Modeling the efficacy of the extent of surgical resection in the setting of radiation therapy for glioblastoma
- PMID: 27240229
- PMCID: PMC4982585
- DOI: 10.1111/cas.12979
Modeling the efficacy of the extent of surgical resection in the setting of radiation therapy for glioblastoma
Abstract
Standard therapy for glioblastoma (GBM) includes maximal surgical resection and radiation therapy. While it is established that radiation therapy provides the greatest survival benefit of standard treatment modalities, the impact of the extent of surgical resection (EOR) on patient outcome remains highly controversial. While some studies describe no correlation between EOR and patient survival even up to total resection, others propose either qualitative (partial versus subtotal versus complete resection) or quantitative EOR thresholds, below which there is no correlation with survival. This work uses a mathematical model in the form of a reaction-diffusion partial differential equation to simulate tumor growth and treatment with radiation therapy and surgical resection based on tumor-specific rates of diffusion and proliferation. Simulation of 36 tumors across a wide spectrum of diffusion and proliferation rates suggests that while partial or subtotal resections generally do not provide a survival advantage, complete resection significantly improves patient outcomes. Furthermore, our model predicts a tumor-specific quantitative threshold below which EOR has no effect on patient survival and demonstrates that this threshold increases with tumor aggressiveness, particularly with the rate of proliferation. Thus, this model may serve as an aid for determining both when surgical resection is indicated as well as the surgical margins necessary to provide clinically significant improvements in patient survival. In addition, by assigning relative benefits to radiation and surgical resection based on tumor invasiveness and proliferation, this model confirms that (with the exception of the least aggressive tumors) the survival benefit of radiation therapy exceeds that of surgical resection.
Keywords: Extent of resection; glioblastoma; mathematical modeling; radiation therapy; surgical therapy.
© 2016 The Authors. Cancer Science published by John Wiley & Sons Australia, Ltd on behalf of Japanese Cancer Association.
Figures


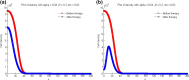


Similar articles
-
An extent of resection threshold for newly diagnosed glioblastomas.J Neurosurg. 2011 Jul;115(1):3-8. doi: 10.3171/2011.2.jns10998. Epub 2011 Mar 18. J Neurosurg. 2011. PMID: 21417701
-
Residual tumor volume versus extent of resection: predictors of survival after surgery for glioblastoma.J Neurosurg. 2014 Nov;121(5):1115-23. doi: 10.3171/2014.7.JNS132449. Epub 2014 Sep 5. J Neurosurg. 2014. PMID: 25192475
-
An extent of resection threshold for recurrent glioblastoma and its risk for neurological morbidity.J Neurosurg. 2014 Apr;120(4):846-53. doi: 10.3171/2013.12.JNS13184. Epub 2014 Jan 31. J Neurosurg. 2014. PMID: 24484232
-
Survival Benefit of Maximal Resection for Glioblastoma Reoperation in the Temozolomide Era: A Meta-Analysis.World Neurosurg. 2019 Jul;127:31-37. doi: 10.1016/j.wneu.2019.03.250. Epub 2019 Apr 1. World Neurosurg. 2019. PMID: 30947000 Review.
-
Role of Intra-operative MRI (iMRI) in Improving Extent of Resection and Survival in Patients with Glioblastoma Multiforme.J Pak Med Assoc. 2017 Jul;67(7):1121-1123. J Pak Med Assoc. 2017. PMID: 28770902 Review.
Cited by
-
Timing of glioblastoma surgery and patient outcomes: a multicenter cohort study.Neurooncol Adv. 2021 Apr 8;3(1):vdab053. doi: 10.1093/noajnl/vdab053. eCollection 2021 Jan-Dec. Neurooncol Adv. 2021. PMID: 34056605 Free PMC article.
-
A Review of Mathematical Models for Tumor Dynamics and Treatment Resistance Evolution of Solid Tumors.CPT Pharmacometrics Syst Pharmacol. 2019 Oct;8(10):720-737. doi: 10.1002/psp4.12450. Epub 2019 Aug 9. CPT Pharmacometrics Syst Pharmacol. 2019. PMID: 31250989 Free PMC article. Review.
-
Estimating intratumoral heterogeneity from spatiotemporal data.J Math Biol. 2018 Dec;77(6-7):1999-2022. doi: 10.1007/s00285-018-1238-6. Epub 2018 May 8. J Math Biol. 2018. PMID: 29737395
-
Salinomycin-Loaded Iron Oxide Nanoparticles for Glioblastoma Therapy.Nanomaterials (Basel). 2020 Mar 6;10(3):477. doi: 10.3390/nano10030477. Nanomaterials (Basel). 2020. PMID: 32155938 Free PMC article.
-
Intraoperative rapid molecular diagnosis aids glioma subtyping and guides precise surgical resection.Ann Clin Transl Neurol. 2024 Aug;11(8):2176-2187. doi: 10.1002/acn3.52138. Epub 2024 Jun 24. Ann Clin Transl Neurol. 2024. PMID: 38924338 Free PMC article.
References
-
- Nishikawa R. Standard therapy for glioblastoma – A review of where we are. Neurol Med Chir (Tokyo) 2010; 50: 713–9. - PubMed
-
- Hentschel SJ, Sawaya R. Optimizing outcomes with maximal surgical resection of malignant gliomas. Cancer Control 2003; 10: 109–14. - PubMed
-
- Quigley MR, Maroon JC. The relationship between survival and the extent of the resection in patients with supratentorial malignant gliomas. Neurosurgery 1991; 29: 385–9. - PubMed
-
- Nazzaro JM, Neuwelt EA. The role of surgery in the management of supratentorial intermediate and high‐grade astrocytomas in adults. J Neurosurg 1990; 73: 331–44. - PubMed
-
- Hess KR. Extent of resection as a prognostic variable in the treatment of gliomas. J Neurooncol 1999; 42: 227–31. - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources

