Analysis of contemporary HIV/AIDS health care costs in Germany: Driving factors and distribution across antiretroviral therapy lines
- PMID: 27367993
- PMCID: PMC4937907
- DOI: 10.1097/MD.0000000000003961
Analysis of contemporary HIV/AIDS health care costs in Germany: Driving factors and distribution across antiretroviral therapy lines
Abstract
To analyze contemporary costs of HIV health care and the cost distribution across lines of combination antiretroviral therapy (cART). To identify variations in expenditures with patient characteristics and to identify main cost determinants. To compute cost ratios between patients with varying characteristics.Empirical data on costs are collected in Germany within a 2-year prospective observational noninterventional multicenter study. The database contains information for 1154 HIV-infected patients from 8 medical centers.Means and standard deviations of the total costs are estimated for each cost fraction and across cART lines and regimens. The costs are regressed against various patient characteristics using a generalized linear model. Relative costs are calculated using the resultant coefficients.The average annual total costs (SD) per patient are &OV0556;22,231.03 (8786.13) with a maximum of &OV0556;83,970. cART medication is the major cost fraction (83.8%) with a mean of &OV0556;18,688.62 (5289.48). The major cost-driving factors are cART regimen, CD4-T cell count, cART drug resistance, and concomitant diseases. Viral load, pathology tests, and demographics have no significant impact. Standard non-nucleoside reverse transcriptase inhibitor-based regimens induce 28% lower total costs compared with standard PI/r regimens. Resistance to 3 or more antiretroviral classes induces a significant increase in costs.HIV treatment in Germany continues to be expensive. Majority of costs are attributable to cART. Main cost determinants are CD4-T cells count, comorbidity, genotypic antiviral resistance, and therapy regimen. Combinations of characteristics associated with higher expenditures enhance the increasing effect on the costs and induce high cost cases.
Conflict of interest statement
Conflicts of Interest and Source of Funding: CORSAR study has been funded by an unrestricted Janssen-Cilag grant.
HHeiken is currently a board member by Abbvie, Bristol-Myers-Squibb, Gilead, MSD, Janssen-Cilag and ViiV Healthcare. He has received payment for lectures from Bristol-Myers Squibb, Gilead, MSD, and ViiV Healthcare, and payment for manuscript preparation from Gilead. MT, AK, and J-MGvdS declared no conflict of interest.
Figures
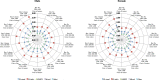
References
-
- Jaggy C, Overbeck F, Ledergerber B, et al. Mortality in the Swiss HIV Cohort Study (SHCS) and the Swiss general population. Lancet 2003; 362:877–878. - PubMed
-
- Department of Health and Human Services. Guidelines for the Use of Antiretroviral Agents in HIV-1-Infected Adults and Adolescents (November 13, 2014). Retrieved from http://aidsinfo.nih.gov/ContentFiles/Adultand.
-
- World Health Organization. Consolidated Guidelines on the Use of Antiretroviral Drugs for Treating and Preventing HIV Infection: Recommendations for a Public Health Approach. Geneva: World Health Organization; 2013. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Molecular Biology Databases
Research Materials
Miscellaneous

