Contemporary Management Strategies for Chronic Type B Aortic Dissections: A Systematic Review
- PMID: 27144723
- PMCID: PMC4856408
- DOI: 10.1371/journal.pone.0154930
Contemporary Management Strategies for Chronic Type B Aortic Dissections: A Systematic Review
Abstract
Background: Currently, the optimal management strategy for chronic type B aortic dissections (CBAD) is unknown. Therefore, we systematically reviewed the literature to compare results of open surgical repair (OSR), standard thoracic endovascular aortic repair (TEVAR) or branched and fenestrated TEVAR (BEVAR/FEVAR) for CBAD.
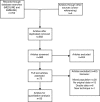
Methods: EMBASE and MEDLINE databases were searched for eligible studies between January 2000 and October 2015. Studies describing outcomes of OSR, TEVAR, B/FEVAR, or all, for CBAD patients initially treated with medical therapy, were included. Primary endpoints were early mortality, and one-year and five-year survival. Secondary endpoints included occurrence of complications. Furthermore, a Time until Treatment Equipoise (TUTE) graph was constructed.
Results: Thirty-five articles were selected for systematic review. A total of 1081 OSR patients, 1397 TEVAR patients and 61 B/FEVAR patients were identified. Early mortality ranged from 5.6% to 21.0% for OSR, 0.0% to 13.7% for TEVAR, and 0.0% to 9.7% for B/FEVAR. For OSR, one-year and five-year survival ranged 72.0%-92.0% and 53.0%-86.7%, respectively. For TEVAR, one-year survival was 82.9%-100.0% and five-year survival 70.0%-88.9%. For B/FEVAR only one-year survival was available, ranging between 76.4% and 100.0%. Most common postoperative complications included stroke (OSR 0.0%-13.3%, TEVAR 0.0%-11.8%), spinal cord ischemia (OSR 0.0%-16.4%, TEVAR 0.0%-12.5%, B/FEVAR 0.0%-12.9%) and acute renal failure (OSR 0.0%-33.3%, TEVAR 0.0%-34.4%, B/FEVAR 0.0%-3.2%). Most common long-term complications after OSR included aneurysm formation (5.8%-20.0%) and new type A dissection (1.7-2.2%). Early complications after TEVAR included retrograde dissection (0.0%-7.1%), malperfusion (1.3%-9.4%), cardiac complications (0.0%-5.9%) and rupture (0.5%-5.0%). Most common long-term complications after TEVAR were rupture (0.5%-7.1%), endoleaks (0.0%-15.8%) and cardiac complications (5.9%-7.1%). No short-term aortic rupture or malperfusion was observed after B/FEVAR. Long-term complications included malperfusion (6.5%) and endoleaks (0.0%-66.7%). Reintervention rates after OSR, TEVAR and B/FEVAR were 5.8%-29.0%, 4.3%-47.4% and 0.0%-53.3%, respectively. TUTE for OSR was 2.7 years, for TEVAR 9.9 months and for B/FEVAR 10.3 months.
Conclusion: We found a limited early survival benefit of standard TEVAR over OSR for CBAD. Complication rates after TEVAR are higher, but complications after OSR are usually more serious. Initial experiences with B/FEVAR show its feasibility, but long-term results are needed to compare it to OSR and standard TEVAR. We conclude that optimal treatment of CBAD remains debatable and merits a patient specific decision. TUTE seems a feasible and useful tool to better understand management outcomes of CBAD.
Conflict of interest statement
Figures
References
-
- Erbel R, Aboyans V, Boileau C, Bossone E, Bartolomeo RD, Eggebrecht H, et al. 2014 ESC Guidelines on the diagnosis and treatment of aortic diseases: Document covering acute and chronic aortic diseases of the thoracic and abdominal aorta of the adult. The Task Force for the Diagnosis and Treatment of Aortic Diseases of the European Society of Cardiology (ESC). Eur Heart J. 2014;35(41):2873–926. 10.1093/eurheartj/ehu281 - DOI - PubMed
-
- Sobocinski J, Spear R, Tyrrell MR, Maurel B, Martin Gonzalez T, Hertault A, et al. Chronic dissection—indications for treatment with branched and fenestrated stent-grafts. J Cardiovasc Surg (Torino). 2014;55(4):505–17. - PubMed
-
- Akutsu K, Nejima J, Kiuchi K, Sasaki K, Ochi M, Tanaka K, et al. Effects of the patent false lumen on the long-term outcome of type B acute aortic dissection. Eur J Cardiothorac Surg. 2004;26(2):359–66. - PubMed
-
- Gysi J, Schaffner T, Mohacsi P, Aeschbacher B, Althaus U, Carrel T. Early and late outcome of operated and non-operated acute dissection of the descending aorta. Eur J Cardiothorac Surg. 1997;11(6):1163–9; discussion 9–70. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources