European perspective in Thoracic surgery-eso-coloplasty: when and how?
- PMID: 27195136
- PMCID: PMC4856848
- DOI: 10.21037/jtd.2016.04.43
European perspective in Thoracic surgery-eso-coloplasty: when and how?
Abstract
Colon interposition has been used since the beginning of the 20(th) century as a substitute for esophageal replacement. Colon interposition is mainly chosen as a second line treatment when the stomach cannot be used, when the stomach has to be resected for oncological or technical reasons, or when the stomach is deliberately kept intact for benign diseases in young patients with long-life expectancy. During the surgery the vascularization of the colon must be carefully assessed, as well as the type of the graft (right or left colon), the length of the graft, the surgical approach and the route of the reconstruction. Early complications such as graft necrosis or anastomotic leaks, and late complications such as redundancy depend on the quality of the initial surgery. Despite a complex and time-consuming procedure requiring at least three or four digestive anastomoses, reported long term functional outcomes of colon interposition are good, with an acceptable operative risk. Thus, in very selected indications, colon interposition could be seen as a valuable alternative for esophageal replacement when stomach cannot be considered. This review aims at briefly defining "when" and "how" to perform a coloplasty through demonstrative videos.
Keywords: Esophageal surgery; benign esophageal disease; colon interposition; esophageal cancer; esophageal motility dysfunction.
Conflict of interest statement
Figures
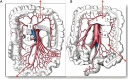










References
-
- Kelling GE. Oesophagoplastik mit Hilfe des Querkolons. Zentralbl Chir 1911;38:1209-12.
-
- Von Hacker V. Uber Oesophagoplastik in Allgemeinen under uber den Ersatz der Speiserohre durch antethorakle Hautdickdarmschlauchbildung im Besonderen. Arch Klin Chir 1914;105:973.
Publication types
LinkOut - more resources
Full Text Sources
Other Literature Sources
