Transforming the Patient Role to Achieve Better Outcomes Through a Patient Empowerment Program: A Randomized Wait-List Control Trial Protocol
- PMID: 27103306
- PMCID: PMC4858596
- DOI: 10.2196/resprot.5376
Transforming the Patient Role to Achieve Better Outcomes Through a Patient Empowerment Program: A Randomized Wait-List Control Trial Protocol
Abstract
Background: In the patient-centered medical home model of health care, both health care providers (HCPs) and patients must understand their respective roles and responsibilities, view the other as a partner, and use communication skills that promote shared decision making. This is particularly necessary in chronic conditions where outcomes depend on behavior change and in underserved populations where the burden of chronic disease is high.
Objective: The objectives of this study are to determine if a Patient Empowerment Program (PEP) (1) is acceptable to patients and feasible across multiple clinical sites; (2) will increase patient preference for control in medical decision making, improve patient perceptions of patient-HCP communication, and increase patient activation; (3) is associated with an increase in diabetes self-management behaviors; and (4) has an effect on hemoglobin A1c (HbA1c) level.
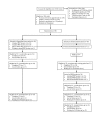
Methods: This study recruited English-speaking adult patients with type 2 diabetes mellitus from three urban clinical sites in New York City and randomized them to an immediate intervention group that completed the PEP intervention or a deferred intervention group that served as a wait-list control and completed the PEP intervention after 3-4 months. The PEP intervention consists of two facilitated small group sessions. Session 1 focuses on defining HCP and patient roles in the medical encounter by introducing ideal communication behaviors in each role and by providing both positive and negative examples of patient-HCP encounters. Session 2 focuses on practicing communication skills by role-playing with actors who serve as standardized health care providers. After the role play, participants set goals for their own health care and for future interactions with their HCPs. Outcome measures include the Patient Activation Measure; Ask, Understand, Remember Assessment; Krantz Health Opinion Survey; SF-12v2 Health Survey; Diabetes Self-Management Questionnaire; and HbA1c. These measures will be assessed at the time of enrollment, after the waiting period (deferred intervention only), and then postintervention at 1 week, 3 months, and 6 months.
Results: Study recruitment occurred from November 2014 to June 2015, with a total of 80 patients enrolled. To date, 45 participants have attended at least one session of the PEP intervention. Further intervention sessions and post-intervention follow-up are ongoing, with data collection set to be completed in April 2016 and results of data analysis available by June 2016.
Conclusions: From preliminary participant self-report data, our PEP intervention is acceptable to low-income, low-health literate patients and feasible to hold across multiple clinical sites. Participants have reported learning specific ways to change their behaviors at their next HCP visit (eg, stating their opinions, asking more questions). With the forthcoming quantitative data on participant attitudinal and behavior change, the PEP intervention may ultimately empower participants within the medical encounter and improve health outcomes.
Keywords: health literacy; patient activation; shared decision making.
Conflict of interest statement
Conflicts of Interest: None declared.
Figures
Similar articles
-
Virtualized clinical studies to assess the natural history and impact of gut microbiome modulation in non-hospitalized patients with mild to moderate COVID-19 a randomized, open-label, prospective study with a parallel group study evaluating the physiologic effects of KB109 on gut microbiota structure and function: a structured summary of a study protocol for a randomized controlled study.Trials. 2021 Apr 2;22(1):245. doi: 10.1186/s13063-021-05157-0. Trials. 2021. PMID: 33810796 Free PMC article.
-
A qualitative systematic review of internal and external influences on shared decision-making in all health care settings.JBI Libr Syst Rev. 2012;10(58):4633-4646. doi: 10.11124/jbisrir-2012-432. JBI Libr Syst Rev. 2012. PMID: 27820528
-
Structured, intensive education maximising engagement, motivation and long-term change for children and young people with diabetes: a cluster randomised controlled trial with integral process and economic evaluation - the CASCADE study.Health Technol Assess. 2014 Mar;18(20):1-202. doi: 10.3310/hta18200. Health Technol Assess. 2014. PMID: 24690402 Free PMC article. Clinical Trial.
-
Adult patient access to electronic health records.Cochrane Database Syst Rev. 2021 Feb 26;2(2):CD012707. doi: 10.1002/14651858.CD012707.pub2. Cochrane Database Syst Rev. 2021. PMID: 33634854 Free PMC article.
-
Communication interventions for autism spectrum disorder in minimally verbal children.Cochrane Database Syst Rev. 2018 Nov 5;11(11):CD012324. doi: 10.1002/14651858.CD012324.pub2. Cochrane Database Syst Rev. 2018. PMID: 30395694 Free PMC article.
Cited by
-
Promoting patient participation in healthcare interactions through communication skills training: A systematic review.Patient Educ Couns. 2017 Jul;100(7):1247-1257. doi: 10.1016/j.pec.2017.02.016. Epub 2017 Feb 16. Patient Educ Couns. 2017. PMID: 28238421 Free PMC article.
-
Interventions for increasing the use of shared decision making by healthcare professionals.Cochrane Database Syst Rev. 2018 Jul 19;7(7):CD006732. doi: 10.1002/14651858.CD006732.pub4. Cochrane Database Syst Rev. 2018. PMID: 30025154 Free PMC article.
References
-
- American DA. Economic costs of diabetes in the U.S. in 2012. Diabetes Care. 2013 Apr;36(4):1033–46. doi: 10.2337/dc12-2625. http://europepmc.org/abstract/MED/23468086 dc12-2625 - DOI - PMC - PubMed
-
- City University of New York Campaign Against Diabetes. 2007. [2016-04-06]. Reversing the Diabetes and Obesity Epidemics in New York City https://www.monroecollege.edu/uploadedFiles/_Site_Assets/PDF/diabetes_pr... .
-
- Scholle SH, Torda P, Peikes D, Han E, Genevro J. Patient Centered Medical Home. Rockville, MD: Agency for Healthcare Research and Quality; 2010. [2016-04-06]. Engaging Patients and Families in the Medical Home https://pcmh.ahrq.gov/page/engaging-patients-and-families-medical-home .
-
- Committee on Quality of Healthcare in America . Crossing the Quality Chasm: A New Health System for the 21st Century. Washington (DC): National Academies Press (US); 2001. https://www.nationalacademies.org/hmd/~/media/Files/Report%20Files/2001/... . - PubMed
-
- IOM Executive Office Partnering with Patients to Drive Shared Decisions, Better Value, and Care Improvement: Workshop Proceedings. Building the Patient and Family Advisory Leadership Network for Better Care; 2013; Washington, DC. 2013. Nov 11, p. 205. http://www.nap.edu/
LinkOut - more resources
Full Text Sources
Other Literature Sources
Miscellaneous