Current trends to measure implant stability
- PMID: 27141160
- PMCID: PMC4837777
- DOI: 10.4103/0972-4052.176539
Current trends to measure implant stability
Abstract
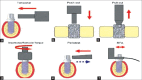
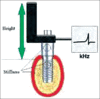
Implant stability plays a critical role for successful osseointegration. Successful osseointegration is a prerequisite for functional dental implants. Continuous monitoring in an objective and qualitative manner is important to determine the status of implant stability. Implant stability is measured at two different stages: Primary and secondary. Primary stability comes from mechanical engagement with cortical bone. Secondary stability is developed from regeneration and remodeling of the bone and tissue around the implant after insertion and affected by the primary stability, bone formation and remodelling. The time of functional loading is dependent upon the implant stability. Historically the gold standard method to evaluate stability were microscopic or histologic analysis, radiographs, however due to invasiveness of these methods and related ethical issues various other methods have been proposed like cutting torque resistance, reverse torque analysis, model analysis etc. It is, therefore, of an utmost importance to be able to access implant stability at various time points and to project a long term prognosis for successful therapy. Therefore this review focuses on the currently available methods for evaluation of implant stability.
Keywords: Primary stability; resonance frequency analysis; secondary stability.
Figures


References
-
- Albrektsson T, Zarb G, Worthington P, Eriksson AR. The long-term efficacy of currently used dental implants: A review and proposed criteria of success. Int J Oral Maxillofac Implants. 1986;1:11–25. - PubMed
-
- Albrektsson T, Talbrektsson B. New York: Raven Press Ltd; 1983. Implant fixation by direct bone anchorage; pp. 87–97.
-
- Meredith N. Assessment of implant stability as a prognostic determinant. Int J Prosthodont. 1998;11:491–501. - PubMed
-
- Brunski JB. Biomechanical factors affecting the bone-dental implant interface. Clin Mater. 1992;10:153–201. - PubMed
-
- Sennerby L, Roos J. Surgical determinants of clinical success of osseointegrated oral implants: A review of the literature. Int J Prosthodont. 1998;11:408–20. - PubMed
Publication types
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
