Multidisciplinary Approach to the Treatment of Concomitant Rectal and Vaginal Prolapse
- PMID: 27247534
- PMCID: PMC4882172
- DOI: 10.1055/s-0036-1580721
Multidisciplinary Approach to the Treatment of Concomitant Rectal and Vaginal Prolapse
Abstract
Rectal prolapse and vaginal prolapse have traditionally been treated as separate entities despite sharing a common pathophysiology. This compartmentalized approach often leads to frustration and suboptimal outcomes. In recent years, there has been a shift to a more patient-centered, multidisciplinary approach. Procedures to repair pelvic organ prolapse are divided into three categories: abdominal, perineal, and a combination of both. Most commonly, a combined minimally invasive abdominal sacral colpopexy and ventral rectopexy is performed to treat concomitant rectal and vaginal prolapse. Combining the two procedures adds little operative time and offers complete pelvic floor repair. The choice of minimally invasive abdominal prolapse repair versus perineal repair depends on the patient's comorbidities, previous surgeries, preference to avoid mesh, and physician's expertise. Surgeons should at least be able to identify these patients and provide the appropriate treatment or refer them to specialized centers.
Keywords: pelvic organ prolapse; rectopexy; sacral colpopexy.
Figures
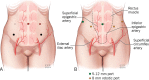
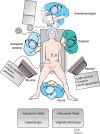

References
-
- Lim M, Sagar P M, Gonsalves S, Thekkinkattil D, Landon C. Surgical management of pelvic organ prolapse in females: functional outcome of mesh sacrocolpopexy and rectopexy as a combined procedure. Dis Colon Rectum. 2007;50(9):1412–1421. - PubMed
-
- González-Argenté F X, Jain A, Nogueras J J, Davila G W, Weiss E G, Wexner S D. Prevalence and severity of urinary incontinence and pelvic genital prolapse in females with anal incontinence or rectal prolapse. Dis Colon Rectum. 2001;44(7):920–926. - PubMed
-
- Collopy B T Barham K A Abdominal colporectopexy with pelvic cul-de-sac closure Dis Colon Rectum 2002454522–526., discussion 526–529 - PubMed
-
- Baessler K, Schuessler B. Abdominal sacrocolpopexy and anatomy and function of the posterior compartment. Obstet Gynecol. 2001;97(5, Pt 1):678–684. - PubMed
Publication types
LinkOut - more resources
Full Text Sources
Other Literature Sources

