Improving the Diagnosis and Treatment of Urinary Tract Infection in Young Children in Primary Care: Results from the DUTY Prospective Diagnostic Cohort Study
- PMID: 27401420
- PMCID: PMC4940462
- DOI: 10.1370/afm.1954
Improving the Diagnosis and Treatment of Urinary Tract Infection in Young Children in Primary Care: Results from the DUTY Prospective Diagnostic Cohort Study
Abstract
Purpose: Up to 50% of urinary tract infections (UTIs) in young children are missed in primary care. Urine culture is essential for diagnosis, but urine collection is often difficult. Our aim was to derive and internally validate a 2-step clinical rule using (1) symptoms and signs to select children for urine collection; and (2) symptoms, signs, and dipstick testing to guide antibiotic treatment.
Methods: We recruited acutely unwell children aged under 5 years from 233 primary care sites across England and Wales. Index tests were parent-reported symptoms, clinician-reported signs, urine dipstick results, and clinician opinion of UTI likelihood (clinical diagnosis before dipstick and culture). The reference standard was microbiologically confirmed UTI cultured from a clean-catch urine sample. We calculated sensitivity, specificity, and area under the receiver operator characteristic (AUROC) curve of coefficient-based (graded severity) and points-based (dichotomized) symptom/sign logistic regression models, and we then internally validated the AUROC using bootstrapping.
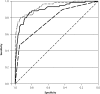
Results: Three thousand thirty-six children provided urine samples, and culture results were available for 2,740 (90%). Of these results, 60 (2.2%) were positive: the clinical diagnosis was 46.6% sensitive, with an AUROC of 0.77. Previous UTI, increasing pain/crying on passing urine, increasingly smelly urine, absence of severe cough, increasing clinician impression of severe illness, abdominal tenderness on examination, and normal findings on ear examination were associated with UTI. The validated coefficient- and points-based model AUROCs were 0.87 and 0.86, respectively, increasing to 0.90 and 0.90, respectively, by adding dipstick nitrites, leukocytes, and blood.
Conclusions: A clinical rule based on symptoms and signs is superior to clinician diagnosis and performs well for identifying young children for noninvasive urine sampling. Dipstick results add further diagnostic value for empiric antibiotic treatment.
Keywords: anti-bacterial agents; diagnosis; pediatrics; primary health care; urinary tract infections.
© 2016 Annals of Family Medicine, Inc.
Figures

References
-
- Farnham SB, Adams MC, Brock JW, III, Pope JC., IV Pediatric urological causes of hypertension. J Urol. 2005;173(3):697–704. - PubMed
-
- National Collaborating Centre for Women’s and Children’s Health. Urinary Tract Infection in Children: Diagnosis, Treatment and Long Term Management. London, England: RCOG Press; 2007. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
