[Role of Postoperative Radiotherapy for Stage I/II/III Thymic Tumor - Results of the ChART Retrospective Database]
- PMID: 27339724
- PMCID: PMC6133973
- DOI: 10.3779/j.issn.1009-3419.2016.07.09
[Role of Postoperative Radiotherapy for Stage I/II/III Thymic Tumor - Results of the ChART Retrospective Database]
Abstract
Background: Postoperative radiotherapy (PORT) for thymic tumor is still controversial. The object of the study is to evaluate the role of PORT for stage I/II/III thymic tumor.
Methods: The database of Chinese Alliance of Research for Thymomas (ChART) was retrieved for patients with stage I/II/III thymic tumor who underwent surgical therapy without neoajuvant therapy between 1994 and 2012. Univariate and multivariate survival analyses were performed. Cox proportional hazard model was used to determine the hazard ratio for death.
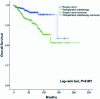
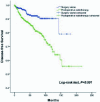
Results: 1,546 stage I/II/III patients were identified from ChART database. Among these patients, 649 (41.98%) underwent PORT. PORT was associated with gender, histologic type (World Health Organization, WHO), surgical extent, complete resection, Masaoka stage and adjuvant chemotherapy. The 5-yr and 10-yr overall survival (OS) rates and disease-free survival (DFS) rate for patients underwent surgery followed by PORT were 90% and 80%, 81% and 63%, comparing with 96% and 95%, 92% and 90% for patients underwent surgery alone (P=0.001, P<0.001) respectively. In univariate analysis, age, histologic type (WHO), Masaoka stage, completeness of resection, and PORT were associated with OS. Multivariable analysis showed that histologic type (WHO)(P=0.001), Masaoka stage (P=0.029) and completeness of resection (P=0.003) were independently prognostic factors of OS. In univariate analysis, gender, myasthenia gravis, histologic type (WHO), Masaoka stage, surgical approach, PORT and completeness of resection were associated with DFS. Multivariable analysis showed that histologic type (WHO) (P<0.001), Masaoka stage (P=0.005) and completeness of resection (P=0.006) were independently prognostic factors of DFS. Subgroup analysis showed that patients with incomplete resection underwent PORT achieved the better OS and DFS (P=0.010, 0.017, respectively). However, patients with complete resection underwent PORT had the worse OS and DFS (P<0.001, P<0.001, respectively).
Conclusions: The current retrospective study indicated that PORT after incomplete resection could improve OS and DFS for patients with stage I/II/III thymic tumor. But for those after complete resection, PORT may not help improve prognosis on the whole. .
背景与目的 胸腺肿瘤术后放疗尚存在争议,此研究目的为评价术后放疗在I期-III期胸腺肿瘤中的作用。方法 搜索中国胸腺瘤研究协作组(Chinese Alliance of Research for Thymomas, ChART)数据库中1994年至2012年接受手术切除未行新辅助治疗的I期-III期胸腺肿瘤患者的资料。对临床病理资料进行单因素、多因素分析,Cox比例风险模型用于决定死亡风险比。结果 ChART数据库中I期-III期胸腺肿瘤共1,546例。其中649例(41.98%)接受术后放疗。术后放疗与性别、组织学类型(World Health Organization, WHO)、胸腺切除程度、是否完全切除、Masaoka-Koga分期及辅助化疗相关。手术后辅助放疗患者5年、10年总生存和无瘤生存分别为90%和80%、81%和63%,而单纯手术者5年、10年总生存和无瘤生存分别为96%和95%、92%和90%,两组生存有统计学差异(P=0.001, P<0.001)。单因素表明年龄、组织学分类(WHO)、Masaoka-Koga分期、是否完全切除和术后放疗与总生存相关。多因素分析提示组织学分类(WHO)(P=0.001)、Masaoka-Koga分期(P=0.029)和是否完全切除(P=0.003)是总生存的独立预后因素。单因素分析表明性别、重症肌无力、组织学分类、Masaoka-Koga分期、手术方式、术后放疗和是否完全切除与无瘤生存相关。多因素分析表明组织学类型(P<0.001)、Masaoka-Koga分期(P=0.005)和是否完全切除(P=0.006)是无瘤生存的独立预后因素。亚组分析表明不完全切除患者接受术后放疗可以提高总生存和无瘤生存(P=0.010, P=0.017)。然而,完全切除者接受术后放疗则会降低总生存和无瘤生存(P<0.001, P<0.001)。结论 此回顾性研究表明不完全切除I期-III期胸腺肿瘤患者术后放疗可以提高总生存和无瘤生存。但是,对于完全切除患者,术后放疗总体上并未显示出生存获益。.
Figures
Similar articles
-
The role of postoperative radiotherapy for stage I/II/III thymic tumor-results of the ChART retrospective database.J Thorac Dis. 2016 Apr;8(4):687-95. doi: 10.21037/jtd.2016.03.28. J Thorac Dis. 2016. PMID: 27114836 Free PMC article.
-
Postoperative radiotherapy is effective for thymic carcinoma but not for thymoma in stage II and III thymic epithelial tumors: the Japanese Association for Research on the Thymus Database Study.Cancer. 2015 Apr 1;121(7):1008-16. doi: 10.1002/cncr.29166. Epub 2015 Jan 6. Cancer. 2015. PMID: 25565590
-
The Impact of Postoperative Radiotherapy for Thymoma and Thymic Carcinoma.J Thorac Oncol. 2017 Apr;12(4):734-744. doi: 10.1016/j.jtho.2017.01.002. Epub 2017 Jan 25. J Thorac Oncol. 2017. PMID: 28126540
-
Survival Impact of Adjuvant Radiation Therapy in Masaoka Stage II to IV Thymomas: A Systematic Review and Meta-analysis.Int J Radiat Oncol Biol Phys. 2016 Apr 1;94(5):1129-36. doi: 10.1016/j.ijrobp.2016.01.007. Epub 2016 Jan 14. Int J Radiat Oncol Biol Phys. 2016. PMID: 27026316
-
The value of postoperative radiotherapy in thymoma patients with myasthenia gravis.Radiother Oncol. 2023 Jun;183:109644. doi: 10.1016/j.radonc.2023.109644. Epub 2023 Mar 27. Radiother Oncol. 2023. PMID: 36990391 Review.
Cited by
-
The role of postoperative radiotherapy for thymomas: a multicentric retrospective evaluation from three Italian centers and review of the literature.J Thorac Dis. 2020 Dec;12(12):7518-7530. doi: 10.21037/jtd-2019-thym-09. J Thorac Dis. 2020. PMID: 33447442 Free PMC article.
References
-
- Engels EA. Epidemiology of thymoma and associated malignancies. http://europepmc.org/abstract/MED/20859116. J Thorac Oncol. 2010;5(10 Suppl 4):S260–S265. - PMC - PubMed
-
- Deterbeck F, Youssef S, Rufni E, et al. A review of prognostic factors in thymic malignancies. https://www.jto.org/article/S1556-0864(15)32894-X/fulltext. J Thorac Oncol. 2011;6(7 Suppl 3):S1698–S1704. - PubMed
-
- Deterbeck FC, Zeeshan A. Thymoma:current diagnosis and treatment. https://www.ncbi.nlm.nih.gov/pubmed/23769581. Chin Med J (Engl) 2013;126(11):2186–2191. - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Medical

