The course of lung inflation alters the central pattern of tracheobronchial cough in cat-The evidence for volume feedback during cough
- PMID: 27125979
- PMCID: PMC5369651
- DOI: 10.1016/j.resp.2016.04.008
The course of lung inflation alters the central pattern of tracheobronchial cough in cat-The evidence for volume feedback during cough
Erratum in
-
Corrigendum to "The course of lung inflation alters the central pattern of tracheobronchial cough in cat - The evidence for volume feedback during cough" [Respir. Physiol. Neurobiol. 229 (2016) 43-50].Respir Physiol Neurobiol. 2024 Jan;319:104184. doi: 10.1016/j.resp.2023.104184. Epub 2023 Nov 7. Respir Physiol Neurobiol. 2024. PMID: 37944477 No abstract available.
Abstract
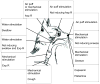
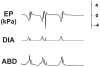
The effect of volume-related feedback and output airflow resistance on the cough motor pattern was studied in 17 pentobarbital anesthetized spontaneously-breathing cats. Lung inflation during tracheobronchial cough was ventilator controlled and triggered by the diaphragm electromyographic (EMG) signal. Altered lung inflations during cough resulted in modified cough motor drive and temporal features of coughing. When tidal volume was delivered (via the ventilator) there was a significant increase in the inspiratory and expiratory cough drive (esophageal pressures and EMG amplitudes), inspiratory phase duration (CTI), total cough cycle duration, and the duration of all cough related EMGs (Tactive). When the cough volume was delivered (via the ventilator) during the first half of inspiratory period (at CTI/2-early over inflation), there was a significant reduction in the inspiratory and expiratory EMG amplitude, peak inspiratory esophageal pressure, CTI, and the overlap between inspiratory and expiratory EMG activity. Additionally, there was significant increase in the interval between the maximum inspiratory and expiratory EMG activity and the active portion of the expiratory phase (CTE1). Control inflations coughs and control coughs with additional expiratory resistance had increased maximum expiratory esophageal pressure and prolonged CTE1, the duration of cough abdominal activity, and Tactive. There was no significant difference in control coughing and/or control coughing when sham ventilation was employed. In conclusion, modified lung inflations during coughing and/or additional expiratory airflow resistance altered the spatio-temporal features of cough motor pattern via the volume related feedback mechanism similar to that in breathing.
Keywords: Airflow resistance; Cough control; Cough motor pattern; Impaired cough; Stretch receptors; Volume feedback.
Copyright © 2016. Published by Elsevier B.V.
Figures


Similar articles
-
Airway mechanics alters generation of cough motor pattern.Respir Physiol Neurobiol. 2024 Oct;328:104315. doi: 10.1016/j.resp.2024.104315. Epub 2024 Aug 14. Respir Physiol Neurobiol. 2024. PMID: 39128767
-
The motor pattern of tracheobronchial cough is affected by inspiratory resistance and expiratory occlusion - The evidence for volume feedback during cough expiration.Respir Physiol Neurobiol. 2019 Mar;261:9-14. doi: 10.1016/j.resp.2018.12.006. Epub 2018 Dec 21. Respir Physiol Neurobiol. 2019. PMID: 30583067
-
Blood pressure changes alter tracheobronchial cough: computational model of the respiratory-cough network and in vivo experiments in anesthetized cats.J Appl Physiol (1985). 2011 Sep;111(3):861-73. doi: 10.1152/japplphysiol.00458.2011. Epub 2011 Jun 30. J Appl Physiol (1985). 2011. PMID: 21719729 Free PMC article.
-
Changes in vagal afferent drive alter tracheobronchial coughing in anesthetized cats.Respir Physiol Neurobiol. 2016 Aug;230:36-43. doi: 10.1016/j.resp.2016.05.008. Epub 2016 May 13. Respir Physiol Neurobiol. 2016. PMID: 27184303
-
Volume feedback during cough in anesthetized cats, effects of occlusions and modulation summary.Respir Physiol Neurobiol. 2021 Jan;283:103547. doi: 10.1016/j.resp.2020.103547. Epub 2020 Sep 14. Respir Physiol Neurobiol. 2021. PMID: 32942050
Cited by
-
OSA and Chronic Respiratory Disease: Mechanisms and Epidemiology.Int J Environ Res Public Health. 2022 Apr 30;19(9):5473. doi: 10.3390/ijerph19095473. Int J Environ Res Public Health. 2022. PMID: 35564882 Free PMC article. Review.
-
Differential effects of acute cerebellectomy on cough in spontaneously breathing cats.PLoS One. 2021 Jun 21;16(6):e0253060. doi: 10.1371/journal.pone.0253060. eCollection 2021. PLoS One. 2021. PMID: 34153070 Free PMC article.
-
Cough modulation by upper airway stimuli in cat - potential clinical application?Open J Mol Integr Physiol. 2016 Aug;6(3):35-43. doi: 10.4236/ojmip.2016.63004. Epub 2016 Aug 22. Open J Mol Integr Physiol. 2016. PMID: 28944100 Free PMC article.
-
GABA-ergic neurotransmission in the nucleus of the solitary tract modulates cough in the cat.Respir Physiol Neurobiol. 2018 Nov;257:100-106. doi: 10.1016/j.resp.2018.02.009. Epub 2018 Feb 21. Respir Physiol Neurobiol. 2018. PMID: 29474953 Free PMC article.
-
Influence of intrathoracic vagotomy on the cough reflex in the anesthetized cat.Respir Physiol Neurobiol. 2022 Feb;296:103805. doi: 10.1016/j.resp.2021.103805. Epub 2021 Oct 19. Respir Physiol Neurobiol. 2022. PMID: 34678475 Free PMC article.
References
-
- Arora NS, Gal TJ. Cough dynamics during progressive expiratory muscle weakness in healthy curarized subjects. J Appl Physiol Respir Environ Exerc Physiol. 1981;51(2):494–498. - PubMed
-
- Bishop B. Vagal control of diaphragm timing in cat while breathing at elevated lung volumes. Respir Physiol. 1977;30(1–2):169–184. - PubMed
-
- Bolser DC, Lindsey BG, Shannon R. Medullary inspiratory activity: influence of intercostal tendon organs and muscle spindle endings. J Appl Physiol (1985) 1987;62(3):1046–1056. - PubMed
-
- Bolser DC, Hey JA, Chapman RW. Influence of central antitussive drugs on the cough motor pattern. J Appl Physiol. 1999;86:1017–1024. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Miscellaneous

