Stroke volume changes induced by a recruitment maneuver predict fluid responsiveness in patients with protective ventilation in the operating theater
- PMID: 27428237
- PMCID: PMC4956831
- DOI: 10.1097/MD.0000000000004259
Stroke volume changes induced by a recruitment maneuver predict fluid responsiveness in patients with protective ventilation in the operating theater
Abstract
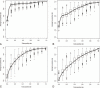
During abdominal surgery, the use of protective ventilation with a low tidal volume, positive expiratory pressure (PEEP) and recruitment maneuvers (RMs) may limit the applicability of dynamic preload indices. The objective of the present study was to establish whether or not the variation in stroke volume (SV) during an RM could predict fluid responsiveness.We prospectively included patients receiving protective ventilation (tidal volume: 6 mL kg, PEEP: 5-7 cmH2O; RMs). Hemodynamic variables, such as heart rate, arterial pressure, SV, cardiac output (CO), respiratory variation in SV (ΔrespSV) and pulse pressure (ΔrespPP), and the variation in SV (ΔrecSV) as well as pulse pressure (ΔrecPP) during an RM were measured at baseline, at the end of the RM, and after fluid expansion. Responders were defined as patients with an SV increase of at least 15% after infusion of 500 mL of crystalloid solution.Thirty-seven (62%) of the 60 included patients were responders. Responders and nonresponders differed significantly in terms of the median ΔrecSV (26% [19-37] vs 10% [4-12], respectively; P < 0.0001). A ΔrecSV value more than 16% predicted fluid responsiveness with an area under the receiver-operating characteristic curve (AU) of 0.95 (95% confidence interval [CI]: 0.91-0.99; P < 0.0001) and a narrow gray zone between 15% and 17%. The area under the curve values for ΔrecPP and ΔrespSV were, respectively, 0.81 (95%CI: 0.7-0.91; P = 0.0001) and 0.80 (95%CI: 0.70-0.94; P < 0.0001). ΔrespPP did not predict fluid responsiveness.During abdominal surgery with protective ventilation, a ΔrecSV value more than 16% accurately predicted fluid responsiveness and had a narrow gray zone (between 15% and 17%). ΔrecPP and ΔrespSV (but not ΔrespPP) were also predictive.
Conflict of interest statement
The authors have no conflicts of interest to declare.
Figures
Similar articles
-
End-expiratory occlusion manoeuvre does not accurately predict fluid responsiveness in the operating theatre.Br J Anaesth. 2014 Jun;112(6):1050-4. doi: 10.1093/bja/aet582. Epub 2014 Mar 4. Br J Anaesth. 2014. PMID: 24598390
-
Ability of stroke volume variation measured by oesophageal Doppler monitoring to predict fluid responsiveness during surgery.Br J Anaesth. 2013 Jan;110(1):28-33. doi: 10.1093/bja/aes301. Epub 2012 Aug 22. Br J Anaesth. 2013. PMID: 22918700
-
Hemodynamic Changes via the Lung Recruitment Maneuver Can Predict Fluid Responsiveness in Stroke Volume and Arterial Pressure During One-Lung Ventilation.Anesth Analg. 2021 Jul 1;133(1):44-52. doi: 10.1213/ANE.0000000000005375. Anesth Analg. 2021. PMID: 33687175
-
Stroke volume variation induced by lung recruitment maneuver to predict fluid responsiveness in patients receiving mechanical ventilation: A systematic review and meta-analysis.J Clin Anesth. 2024 Oct;97:111545. doi: 10.1016/j.jclinane.2024.111545. Epub 2024 Jul 5. J Clin Anesth. 2024. PMID: 38971135
-
Does End-Expiratory Occlusion Test Predict Fluid Responsiveness in Mechanically Ventilated Patients? A Systematic Review and Meta-Analysis.Shock. 2020 Dec;54(6):751-760. doi: 10.1097/SHK.0000000000001545. Shock. 2020. PMID: 32433213
Cited by
-
Fluid expansion improve ventriculo-arterial coupling in preload-dependent patients: a prospective observational study.BMC Anesthesiol. 2020 Jul 17;20(1):171. doi: 10.1186/s12871-020-01087-7. BMC Anesthesiol. 2020. PMID: 32680470 Free PMC article.
-
Functional hemodynamic tests: a systematic review and a metanalysis on the reliability of the end-expiratory occlusion test and of the mini-fluid challenge in predicting fluid responsiveness.Crit Care. 2019 Jul 29;23(1):264. doi: 10.1186/s13054-019-2545-z. Crit Care. 2019. PMID: 31358025 Free PMC article.
-
Assessment of fluid responsiveness using pulse pressure variation, stroke volume variation, plethysmographic variability index, central venous pressure, and inferior vena cava variation in patients undergoing mechanical ventilation: a systematic review and meta-analysis.Crit Care. 2024 Aug 31;28(1):289. doi: 10.1186/s13054-024-05078-9. Crit Care. 2024. PMID: 39217370 Free PMC article.
-
Reliability of pulse pressure and stroke volume variation in assessing fluid responsiveness in the operating room: a metanalysis and a metaregression.Crit Care. 2023 Nov 8;27(1):431. doi: 10.1186/s13054-023-04706-0. Crit Care. 2023. PMID: 37940953 Free PMC article.
-
Correlation coefficient between plethysmographic variability index and Systolic Pressure Variation as an indicator for fluid responsiveness in hypotensive patients in the ICU/OT.Med J Armed Forces India. 2024 Jan-Feb;80(1):52-59. doi: 10.1016/j.mjafi.2021.06.026. Epub 2021 Sep 7. Med J Armed Forces India. 2024. PMID: 38261854 Free PMC article.
References
-
- Hamilton MA, Cecconi M, Rhodes A. A systematic review and meta-analysis on the use of preemptive hemodynamic intervention to improve postoperative outcomes in moderate and high-risk surgical patients. Anesth Analg 2011; 112:1392–1402. - PubMed
-
- Perel A, Pizov R, Cotev S. Respiratory variations in the arterial pressure during mechanical ventilation reflect volume status and fluid responsiveness. Intensive Care Med 2014; 40:798–807. - PubMed
-
- Guerin L, Monnet X, Teboul JL. Monitoring volume and fluid responsiveness: from static to dynamic indicators. Best Pract Res Clin Anaesthesiol 2013; 27:177–185. - PubMed
-
- Futier E, Godet T, Millot A, et al. Mechanical ventilation in abdominal surgery. Ann Fr Anesth Reanim 2014; 33:472–475. - PubMed
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

