Ultrasound Quality Assurance for Singletons in the National Institute of Child Health and Human Development Fetal Growth Studies
- PMID: 27353072
- PMCID: PMC6309992
- DOI: 10.7863/ultra.15.09087
Ultrasound Quality Assurance for Singletons in the National Institute of Child Health and Human Development Fetal Growth Studies
Abstract
Objectives: To report on the ultrasound quality assurance program for the National Institute of Child Health and Human Development Fetal Growth Studies and describe both its advantages and generalizability.
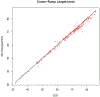
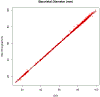
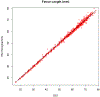
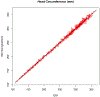
Methods: After training on an ultrasound system and software, research sonographers were expected to capture blank (unmeasured) images in triplicate for crown-rump length, biparietal diameter, head circumference, abdominal circumference, and femur length. A primary expert sonographer was designated and validated. A 5% sample (n = 740 of 14,785 scans) was randomly selected in 3 distinct rounds from within strata of maternal body mass index (round 1 only), gestational age, and research site. Unmeasured images were extracted from selected scans and measured with the ultrasound software by an expert sonographer. Correlations and coefficients of variation (CVs) were calculated, and the within-measurement standard deviation (ie, technical error of the measurement), was calculated.
Results: The reliability between the site sonographers and the expert was high, with correlations exceeding 0.99 for all dimensions in all rounds. The CV % values showed low variability, with the percentage differences being less than 2%, except for abdominal circumference in rounds 2 and 3, in which it averaged about 3%. Correlations remained high (>0.90) with increasing fetal size; there was a monotonic increase in technical errors of the measurement but without a corresponding increase in the CV %.
Conclusions: Using rigorous procedures for training sonographers, coupled with quality assurance oversight, we determined that the measurements acquired longitudinally for singletons are both accurate and reliable for establishment of an ultrasound standard for fetal growth.
Keywords: obstetric ultrasound; obstetrics; quality assurance; quality control; reliability; ultrasound.
Figures
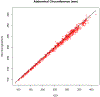
References
-
- Buck Louis GM, Grewal J, Albert PS, Sciscione A, Wing DA, Grobman WA, Newman RB, Wapner R, D’Alton ME, Skupski D, Nageotte MP, Ranzini AC, Owen J, Chien EK, Craigo S, Hediger ML, Kim S, Zhang C, Grantz KL. Racial/ethnic standards for fetal growth, the NICHD Fetal Growth Studies. Am J Obstet Gynecol 2015; 213(4):449.e1–449.e41. - PMC - PubMed
-
- Mueller RH, Martorell R. Reliability and accuracy of measurement In: Lohman TG, Roche AF, Martorell R (eds), Anthropometric Standardization Reference Manual. Champaign, IL: Human Kinetics Books, 1988:83–86.
-
- Ulijaszek SJ, Kerr DA. Anthropometric measurement error and the assessment of nutritional status. Br J Nutr 1999; 82:165–177 (Erratum: Br J Nutr 2000; 83:95). - PubMed
-
- Cameron N Essential anthropometry: baseline anthropometric methods for human biologists in laboratory and field situations. Am J Hum Biol 2013; 25:291–299. - PubMed
-
- Milani S, Bossi A, Bertino E, Di Battista E, Coscia A, Aicardi G, Fabris C, Benso L. Differences in size at birth are determined by differences in growth velocity during early prenatal life. Pediatr Res 2005; 57:205–210. - PubMed
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

