Depressive Symptoms, Patient Satisfaction, and Quality of Life Over Time in Automated and Continuous Ambulatory Peritoneal Dialysis Patients: A Prospective Multicenter Propensity-Matched Study
- PMID: 27227956
- PMCID: PMC4902380
- DOI: 10.1097/MD.0000000000003795
Depressive Symptoms, Patient Satisfaction, and Quality of Life Over Time in Automated and Continuous Ambulatory Peritoneal Dialysis Patients: A Prospective Multicenter Propensity-Matched Study
Abstract
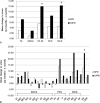
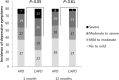
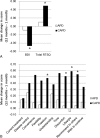
Health-related quality of life (HRQOL) is an important clinical outcome for dialysis patients. However, relative superiority in HRQOL between automated peritoneal dialysis (APD) and continuous ambulatory peritoneal dialysis (CAPD) are not clearly known. We compared HRQOL over time between APD and CAPD patients and evaluated factors associated with HRQOL.All 260 incident patients initiating APD or CAPD at multiple centers throughout Korea were prospectively enrolled in this study between October 2010 and February 2013. HRQOL, depressive symptoms, and renal treatment satisfaction were assessed 1 and 12 months after the start of dialysis by the Kidney Disease Quality of Life Short Form 36 (KDQOL-36), the Beck Depression Inventory (BDI), and the Renal Treatment Satisfaction Questionnaire (RTSQ), respectively.Of 196 patients who completed all questionnaires and did not change the peritoneal dialysis (PD) modality during the 1-year follow-up period, 160 were matched. APD patients showed better baseline HRQOL than CAPD patients for the symptoms, patient satisfaction, pain, and social function domains. There were no differences in HRQOL between the 2 groups at 12 months, and CAPD patients had significantly greater improvements in symptoms (P = 0.02), the mental composite summary (P = 0.03), and health status domains (P = 0.03) than APD patients. There were similar improvements in depressive symptoms (P = 0.01) and patient satisfaction with treatment (P = 0.01) in CAPD and APD patients. Interestingly, depressive symptoms, not PD modality, was the most influential and consistent factor for HRQOL. Despite the spontaneous improvement of depressive symptoms, considerable PD patients still had depressive symptoms at the 1-year appointment.APD has no advantage over CAPD for HRQOL. Considering the substantial negative effect of depressive symptoms on HRQOL, it is important to evaluate PD patients for depression and to treat those with depression to improve their HRQOL.
Conflict of interest statement
The authors have no conflicts of interest to disclose.
Figures
Similar articles
-
Comparison of effects of automated peritoneal dialysis and continuous ambulatory peritoneal dialysis on health-related quality of life, sleep quality, and depression.Hemodial Int. 2010 Oct;14(4):515-22. doi: 10.1111/j.1542-4758.2010.00465.x. Hemodial Int. 2010. PMID: 20955286
-
Comparison of cost-utility between automated peritoneal dialysis and continuous ambulatory peritoneal dialysis.Arch Med Res. 2013 Nov;44(8):655-61. doi: 10.1016/j.arcmed.2013.10.017. Epub 2013 Nov 8. Arch Med Res. 2013. PMID: 24211750
-
A comparison of health-related quality of life between continuous ambulatory peritoneal dialysis and automated peritoneal dialysis in children with stage 5 chronic kidney disease in Thailand: a randomized controlled trial.Pediatr Nephrol. 2025 Jun;40(6):2029-2041. doi: 10.1007/s00467-024-06632-x. Epub 2025 Jan 20. Pediatr Nephrol. 2025. PMID: 39833615 Free PMC article. Clinical Trial.
-
Long-term outcomes in automated peritoneal dialysis: similar or better than in continuous ambulatory peritoneal dialysis?Perit Dial Int. 2009 Feb;29 Suppl 2:S111-4. Perit Dial Int. 2009. PMID: 19270197 Review.
-
[Adequate peritoneal dialysis: limitations of continuous ambulatory peritoneal dialysis (CAPD), place of automated peritoneal dialysis (APD)].Nephrologie. 1998;19(5):239-44. Nephrologie. 1998. PMID: 9793936 Review. French.
Cited by
-
Automated Peritoneal Dialysis: Patient Perspectives and Outcomes.Int J Nephrol Renovasc Dis. 2021 Oct 7;14:385-392. doi: 10.2147/IJNRD.S236553. eCollection 2021. Int J Nephrol Renovasc Dis. 2021. PMID: 34675604 Free PMC article. Review.
-
Better Quality of Life of Peritoneal Dialysis compared to Hemodialysis over a Two-year Period after Dialysis Initiation.Sci Rep. 2019 Jul 16;9(1):10266. doi: 10.1038/s41598-019-46744-1. Sci Rep. 2019. PMID: 31312004 Free PMC article.
-
Symptom profiles in patients receiving maintenance hemodialysis and their association with quality of life: a longitudinal study.Qual Life Res. 2024 Jun;33(6):1501-1512. doi: 10.1007/s11136-024-03630-2. Epub 2024 Apr 2. Qual Life Res. 2024. PMID: 38565748
-
Patient-reported advantages and disadvantages of peritoneal dialysis: results from the PDOPPS.BMC Nephrol. 2019 Apr 2;20(1):116. doi: 10.1186/s12882-019-1304-3. BMC Nephrol. 2019. PMID: 30940103 Free PMC article.
-
Health-Related Quality of Life in Patients Treated with Continuous Ambulatory Peritoneal Dialysis and Automated Peritoneal Dialysis in Singapore.Pharmacoecon Open. 2018 Jun;2(2):203-208. doi: 10.1007/s41669-017-0046-z. Pharmacoecon Open. 2018. PMID: 29623617 Free PMC article.
References
-
- de Wit GA, Merkus MP, Krediet RT, et al. A comparison of quality of life of patients on automated and continuous ambulatory peritoneal dialysis. Perit Dial Int 2001; 21:306–312. - PubMed
-
- Cukor D, Peterson RA, Cohen SD, et al. Depression in end-stage renal disease hemodialysis patients. Nat Clin Pract Nephrol 2006; 2:678–687. - PubMed
-
- Mapes DL, Lopes AA, Satayathum S, et al. Health-related quality of life as a predictor of mortality and hospitalization: The Dialysis Outcomes and Practice Patterns Study (DOPPS). Kidney Int 2003; 64:339–349. - PubMed
-
- Farrokhi F, Abedi N, Beyene J, et al. Association between depression and mortality in patients receiving long-term dialysis: a systematic review and meta-analysis. Am J Kidney Dis 2014; 63:623–635. - PubMed
-
- Valderrabano F, Jofre R, Lopez-Gomez JM. Quality of life in end-stage renal disease patients. Am J Kidney Dis 2001; 38:443–464. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

