Employment Outcomes After Critical Illness: An Analysis of the Bringing to Light the Risk Factors and Incidence of Neuropsychological Dysfunction in ICU Survivors Cohort
- PMID: 27171492
- PMCID: PMC5069078
- DOI: 10.1097/CCM.0000000000001849
Employment Outcomes After Critical Illness: An Analysis of the Bringing to Light the Risk Factors and Incidence of Neuropsychological Dysfunction in ICU Survivors Cohort
Abstract
Objectives: To characterize survivors' employment status after critical illness and to determine if duration of delirium during hospitalization and residual cognitive function are each independently associated with decreased employment.
Design: Prospective cohort investigation with baseline and in-hospital clinical data and follow-up at 3 and 12 months.
Setting: Medical and surgical ICUs at two tertiary-care hospitals.
Patients: Previously employed patients from the Bringing to Light the Risk Factors and Incidence of Neuropsychological Dysfunction in ICU Survivors study who survived a critical illness due to respiratory failure or shock were evaluated for global cognition and employment status at 3- and 12-month follow-up.
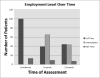
Measurements and main results: We used multivariable logistic regression to evaluate independent associations between employment at both 3 and 12 months and global cognitive function at the same time point, and delirium during the hospital stay. At 3-month follow-up, 113 of the total survival cohort of 448 (25%) were identified as being employed at study enrollment. Of these, 94 survived to 12-month follow-up. At 3- and 12-month follow-up, 62% and 49% had a decrease in employment, 57% and 49% of whom, respectively, were newly unemployed. After adjustment for physical health status, depressive symptoms, marital status, level of education, and severity of illness, we did not find significant predictors of employment status at 3 months, but better cognition at 12 months was marginally associated with lower odds of employment reduction at 12 months (odds ratio, 0.49; p = 0.07).
Conclusions: Reduction in employment after critical illness was present in the majority of our ICU survivors, approximately half of which was new unemployment. Cognitive function at 12 months was a predictor of subsequent employment status. Further research is needed into the potential relationship between the impact of critical illness on cognitive function and employment status.
Figures

Comment in
-
The Road to Recovery: Turning the Tide on Losses Incurred After Critical Illness.Crit Care Med. 2016 Nov;44(11):2111-2112. doi: 10.1097/CCM.0000000000001925. Crit Care Med. 2016. PMID: 27755073 No abstract available.
Similar articles
-
Clinical phenotypes of delirium during critical illness and severity of subsequent long-term cognitive impairment: a prospective cohort study.Lancet Respir Med. 2018 Mar;6(3):213-222. doi: 10.1016/S2213-2600(18)30062-6. Lancet Respir Med. 2018. PMID: 29508705 Free PMC article.
-
Association of Hypoactive and Hyperactive Delirium With Cognitive Function After Critical Illness.Crit Care Med. 2020 Jun;48(6):e480-e488. doi: 10.1097/CCM.0000000000004313. Crit Care Med. 2020. PMID: 32317589 Free PMC article.
-
Depression, post-traumatic stress disorder, and functional disability in survivors of critical illness in the BRAIN-ICU study: a longitudinal cohort study.Lancet Respir Med. 2014 May;2(5):369-79. doi: 10.1016/S2213-2600(14)70051-7. Epub 2014 Apr 7. Lancet Respir Med. 2014. PMID: 24815803 Free PMC article.
-
Return to Employment after Critical Illness and Its Association with Psychosocial Outcomes. A Systematic Review and Meta-Analysis.Ann Am Thorac Soc. 2019 Oct;16(10):1304-1311. doi: 10.1513/AnnalsATS.201903-248OC. Ann Am Thorac Soc. 2019. PMID: 31184500
-
Factors associated with employment outcome after critical illness: Systematic review, meta-analysis, and meta-regression.J Adv Nurs. 2021 Feb;77(2):653-663. doi: 10.1111/jan.14631. Epub 2020 Nov 19. J Adv Nurs. 2021. PMID: 33210753
Cited by
-
Advance Identification of Patients With Chronic Conditions and Acute Respiratory Failure at Greatest Risk for High-Intensity, Costly Care.J Pain Symptom Manage. 2022 Apr;63(4):618-626. doi: 10.1016/j.jpainsymman.2021.11.004. Epub 2021 Nov 15. J Pain Symptom Manage. 2022. PMID: 34793946 Free PMC article.
-
Post-intensive care syndrome after a critical COVID-19: cohort study from a Belgian follow-up clinic.Ann Intensive Care. 2021 Jul 29;11(1):118. doi: 10.1186/s13613-021-00910-9. Ann Intensive Care. 2021. PMID: 34324073 Free PMC article.
-
Financial Toxicity After Acute Respiratory Distress Syndrome: A National Qualitative Cohort Study.Crit Care Med. 2020 Aug;48(8):1103-1110. doi: 10.1097/CCM.0000000000004378. Crit Care Med. 2020. PMID: 32697479 Free PMC article.
-
Improving Quality of Life in Patients at Risk for Post-Intensive Care Syndrome.Mayo Clin Proc Innov Qual Outcomes. 2018 Nov 26;2(4):359-369. doi: 10.1016/j.mayocpiqo.2018.10.001. eCollection 2018 Dec. Mayo Clin Proc Innov Qual Outcomes. 2018. PMID: 30560238 Free PMC article.
-
Patients suffering from psychological impairments following critical illness are in need of information.J Intensive Care. 2020 Jan 9;8:6. doi: 10.1186/s40560-019-0422-0. eCollection 2020. J Intensive Care. 2020. PMID: 31938546 Free PMC article.
References
-
- Halpern NA, Pastores SM, Greenstein RJ. Critical care medicine in the United States 1985-2000: an analysis of bed numbers, use, and costs. Critical care medicine. 2004;32:1254–1259. - PubMed
-
- Halpern NA, Pastores SM. Critical care medicine in the United States 2000-2005: an analysis of bed numbers, occupancy rates, payer mix, and costs. Crit Care Med. 2010;38:65–71. - PubMed
-
- Castellanos-Ortega A, Suberviola B, Garcia-Astudillo LA, Holanda MS, Ortiz F, Llorca J, Delgado-Rodriguez M. Impact of the Surviving Sepsis Campaign protocols on hospital length of stay and mortality in septic shock patients: results of a three-year follow-up quasi-experimental study. Crit Care Med. 2010;38:1036–1043. - PubMed
-
- Iwashyna TJ. Survivorship will be the defining challenge of critical care in the 21st century. Ann Intern Med. 2010;153:204–205. - PubMed
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

