Bronchogenic cyst at esophagogastric junction treated by laparoscopic full-thickness resection and hand-sewn closure: a case report
- PMID: 27117265
- PMCID: PMC4848280
- DOI: 10.1186/s40792-016-0168-z
Bronchogenic cyst at esophagogastric junction treated by laparoscopic full-thickness resection and hand-sewn closure: a case report
Abstract
Background: We herein report a case of a bronchogenic cyst arising from the esophagogastric junction treated by laparoscopic full-thickness extirpation. The full-thickness defect was closed by hand sewing a T-shaped line over the gastroendoscope as a bougie to prevent postoperative deformity or stenosis. Partial fundoplication (Toupet fundoplication) was added to prevent reflux.
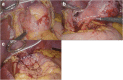
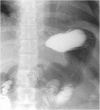
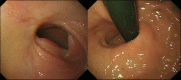
Case presentation: A 32-year-old woman with a body mass index of 43 kg/m(2) was admitted for treatment of a cyst-forming submucosal tumor (60 mm in diameter) on the anterior wall of the esophagogastric junction, which was detected during screening endoscopy before bariatric surgery. The tumor was an extraluminal growing type but exhibited severe erosion at the mucosal site. A cystic tumor such as a duplication cyst, bronchogenic cyst, or cyst-forming gastrointestinal stromal tumor was suspected, and the abovementioned surgery was carried out. The postoperative course was uneventful. The pathological findings revealed the tumor to be a benign bronchogenic cyst. Endoscopic examination 3 months postoperatively showed no deformity or stenosis, and the patient complained of no reflux symptoms.
Conclusion: This procedure may be an efficient option for treatment of submucosal tumors on the esophagogastric junction to maintain function or avoid excessive surgery.
Keywords: Bronchogenic cyst; Esophagogastric junction; Laparoscopic resection.
Figures




Similar articles
-
Laparoscopic surgery for an esophageal duplication cyst using a near-infrared indocyanine green fluorescence system: A case report.Asian J Endosc Surg. 2020 Apr;13(2):211-214. doi: 10.1111/ases.12729. Epub 2019 Jul 1. Asian J Endosc Surg. 2020. PMID: 31264376 Free PMC article.
-
A gastrointestinal stromal tumor at the esophagogastric junction successfully treated by laparoscopic wedge resection with seromuscular layer dissection: a case report.Surg Case Rep. 2015 Dec;1(1):89. doi: 10.1186/s40792-015-0090-9. Epub 2015 Sep 25. Surg Case Rep. 2015. PMID: 26943414 Free PMC article.
-
Subdiaphragmatic bronchogenic cyst at the gastroesophageal junction presenting with Dysphagia: a case report.Surg Laparosc Endosc Percutan Tech. 2013 Aug;23(4):e170-2. doi: 10.1097/SLE.0b013e31828e3e54. Surg Laparosc Endosc Percutan Tech. 2013. PMID: 23917610
-
[Laparoscopic and endoscopic cooperative surgery for gastric tumor--a case report with review of literature].Gan To Kagaku Ryoho. 2010 Nov;37(12):2467-9. Gan To Kagaku Ryoho. 2010. PMID: 21224608 Review. Japanese.
-
[Intrapericardial bronchogenic cyst--a report of two surgical cases].Nihon Kyobu Geka Gakkai Zasshi. 1990 Apr;38(4):660-6. Nihon Kyobu Geka Gakkai Zasshi. 1990. PMID: 2197351 Review. Japanese.
Cited by
-
Intramural bronchogenic cysts of the esophagus and gastroesophageal junction: A case report.Mol Clin Oncol. 2020 Aug;13(2):162-168. doi: 10.3892/mco.2020.2058. Epub 2020 Jun 3. Mol Clin Oncol. 2020. PMID: 32714540 Free PMC article.
References
-
- Liang MK, Yee HT, Song JW, Marks JL. Subdiaphragmatic bronchogenic cysts: a comprehensive review of the literature. Am Surg. 2005;71:1034–41. - PubMed
LinkOut - more resources
Full Text Sources
Other Literature Sources

