Pathology of eyelid tumors
- PMID: 27146927
- PMCID: PMC4869455
- DOI: 10.4103/0301-4738.181752
Pathology of eyelid tumors
Abstract
The eyelids are composed of four layers: skin and subcutaneous tissue including its adnexa, striated muscle, tarsus with the meibomian glands, and the palpebral conjunctiva. Benign and malignant tumors can arise from each of the eyelid layers. Most eyelid tumors are of cutaneous origin, mostly epidermal, which can be divided into epithelial and melanocytic tumors. Benign epithelial lesions, cystic lesions, and benign melanocytic lesions are very common. The most common malignant eyelid tumors are basal cell carcinoma in Caucasians and sebaceous gland carcinoma in Asians. Adnexal and stromal tumors are less frequent. The present review describes the more important eyelid tumors according to the following groups: Benign and malignant epithelial tumors, benign and malignant melanocytic tumors, benign and malignant adnexal tumors, stromal eyelid tumors, lymphoproliferative and metastatic tumors, other rare eyelid tumors, and inflammatory and infections lesions that simulate neoplasms.
Figures
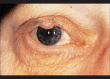





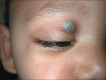


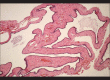
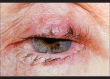


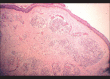

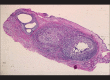
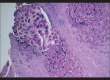
Similar articles
-
A retrospective study of 2228 cases with eyelid tumors.Int J Ophthalmol. 2018 Nov 18;11(11):1835-1841. doi: 10.18240/ijo.2018.11.16. eCollection 2018. Int J Ophthalmol. 2018. PMID: 30450316 Free PMC article.
-
[Modified meibography in malignant eyelid tumors of epithelial origin].Vestn Oftalmol. 2019;135(5. Vyp. 2):141-149. doi: 10.17116/oftalma2019135052141. Vestn Oftalmol. 2019. PMID: 31691652 Russian.
-
[Tumors and tumor-like lesions of eyelids collected at Department of Pathological Anatomy, Wroclaw Medical University, between 1946 and 1999].Klin Oczna. 2005;107(7-9):475-8. Klin Oczna. 2005. PMID: 16417001 Polish.
-
[Incidence of benign and malignant lesions of eyelid and conjunctival tumors].Nippon Ganka Gakkai Zasshi. 2005 Sep;109(9):573-9. Nippon Ganka Gakkai Zasshi. 2005. PMID: 16218435 Review. Japanese.
-
[Diagnosis and treatment of benign eyelid tumors].Ophthalmologie. 2023 Mar;120(3):240-251. doi: 10.1007/s00347-022-01798-x. Epub 2023 Feb 10. Ophthalmologie. 2023. PMID: 36763162 Review. German.
Cited by
-
Characteristics and Factors Related to Eyelid Basal Cell Carcinoma in Saudi Arabia.Middle East Afr J Ophthalmol. 2018 Apr-Jun;25(2):96-102. doi: 10.4103/meajo.MEAJO_305_17. Middle East Afr J Ophthalmol. 2018. PMID: 30122855 Free PMC article.
-
Lower Eyelid Nodule: Chalazion or Idiopathic Facial Aseptic Granuloma? A Case Series.Acta Derm Venereol. 2021 May 10;101(5):adv00451. doi: 10.2340/00015555-3779. Acta Derm Venereol. 2021. PMID: 33686444 Free PMC article. No abstract available.
-
Analysis of Tumour Related Data and Clinical Features of Eyelid Carcinomas.Curr Health Sci J. 2020 Jul-Sep;46(3):222-229. doi: 10.12865/CHSJ.46.03.02. Epub 2020 Sep 30. Curr Health Sci J. 2020. PMID: 33304622 Free PMC article.
-
Population-Based Incidence and Clinical Characteristics of Ocular Adnexal Tumors in Olmsted County, Minnesota.Ophthalmic Epidemiol. 2025 Jun;32(3):326-333. doi: 10.1080/09286586.2024.2379971. Epub 2024 Aug 30. Ophthalmic Epidemiol. 2025. PMID: 39212488
-
Clinicopathological analysis of eyelid lesions in Sri Lanka.Int Ophthalmol. 2023 Jul;43(7):2513-2519. doi: 10.1007/s10792-023-02651-z. Epub 2023 Mar 7. Int Ophthalmol. 2023. PMID: 36881193
References
-
- Bedrossian EH. Embryology and anatomy of the eyelid. In: Tasman W, Jaeger EA, editors. Duane's Foundation of Clinical Ophthalmology, Ocular Anatomy, Embryology and Teratology. Vol. 1. Philadelphia: Lippincott Williams & Wilkins; 2004. pp. 1–24. Ch. 5.
-
- Campbell RJ, Sobin LH. World Health Organization International Histological Classification of Tumors. 2nd ed. Berlin: Springer; 1998. Tumours of the eyelid; pp. 3–9.
-
- Pe'er J. Eyelid tumors: Classification and differential diagnosis. In: Pe'er J, Singh AD, editors. Clinical Ophthalmic Oncology: Eyelid and Conjunctival Tumors. 2nd ed. Berlin: Springer; 2014. pp. 9–10. Ch. 2.
-
- Kersten RC, Ewing-Chow D, Kulwin DR, Gallon M. Accuracy of clinical diagnosis of cutaneous eyelid lesions. Ophthalmology. 1997;104:479–84. - PubMed
-
- Font RL. Ophthalmic Pathology. An Atlas and Textbook. 3rd ed. Philadelphia: WB Saunders; 1996. Eyelids and lacrimal drainage system; pp. 2229–32.
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources

