The Incidence and Differential Seasonal Patterns of Plasmodium vivax Primary Infections and Relapses in a Cohort of Children in Papua New Guinea
- PMID: 27144482
- PMCID: PMC4856325
- DOI: 10.1371/journal.pntd.0004582
The Incidence and Differential Seasonal Patterns of Plasmodium vivax Primary Infections and Relapses in a Cohort of Children in Papua New Guinea
Abstract
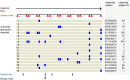
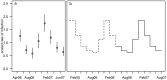
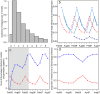
Plasmodium vivax has the ability to relapse from dormant parasites in the liver weeks or months after inoculation, causing further blood-stage infection and potential onward transmission. Estimates of the force of blood-stage infections arising from primary infections and relapses are important for designing intervention strategies. However, in endemic settings their relative contributions are unclear. Infections are frequently asymptomatic, many individuals harbor multiple infections, and while high-resolution genotyping of blood samples enables individual infections to be distinguished, primary infections and relapses cannot be identified. We develop a model and fit it to longitudinal genotyping data from children in Papua New Guinea to estimate the incidence and seasonality of P vivax primary infection and relapse. The children, aged one to three years at enrolment, were followed up over 16 months with routine surveys every two months. Blood samples were taken at the routine visits and at other times if the child was ill. Samples positive by microscopy or a molecular method for species detection were genotyped using high-resolution capillary electrophoresis for P vivax MS16 and msp1F3, and P falciparum msp2. The data were summarized as longitudinal patterns of success or failure to detect a genotype at each routine time-point (eg 001000001). We assume that the seasonality of P vivax primary infection is similar to that of P falciparum since they are transmitted by the same vectors and, because P falciparum does not have the ability to relapse, the seasonality can be estimated. Relapses occurring during the study period can be a consequence of infections occurring prior to the study: we assume that the seasonal pattern of primary infections repeats over time. We incorporate information from parasitological and entomology studies to gain leverage for estimating the parameters, and take imperfect detection into account. We estimate the force of P vivax primary infections to be 11.5 (10.5, 12.3) for a three-year old child per year and the mean number of relapses per infection to be 4.3 (4.0, 4.6) over 16 months. The peak incidence of relapses occurred in the two month interval following the peak interval for primary infections: the contribution to the force of blood-stage infection from relapses is between 71% and 90% depending on the season. Our estimates contribute to knowledge of the P vivax epidemiology and have implications for the timing of intervention strategies targeting different stages of the life cycle.
Conflict of interest statement
The authors have declared that no competing interests exist.
Figures
References
-
- Mendis K, Sina B, Marchesini P, Carter R. The neglected burden of Plasmodium vivax malaria. Am J Trop Med Hyg 2001;64 (1–2 Suppl):97–106. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Molecular Biology Databases

