Efficacy and Safety of Plastic Wrap for Prevention of Hypothermia after Birth and during NICU in Preterm Infants: A Systematic Review and Meta-Analysis
- PMID: 27281027
- PMCID: PMC4900561
- DOI: 10.1371/journal.pone.0156960
Efficacy and Safety of Plastic Wrap for Prevention of Hypothermia after Birth and during NICU in Preterm Infants: A Systematic Review and Meta-Analysis
Abstract
Objective: This meta-analysis aimed to investigate the efficacy and safety of plastic wrap applied after birth and during NICU in preterm infants for prevention of heat loss in preterm infants.
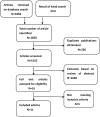
Study methods: The Medline (1950 to August 2015), the Cochrane Central Register of Controlled Trials (CENTRAL, Issue 7, 2015), CINAHL (1982 to August 2015) and the Embase (1974 to August 2015) databases were searched for randomized controlled trials (RCTs) or quasi-RCTs with main outcomes related to the core temperature (baseline temperature and/or post-stabilization temperature), hypothermia, mortality rate and hyperthermia.
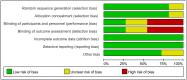
Result: The included studies were of low to moderate quality. Compared with unwrapped infants, plastic wrap was associated with a significantly higher baseline temperature and post-stabilization temperature both in infants < 28 weeks of gestation (mean difference [MD] = 0.62, 95% CI 0.38 to 0.85; MD = 0.41, 95% CI 0.33 to 0.50, respectively), and in infants between 28 to 34 weeks of gestation (MD = 0.54, 95% CI 0.21 to 0.87; MD = 0.64, 95% CI 0.45 to 0.82, respectively). Use of plastic wrap was associated with lower incidence of hypothermia (relative risk [RR] = 0.70, 95% CI 0.63 to 0.78). However, use of plastic wrap in preterm infants was not associated with decrease in mortality (RR: 0.88, 95% CI 0.70 to 1.12, P = 0.31). Incidence of hyperthermia was significantly higher in the plastic wrap group as compared to that in the control group (RR = 2.55, 95% CI: 1.56 to 4.15, P = 0.0002). Hyperthermia in the plastic wrap group was resolved within one or two hours after unwrapping the babies.
Conclusion: Plastic wrap can be considered an effective and safe additional intervention to prevent hypothermia in preterm infants. However, its cost-effectiveness and long-term effect on mortality needs to be ascertained by conducting well-designed studies with longer follow-up period.
Conflict of interest statement
Figures




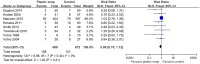
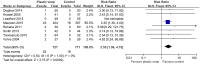

References
-
- Flamant C, Gascoin G. [Short-term outcome and small for gestational age newborn management]. J Gynecol Obstet Biol Reprod (Paris).2013; 42: 985–995. - PubMed
-
- Hazan J, Maag U, Chessex P. Association between hypothermia and mortality rate of premature infants—revisited. Am J Obstet Gynecol.1991; 164: 111–112. - PubMed
-
- Mannan MA, Jahan N, Dey SK, Uddin MF, Ahmed S. Maternal and foetal risk factor and complication with immediate outcome during hospital stay of very low birth weight babies. Mymensingh Med J.2012; 21: 639–647. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

