Cardiometabolic Effects of Chronic Hyperandrogenemia in a New Model of Postmenopausal Polycystic Ovary Syndrome
- PMID: 27145003
- PMCID: PMC4929551
- DOI: 10.1210/en.2015-1617
Cardiometabolic Effects of Chronic Hyperandrogenemia in a New Model of Postmenopausal Polycystic Ovary Syndrome
Abstract
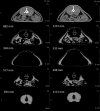
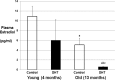
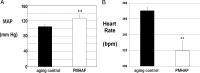
Postmenopausal women who have had polycystic ovary syndrome (PCOS) and chronic hyperandrogenemia may be at a greater risk for cardiovascular disease than normoandrogenemic postmenopausal women. The cardiometabolic effect of chronic hyperandrogenemia in women with PCOS after menopause is unclear. The present study was performed to test the hypothesis that chronic hyperandrogenemia in aging female rats would have more deleterious effects on metabolic function, blood pressure, and renal function than in normoandrogenemic age-matched females. Female Sprague Dawley were implanted continuously, beginning at 4-5 weeks, with dihydrotestosterone (postmenopausal hyperandrogenemic female [PMHAF]) or placebo pellets (controls), and were studied at 13 months of age. Plasma DHT was 3-fold higher, and estradiol was 90% lower in PMHAF than controls. Body weights were higher; EchoMRI showed greater fat and lean mass; and computed tomography showed more sc and visceral adiposity in PMHAF, but with similar femur length compared with controls. Insulin resistance was present in PMHAF with higher plasma insulin, normal fasting blood glucose, abnormal oral glucose tolerance test, and higher nonfasting blood glucose. Blood pressure (radiotelemetry) was significantly higher and heart rate was lower, and renal function (glomerular filtration rate) was reduced by 40% in PMHAF. Thus the aging chronically hyperandrogenemic female rat is a new model of postmenopausal PCOS, which exhibits insulin resistance and visceral obesity, hypertension, and impairment in renal function. This new model provides a unique tool to study the deleterious effects of chronic androgen excess in postmenopausal females rats.
Figures

Similar articles
-
Cardiovascular-renal and metabolic characterization of a rat model of polycystic ovary syndrome.Gend Med. 2011 Apr;8(2):103-15. doi: 10.1016/j.genm.2010.11.013. Gend Med. 2011. PMID: 21536229 Free PMC article.
-
Consequences of advanced aging on renal function in chronic hyperandrogenemic female rat model: implications for aging women with polycystic ovary syndrome.Physiol Rep. 2017 Nov;5(20):e13461. doi: 10.14814/phy2.13461. Physiol Rep. 2017. PMID: 29051304 Free PMC article.
-
Effect of GLP-1 Receptor Agonists in the Cardiometabolic Complications in a Rat Model of Postmenopausal PCOS.Endocrinology. 2019 Dec 1;160(12):2787-2799. doi: 10.1210/en.2019-00450. Endocrinology. 2019. PMID: 31593246 Free PMC article.
-
The impact of hyperandrogenism in female obesity and cardiometabolic diseases associated with polycystic ovary syndrome.Horm Mol Biol Clin Investig. 2013 Sep;15(3):91-103. doi: 10.1515/hmbci-2013-0014. Horm Mol Biol Clin Investig. 2013. PMID: 25436736 Review.
-
Cardiovascular risk in postmenopausal women with the polycystic ovary syndrome.Maturitas. 2011 Jan;68(1):13-6. doi: 10.1016/j.maturitas.2010.09.005. Epub 2010 Oct 12. Maturitas. 2011. PMID: 20943333 Review.
Cited by
-
Pregnancy Protects Hyperandrogenemic Female Rats From Postmenopausal Hypertension.Hypertension. 2020 Sep;76(3):943-952. doi: 10.1161/HYPERTENSIONAHA.120.15504. Epub 2020 Aug 3. Hypertension. 2020. PMID: 32755410 Free PMC article.
-
Association of Oxidative Stress with Kidney Injury in a Hyperandrogenemic Female Rat Model.Iran J Med Sci. 2023 Mar;48(2):187-197. doi: 10.30476/IJMS.2022.93594.2497. Iran J Med Sci. 2023. PMID: 36895462 Free PMC article.
-
Cardiometabolic consequences of maternal hyperandrogenemia in male offspring.Physiol Rep. 2021 Jul;9(14):e14941. doi: 10.14814/phy2.14941. Physiol Rep. 2021. PMID: 34288567 Free PMC article.
-
Cardiovascular disease risk in offspring of polycystic ovary syndrome.Front Endocrinol (Lausanne). 2022 Nov 30;13:977819. doi: 10.3389/fendo.2022.977819. eCollection 2022. Front Endocrinol (Lausanne). 2022. PMID: 36531474 Free PMC article. Review.
-
Consequences of hyperandrogenemia during pregnancy in female offspring: attenuated response to angiotensin II.J Hypertens. 2022 Apr 1;40(4):712-722. doi: 10.1097/HJH.0000000000003067. J Hypertens. 2022. PMID: 34980865 Free PMC article.
References
-
- Azziz R, Carmina E, Dewailly D, et al. Position statement: Criteria for defining polycystic ovary syndrome: An Androgen Excess Society guideline. J Clin Endocrinol Metab. 2006;91:4237–4235. - PubMed
-
- Escobar-Morreale HF, San Millan JL. Abdominal adiposity and the polycystic ovary syndrome. Trends in Endocrinol Metab. 2007;18:266–272. - PubMed
-
- Diamanti-Kandarakis E. Polycystic ovarian syndrome: Pathophysiology, molecular aspects and clinical implications. Exp Rev Molec Med. 2008;10:1–21. - PubMed
-
- Luque-Ramírez M, Martí D, Fernández-Durán E, Alpañés M, Álvarez-Blasco F, Escobar-Morreale HF. Office blood pressure, ambulatory blood pressure monitoring, and echocardiographic abnormalities in women with polycystic ovary syndrome: Role of obesity and androgen excess. Hypertension. 2014;63:624–629. - PubMed
-
- Zuchurzok-Buczynska A, Szydlowski L, Gawlik A, Wilk K, Malecka-Tendera E. Blood pressure regulation and resting heart rate abnormalities in adolescent girls with polycystiv ovary syndrome. Fertil Steril. 2011;96:1519–1525. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

