Management and postoperative outcome in primary lung cancer and heart disease co-morbidity: a systematic review and meta-analysis
- PMID: 27386487
- PMCID: PMC4916362
- DOI: 10.21037/atm.2016.06.02
Management and postoperative outcome in primary lung cancer and heart disease co-morbidity: a systematic review and meta-analysis
Abstract
Background: Co-morbidity of primary lung cancer (LC) and heart disease (HD), both requiring surgical therapy, characterizes a high risk group of patients necessitating prompt diagnosis and treatment. The aim of this study is the review of available evidence guiding the management of these patients.
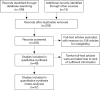
Methods: Postoperative outcome of patients operated for primary LC (first meta-analysis) and for both primary LC and HD co-morbidity (second meta-analysis), were studied. Parameters examined in both meta-analyses were thirty-day postoperative mortality, postoperative complications, three- and five-year survival probabilities. The last 36 years were reviewed by using the PubMed data base. Thirty-seven studies were qualified for both meta-analyses.
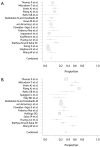
Results: The pooled 30-day mortality percentages (%) were 4.16% [95% confidence interval (CI): 2.68-5.95] (first meta-analysis) and 5.26% (95% CI: 3.47-7.62) (second meta-analysis). Higher percentages of squamous histology and lobectomy, were significantly associated with increased (P=0.001) and decreased (P<0.001) thirty-day postoperative mortality, respectively (first meta-analysis). The pooled percentages for postoperative complications were 34.32% (95% CI: 24.59-44.75) (first meta-analysis) and 45.59% (95% CI: 35.62-55.74) (second meta-analysis). Higher percentages of squamous histology (P=0.001), lobectomy (P=0.002) and p-T1 or p-T2 (P=0.034) were associated with higher proportions of postoperative complications (second meta-analysis). The pooled three- and five- year survival probabilities were 68.25% (95% CI: 45.93-86.86) and 52.03% (95% CI: 34.71-69.11), respectively. Higher mean age (P=0.046) and percentage lobectomy (P=0.009) significantly reduced the five-year survival probability.
Conclusions: Lobectomy and age were both accompanied by reduced five-year survival rate. Also, combined aorto-coronary bypass grafting (CABG) with lobectomy for squamous pT1 or pT2 LC displayed a higher risk of postoperative complications. Moreover, medical decision between combined or staged surgery is suggested to be individualized based on adequacy of coronary arterial perfusion, age, patient's preoperative performance status (taking into account possible co-morbidities per patient), tumor's staging and extent of lung resection.
Keywords: Lung neoplasms; heart disease (HD); intra-operative complications; perioperative period; surgery; survival rate.
Conflict of interest statement
Figures

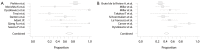
Similar articles
-
Perioperative outcomes of combined heart surgery and lung tumor resection: a systematic review and meta-analysis.J Cardiothorac Surg. 2021 Aug 9;16(1):227. doi: 10.1186/s13019-021-01607-7. J Cardiothorac Surg. 2021. PMID: 34372896 Free PMC article.
-
Additional mitral valve procedure and coronary artery bypass grafting versus isolated coronary artery bypass grafting in the management of significant functional ischemic mitral regurgitation: a meta-analysis.J Cardiovasc Surg (Torino). 2017 Feb;58(1):121-130. doi: 10.23736/S0021-9509.16.08852-2. Epub 2015 Jun 18. J Cardiovasc Surg (Torino). 2017. PMID: 26086215 Review.
-
Thoracoscopic lobectomy is associated with improved short-term and equivalent oncological outcomes compared with open lobectomy for clinical Stage I non-small-cell lung cancer: a propensity-matched analysis of 963 cases.Eur J Cardiothorac Surg. 2014 Oct;46(4):607-13. doi: 10.1093/ejcts/ezu036. Epub 2014 Mar 5. Eur J Cardiothorac Surg. 2014. PMID: 24603446
-
Simultaneous occurrence of coronary artery disease and lung cancer: what is the best surgical treatment strategy?Interact Cardiovasc Thorac Surg. 2014 Oct;19(4):673-81. doi: 10.1093/icvts/ivu218. Epub 2014 Jul 6. Interact Cardiovasc Thorac Surg. 2014. PMID: 25002274 Review.
-
Video-assisted thoracoscopic surgery lobectomy for lung cancer is associated with a lower 30-day morbidity compared with lobectomy by thoracotomy.Eur J Cardiothorac Surg. 2016 Mar;49(3):870-5. doi: 10.1093/ejcts/ezv205. Epub 2015 Jun 18. Eur J Cardiothorac Surg. 2016. PMID: 26088592
Cited by
-
Neoadjuvant therapy bridging percutaneous coronary intervention (PCI) and video-assisted thoracoscopic (VATS) lobectomy: a retrospective study.Transl Cancer Res. 2024 Jun 30;13(6):2662-2673. doi: 10.21037/tcr-24-132. Epub 2024 Jun 18. Transl Cancer Res. 2024. PMID: 38988932 Free PMC article.
-
Perioperative outcomes of combined heart surgery and lung tumor resection: a systematic review and meta-analysis.J Cardiothorac Surg. 2021 Aug 9;16(1):227. doi: 10.1186/s13019-021-01607-7. J Cardiothorac Surg. 2021. PMID: 34372896 Free PMC article.
-
Metastasis-associated protein 2 promotes the metastasis of non-small cell lung carcinoma by regulating the ERK/AKT and VEGF signaling pathways.Mol Med Rep. 2018 Apr;17(4):4899-4908. doi: 10.3892/mmr.2018.8535. Epub 2018 Feb 1. Mol Med Rep. 2018. Retraction in: Mol Med Rep. 2025 Apr;31(4):89. doi: 10.3892/mmr.2025.13454. PMID: 29393472 Free PMC article. Retracted.
-
Surgical management of a simultaneous aortic valve replacement and pneumonectomy.Indian J Thorac Cardiovasc Surg. 2018 Jul;34(3):420-424. doi: 10.1007/s12055-017-0616-9. Epub 2017 Nov 23. Indian J Thorac Cardiovasc Surg. 2018. PMID: 33060907 Free PMC article.
References
-
- Piehler JM, Trastek VF, Pairolero PC, et al. Concomitant cardiac and pulmonary operations. J Thorac Cardiovasc Surg 1985;90:662-7. - PubMed
LinkOut - more resources
Full Text Sources
Other Literature Sources
