No effects of oral vitamin D supplementation on non-alcoholic fatty liver disease in patients with type 2 diabetes: a randomized, double-blind, placebo-controlled trial
- PMID: 27353492
- PMCID: PMC4926287
- DOI: 10.1186/s12916-016-0638-y
No effects of oral vitamin D supplementation on non-alcoholic fatty liver disease in patients with type 2 diabetes: a randomized, double-blind, placebo-controlled trial
Abstract
Background: Non-alcoholic fatty liver disease (NAFLD) is the most common hepatic disorder worldwide, reaching prevalence up to 90 % in obese patients with type 2 diabetes (T2D), and representing an independent risk factor for cardiovascular mortality. Furthermore, the coexistence of T2D and NAFLD leads to higher incidence of diabetes' complications and additive detrimental liver outcomes. The existence of a close association between NAFLD and hypovitaminosis D, along with the anti-inflammatory and insulin-sensitizing properties of vitamin D, have been largely described, but vitamin D effects on hepatic fat content have never been tested in a randomized controlled trial. We assessed the efficacy and safety of 24-week oral high-dose vitamin D supplementation in T2D patients with NAFLD.
Methods: This randomized, double-blind, placebo-controlled trial was carried out at the Diabetes Centre of Sapienza University, Rome, Italy, to assess oral treatment with cholecalciferol (2000 IU/day) or placebo in T2D patients with NAFLD. The primary endpoint was reduction of hepatic fat fraction (HFF) measured by magnetic resonance; as hepatic outcomes, we also investigated changes in serum transaminases, CK18-M30, N-terminal Procollagen III Propeptide (P3NP) levels, and Fatty Liver Index (FLI). Secondary endpoints were improvement in metabolic (fasting glycaemia, HbA1c, lipids, HOMA-IR, HOMA-β, ADIPO-IR, body fat distribution) and cardiovascular (ankle-brachial index, intima-media thickness, flow-mediated dilatation) parameters from baseline to end of treatment.
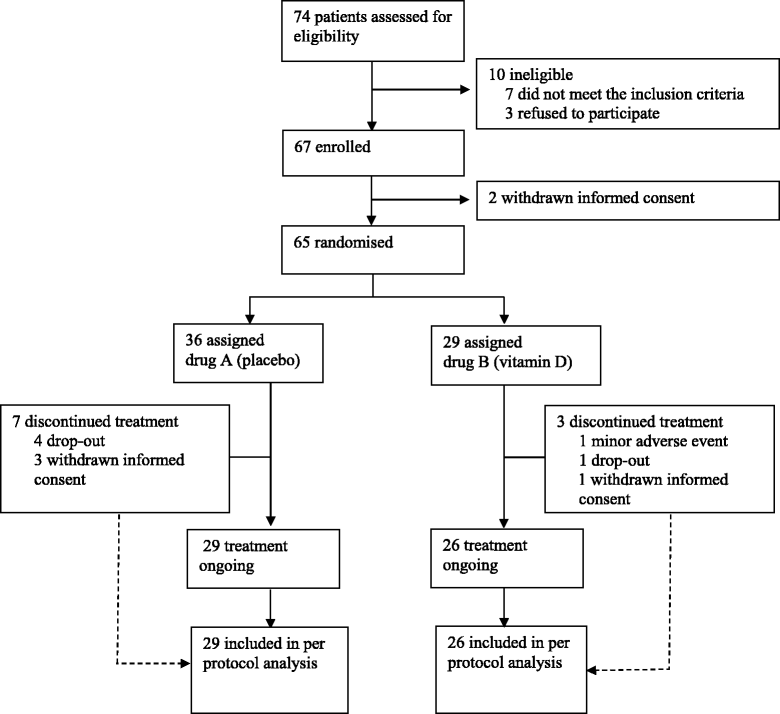
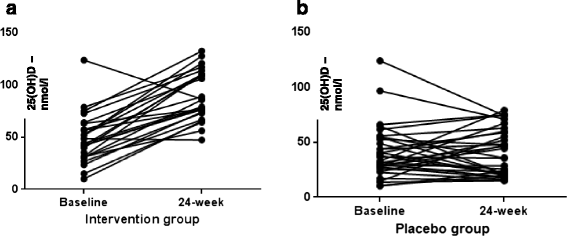
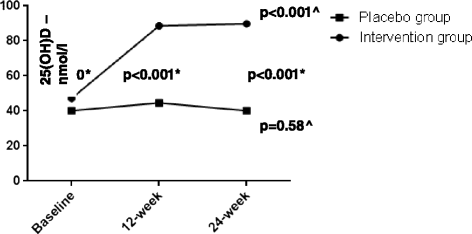
Results: Sixty-five patients were randomized, 26 (cholecalciferol) and 29 (placebo) subjects completed the study. 25(OH) vitamin D significantly increased in the active treated group (48.15 ± 23.7 to 89.80 ± 23.6 nmol/L, P < 0.001); however, no group differences were found in HFF, transaminases, CK18-M30, P3NP levels or FLI after 24 weeks. Vitamin D neither changed the metabolic profile nor the cardiovascular parameters.
Conclusions: Oral high-dose vitamin D supplementation over 24 weeks did not improve hepatic steatosis or metabolic/cardiovascular parameters in T2D patients with NAFLD. Studies with a longer intervention period are warranted for exploring the effect of long time exposure to vitamin D.
Trial registration: This trial was approved on July 2011 by the Ethics Committee of Policlinico Umberto I, Sapienza University of Rome, Italy, and registered at www.clinicaltrialsregister.eu number 2011-003010-17.
Keywords: Fatty liver; NAFLD; Type 2 diabetes; Vitamin D supplementation.
Figures
References
-
- Clark JM, Brancati FL, Diehl AME. Nonalcoholic fatty liver disease: the most common cause of abnormal liver enzymes in the US population. Gastroenterology. 2011;120(5 Suppl 1):A65.
-
- Chalasani N, Younossi Z, Lavine JE, Diehl AM, Brunt EM, Cusi K, et al. The diagnosis and management of non-alcoholic fatty liver disease: practice Guideline by the American Association for the Study of Liver Diseases, American College of Gastroenterology, and the American Gastroenterological Association. Hepatology. 2012;55(6):2005–23. doi: 10.1002/hep.25762. - DOI - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

