna Sergeeva are inventors on a related patent and they receive royalty payments.
Figures

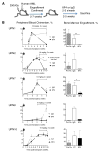


References
-
- Champlin R, Khouri I, Kornblau S, Marini F, Anderlini P, Ueno NT, et al. Allogeneic hematopoietic transplantation as adoptive immunotherapy. Induction of graft-versus-malignancy as primary therapy. Hematol Oncol Clin North Am. 1999 Oct;13(5):1041–1057. vii–viii. - PubMed
-
- Molldrem J, Dermime S, Parker K, Jiang YZ, Mavroudis D, Hensel N, et al. Targeted T-cell therapy for human leukemia: cytotoxic T lymphocytes specific for a peptide derived from proteinase 3 preferentially lyse human myeloid leukemia cells. Blood. 1996 Oct 1;88( 7):2450–2457. - PubMed
-
- Rusakiewicz S, Molldrem JJ. Immunotherapeutic peptide vaccination with leukemia-associated antigens. Curr Opin Immunol. 2006 Oct;18(5):599–604. - PubMed
-
- Denkberg G, Cohen CJ, Lev A, Chames P, Hoogenboom HR, Reiter Y. Direct visualization of distinct T cell epitopes derived from a melanoma tumor-associated antigen by using human recombinant antibodies with MHC- restricted T cell receptor-like specificity. Proc Natl Acad Sci U S A. 2002 Jul 9;99(14):9421–9426. - PMC - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Research Materials

