Evaluation of Biliary Calprotectin as a Biomarker in Primary Sclerosing Cholangitis
- PMID: 27124059
- PMCID: PMC4998722
- DOI: 10.1097/MD.0000000000003510
Evaluation of Biliary Calprotectin as a Biomarker in Primary Sclerosing Cholangitis
Abstract
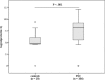
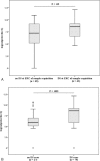
Primary sclerosing cholangitis (PSC) is a chronic inflammatory disease of the bile ducts with limited therapeutic options except liver transplantation. Reliable biomarkers to predict the disease course are unavailable, and currently employed disease activity scores such as the Mayo risk score (MRS) have limitations. The present study aims to evaluate biliary calprotectin as a marker of disease activity and prognosis in PSC.This is a monocentric retrospective observational study. Calprotectin concentrations were measured by an enzyme-linked immunosorbent assay in bile samples collected by endoscopic retrograde cholangiography from 106 PSC patients and 20 controls. Biliary calprotectin concentrations were compared between the 2 groups. In PSC patients, results were evaluated with regard to the presence of dominant bile duct stenoses, bile microbiology, MRS, survival free of liver transplantation, and necessity for bile duct interventions in the further disease course.Median (interquartile ranges) biliary calprotectin concentrations were higher in PSC patients than in controls (3646 ng/mL, 249-9748 vs 116 ng/mL, 104-655; P < 0.001). In the PSC cohort, higher biliary calprotectin concentrations were associated with the presence of microbes in bile (P = 0.02), the occurrence of dominant bile duct stenosis at any time in the disease course (P = 0.005), and the necessity for future bile duct interventions (P = 0.02). Patients with biliary calprotectin concentrations above a cut-off of 11,610 ng/mL displayed significantly shorter transplantation-free survival than those with biliary calprotectin concentrations ≤11,610 ng/mL (P < 0.001). Univariate Cox regression analysis revealed high biliary calprotectin concentration (>11,610 ng/mL) as a risk factor of shorter transplantation-free survival of PSC patients (P < 0.001) beside high plasma alkaline phosphatase (ALP) concentration (>142.5 U/L) (P = 0.006), high MRS (≥2) (P < 0.001), and nonsterility of bile (P = 0.03). Multivariate analysis identified only MRS (P = 0.002) and ALP concentration (P = 0.04) as independent risk factors.Our data strongly suggest that biliary calprotectin may be a valuable additional marker for disease activity and a predictor of outcome in PSC, so that further studies for evaluation of calprotectin in this disease are warranted.
Conflict of interest statement
The authors have no conflicts of interest to disclose.
Figures


References
-
- Gotthardt D, Stiehl A. Endoscopic retrograde cholangiopancreatography in diagnosis and treatment of primary sclerosing cholangitis. Clin Liver Dis 2010; 14:349–358. - PubMed
-
- Eksteen B. Advances and controversies in the pathogenesis and management of primary sclerosing cholangitis. Br Med Bull 2014; 110:89–98. - PubMed
-
- Molodecky NA, Kareemi H, Parab R, et al. Incidence of primary sclerosing cholangitis: a systematic review and meta-analysis. Hepatology 2011; 53:1590–1599. - PubMed
-
- Rudolph G, Gotthardt D, Klöters-Plachky P, et al. Influence of dominant bile duct stenoses and biliary infections on outcome in primary sclerosing cholangitis. J Hepatol 2009; 51:149–155. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources

