Patterns of metastasis and recurrence in thymic epithelial tumours: longitudinal imaging review in correlation with histological subtypes
- PMID: 27267746
- PMCID: PMC5010483
- DOI: 10.1016/j.crad.2016.05.007
Patterns of metastasis and recurrence in thymic epithelial tumours: longitudinal imaging review in correlation with histological subtypes
Abstract
Aim: To determine the patterns of metastasis and recurrence in thymic epithelial tumours based on longitudinal imaging studies, and to correlate the patterns with World Health Organization (WHO) histological classifications.
Materials and methods: Seventy-seven patients with histopathologically confirmed thymomas (n=62) and thymic carcinomas (n=15) who were followed with cross-sectional follow-up imaging after surgery were retrospectively studied. All cross-sectional imaging studies during the disease course were reviewed to identify metastasis or recurrence. The sites of involvement and the time of involvement measured from surgery were recorded.
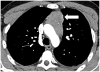
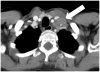
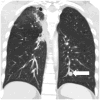
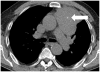
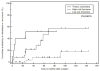
Results: Metastasis or recurrence was noted in 24 (31%) of the 77 patients. Patients with metastasis or recurrence were significantly younger than those without (median age: 46 versus 60, respectively; p=0.0005), and more commonly had thymic carcinomas than thymomas (p=0.002). The most common site of involvement was the pleura (17/24), followed by the lung (9/24), and thoracic nodes (9/24). Abdominopelvic involvement was noted in 12 patients, most frequently in the liver (n=8). Lung metastasis was more common in thymic carcinomas than thymomas (p=0.0005). Time from surgery to the development of metastasis or recurrence was shortest in thymic carcinoma, followed by high-risk thymomas, and was longest in low-risk thymoma (median time in months: 25.1, 68.8, and not reached, respectively; p=0.0015).
Conclusions: The patterns of metastasis and recurrence of thymic epithelial tumours differ significantly across histological subgroups, with thymic carcinomas more commonly having metastasis with shorter length of time after surgery. The knowledge of different patterns of tumour spread may contribute to further understanding of the biological and clinical behaviours of these tumours.
Copyright © 2016 The Royal College of Radiologists. Published by Elsevier Ltd. All rights reserved.
Figures


Similar articles
-
Does CT of thymic epithelial tumors enable us to differentiate histologic subtypes and predict prognosis?AJR Am J Roentgenol. 2004 Aug;183(2):283-9. doi: 10.2214/ajr.183.2.1830283. AJR Am J Roentgenol. 2004. PMID: 15269013
-
The utility of [18F]-fluorodeoxyglucose positron emission tomography-computed tomography in thymic epithelial tumours.Eur J Cardiothorac Surg. 2012 Dec;42(6):e152-6. doi: 10.1093/ejcts/ezs527. Epub 2012 Sep 28. Eur J Cardiothorac Surg. 2012. PMID: 23024234
-
Doubling time of thymic epithelial tumours on CT: correlation with histological subtype.Eur Radiol. 2017 Oct;27(10):4030-4036. doi: 10.1007/s00330-017-4795-y. Epub 2017 Mar 22. Eur Radiol. 2017. PMID: 28332015
-
Risk factors and prognostic factors of pleural metastases in thymic epithelial tumors: A narrative review.Eur J Surg Oncol. 2025 May;51(5):109639. doi: 10.1016/j.ejso.2025.109639. Epub 2025 Jan 27. Eur J Surg Oncol. 2025. PMID: 39892088
-
What is the role of lymph nodal metastases and lymphadenectomy in the surgical treatment and prognosis of thymic carcinomas and carcinoids?Interact Cardiovasc Thorac Surg. 2014 Dec;19(6):1054-8. doi: 10.1093/icvts/ivu281. Epub 2014 Sep 4. Interact Cardiovasc Thorac Surg. 2014. PMID: 25193970 Review.
Cited by
-
Histomorphological Spectrum and Diagnostic Challenges in Thymic Epithelial Neoplasms with their Prognostic Significance: A Case Series of 33 Cases at a Regional Cancer Center in Western India.South Asian J Cancer. 2022 Dec 2;13(3):191-202. doi: 10.1055/s-0042-1757556. eCollection 2024 Jul. South Asian J Cancer. 2022. PMID: 39410987 Free PMC article.
-
Thymoma metastatic to liver and pancreas: case report and review of the literature.J Int Med Res. 2017 Apr;45(2):868-874. doi: 10.1177/0300060516680673. Epub 2017 Feb 13. J Int Med Res. 2017. PMID: 28415940 Free PMC article.
-
Promotor methylation status of MAPK4 is a novel epigenetic biomarker for prognosis of recurrence in patients with thymic epithelial tumors.Thorac Cancer. 2022 Oct;13(20):2844-2853. doi: 10.1111/1759-7714.14628. Epub 2022 Sep 8. Thorac Cancer. 2022. PMID: 36073321 Free PMC article.
-
Type A thymoma with simultaneous solitary intrapulmonary metastasis: A case report.Thorac Cancer. 2021 Jun;12(12):1923-1926. doi: 10.1111/1759-7714.13975. Epub 2021 May 7. Thorac Cancer. 2021. PMID: 33960662 Free PMC article.
-
Thymic Carcinoma Presenting as a Mediastinal Mass Resembling a Cardiac Tumor.Cureus. 2024 May 31;16(5):e61455. doi: 10.7759/cureus.61455. eCollection 2024 May. Cureus. 2024. PMID: 38947614 Free PMC article.
References
-
- Nishino M, Ashiku SK, Kocher ON, Thurer RL, Boiselle PM, Hatabu H. The thymus: a comprehensive review. RadioGraphics. 2006;26:335–348. - PubMed
-
- Marom EM. Advances in thymoma imaging. J Thorac Imaging. 2013;28:69–80. quiz 81–63. - PubMed
-
- Marom EM. Imaging thymoma. J Thorac Oncol. 2010;5:S296–303. - PubMed
-
- Masaoka A, Monden Y, Nakahara K, Tanioka T. Follow-up study of thymomas with special reference to their clinical stages. Cancer. 1981;48:2485–2492. - PubMed
-
- Huang J, Detterbeck FC, Wang Z, Loehrer PJ., Sr Standard outcome measures for thymic malignancies. J Thorac Oncol. 2010;5:2017–2023. - PubMed
MeSH terms
Supplementary concepts
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

