Treatment Interval between Neoadjuvant Chemoradiotherapy and Surgery in Rectal Cancer Patients: A Population-Based Study
- PMID: 27251135
- PMCID: PMC5009153
- DOI: 10.1245/s10434-016-5294-0
Treatment Interval between Neoadjuvant Chemoradiotherapy and Surgery in Rectal Cancer Patients: A Population-Based Study
Abstract
Background: Neoadjuvant chemoradiation therapy (CRT) has been widely implemented in the treatment of rectal cancer patients, but optimal timing of surgery after neoadjuvant therapy is unclear. The purpose of this study was to evaluate the effects of prolonged intervals between long-course CRT and surgery in rectal cancer patients.
Methods: Data on all rectal cancer patients diagnosed between 2006 and 2011 were retrieved from the population-based Netherlands Cancer Registry; the main outcome parameters were pathologic complete response (pCR) and overall survival (OS). Outcomes were reported separately for patients with early tumors (ETs; N = 217) and locally advanced rectal cancer (LARC; N = 1073). Patients were divided into 2-week interval groups according to treatment interval, ranging from 5-6 to 13-14 weeks. Kaplan-Meier curves, and logistic regression and Cox regression models were used for data analysis.
Results: No significant difference in pCR rate was observed for ET patients according to treatment interval. Compared with a treatment interval of 7-8 weeks, pCR rates in LARC patients were higher after 9-10 weeks (18.4 %; odds ratio [OR] 1.56, 95 % CI 1.03-2.37) and 11-12 weeks of treatment interval (20.8 %; OR 1.94, 95 % CI 1.15-3.26). Treatment interval did not influence OS in ET or LARC patients.
Conclusions: Treatment intervals of 9-12 weeks between surgery and CRT seem to improve the chances of pCR in LARC patients, without an effect on OS. The length of treatment interval did not affect outcomes in patients with ET. The ongoing search for minimally invasive surgery drives the need for exploration of factors that improve pathologic response.
Figures
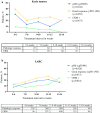
References
-
- Consensus statement on the multidisciplinary management of patients with recurrent and primary rectal cancer beyond total mesorectal excision planes. Br J Surg. 2013;100(8):E1-33. - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Research Materials

