Clinical effects of topical antifungal therapy in chronic rhinosinusitis: a randomized, double-blind, placebo-controlled trial of intranasal fluconazole
- PMID: 27065776
- PMCID: PMC4822190
- DOI: 10.17179/excli2015-678
Clinical effects of topical antifungal therapy in chronic rhinosinusitis: a randomized, double-blind, placebo-controlled trial of intranasal fluconazole
Abstract
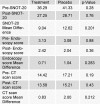
Several studies have been in favor of fungi as a possible pathogenesis of chronic rhinosinusitis (CRS); however, to date, there is no scientific consensus about the use of antifungal agents in disease management. The aim of the present study was to investigate the efficacy of intranasal fluconazole in improving disease symptoms and objective outcomes of patients with CRS. A randomized, double-blind, placebo-controlled study was conducted on 54 patients who were diagnosed with CRS and had not been responsive to routine medical treatments. They were randomly assigned to receive either fluconazole nasal drop 0.2 % or placebo in addition to the standard regimen for a duration of 8 weeks. Patients' outcomes were evaluated according to Sino-Nasal Outcome Test 20 (SNOT-20), endoscopic scores, and Computed Tomography (CT) scores. No statistically significant difference was found in SNOT-20 (p = 0.201), endoscopic (p = 0.283), and CT scores (p = 0.212) of the patients at baseline and after 8-week course of treatment between drug and placebo group. Similar to many studies, the use of topical antifungal treatment for patients with CRS was not shown to be significantly effective. However, further studies are needed to obtain high levels of consistent evidence in order to arrive at a decision whether antifungal therapy is effective in management of CRS or not.
Keywords: antifungal therapy; chronic rhinosinusitis; clinical trial; fluconazole.
Figures
References
-
- Abele-Horn M, Kopp A, Sternberg U, Ohly A, Dauber A, Russwurm W, et al. A randomized study comparing fluconazole with amphotericin B/ 5-flucytosine for the treatment of systemic Candida infections in intensive care patients. Infection. 1996;24:426–432. - PubMed
-
- Benninger MS, Ferguson BJ, Hadley JA, Hamilos DL, Jacobs M, Kennedy DW, et al. Adult chronic rhinosinusitis: definitions, diagnosis, epidemiology, and pathophysiology. Otolaryngol Head Neck Surg. 2003;129:S1–32. - PubMed
-
- Bhattacharyya N, Orlandi RR, Grebner J, Martinson M. Cost burden of chronic rhinosinusitis: a claims-based study. Otolaryngol Head Neck Surg. 2011;144:440–445. - PubMed
-
- Ebbens FA, Georgalas C, Rinia AB, van Drunen CM, Lund VJ, Fokkens WJ. The fungal debate: where do we stand today? Rhinology. 2007;45:178–189. - PubMed
-
- Ebbens FA, Scadding GK, Badia L, Hellings PW, Jorissen M, Mullol J, et al. Amphotericin B nasal lavages: not a solution for patients with chronic rhinosinusitis. J Allergy Clin Immunol. 2006;118:1149–1156. - PubMed
LinkOut - more resources
Full Text Sources