Histological inflammation increases the risk of colorectal neoplasia in ulcerative colitis: a systematic review
- PMID: 27433141
- PMCID: PMC4945523
- DOI: 10.5217/ir.2016.14.3.202
Histological inflammation increases the risk of colorectal neoplasia in ulcerative colitis: a systematic review
Abstract
Background/aims: Ulcerative colitis (UC) patients are at greater risk for the development of colorectal neoplasia. Several individual studies have demonstrated associations between severity of histologic inflammation and colorectal neoplasia. However, a comprehensive systematic review has not been completed. We performed a systematic review and meta-analysis to explore the relationship between histologic inflammation and risk for neoplasia among available observational studies.
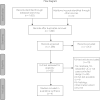
Methods: Three databases (EMBASE, MEDLINE and the Cochrane Library) were systematically searched. Studies were included if they included UC patients who underwent colonoscopic assessment and when histologic inflammation and colorectal neoplasia were both reported. Colorectal neoplasia rates were compared. Quantitative meta-analysis was attempted.
Results: Four of 1,422 records found were eligible. Results from 2 case-control studies reported a 3.5-fold increased risk for colorectal neoplasia associated with a single point increase in histologic inflammation. This result was further corroborated by one cohort study that demonstrated increased hazard ratios. The second cohort study reported outcomes for patients with normal gross endoscopy, but had increased histological inflammation when neoplasia was assessed. Finally, this study reported increased risk for neoplastic progression by histological inflammation among patients who were normal by gross endoscopic evaluation. Quantitative meta-analysis was unsuccessful due to heterogeneity between study measures.
Conclusions: There is strong evidence that histologic inflammation among patients with UC increases the risk of colorectal neoplasia. The depth and nature of assessment of additional clinical variables was varied and may have resulted in greater outcome discrepancy. Additional study related to mechanisms of inflammation-related neoplasia and therapeutic modification is needed.
Keywords: Colitis, ulcerative; Colorectal neoplasms; Dysplasia; Histologic inflammation.
Conflict of interest statement
Figures
Similar articles
-
Histologic inflammation is a risk factor for progression to colorectal neoplasia in ulcerative colitis: a cohort study.Gastroenterology. 2007 Oct;133(4):1099-105; quiz 1340-1. doi: 10.1053/j.gastro.2007.08.001. Epub 2007 Aug 2. Gastroenterology. 2007. PMID: 17919486 Free PMC article.
-
Severity of inflammation is a risk factor for colorectal neoplasia in ulcerative colitis.Gastroenterology. 2004 Feb;126(2):451-9. doi: 10.1053/j.gastro.2003.11.010. Gastroenterology. 2004. PMID: 14762782
-
Patients With Ulcerative Colitis and Primary Sclerosing Cholangitis Frequently Have Subclinical Inflammation in the Proximal Colon.Clin Gastroenterol Hepatol. 2018 Jan;16(1):68-74. doi: 10.1016/j.cgh.2017.07.023. Epub 2017 Jul 26. Clin Gastroenterol Hepatol. 2018. PMID: 28756053 Free PMC article.
-
Increased risk of colorectal neoplasia in patients with primary sclerosing cholangitis and inflammatory bowel disease: a meta-analysis of 16 observational studies.Eur J Gastroenterol Hepatol. 2016 Apr;28(4):383-90. doi: 10.1097/MEG.0000000000000576. Eur J Gastroenterol Hepatol. 2016. PMID: 26938805 Review.
-
Systematic review with meta-analysis: endoscopic and histologic placebo rates in induction and maintenance trials of ulcerative colitis.Aliment Pharmacol Ther. 2018 Jun;47(12):1578-1596. doi: 10.1111/apt.14672. Epub 2018 Apr 25. Aliment Pharmacol Ther. 2018. PMID: 29696670
Cited by
-
Disease clearance in ulcerative colitis: A new therapeutic target for the future.World J Gastroenterol. 2024 Apr 7;30(13):1801-1809. doi: 10.3748/wjg.v30.i13.1801. World J Gastroenterol. 2024. PMID: 38659483 Free PMC article. Review.
-
Inflammatory Bowel Disease and Risk of Colorectal Polyps: A Nationwide Population-Based Cohort Study From Sweden.J Crohns Colitis. 2023 Oct 20;17(9):1395-1409. doi: 10.1093/ecco-jcc/jjad056. J Crohns Colitis. 2023. PMID: 36994851 Free PMC article.
-
Advanced neoplasia detection using chromoendoscopy and white light colonoscopy for surveillance in patients with inflammatory bowel disease.Intest Res. 2020 Oct;18(4):438-446. doi: 10.5217/ir.2019.00090. Epub 2020 Oct 26. Intest Res. 2020. PMID: 33131232 Free PMC article.
-
Deployment of an Artificial Intelligence Histology Tool to Aid Qualitative Assessment of Histopathology Using the Nancy Histopathology Index in Ulcerative Colitis.Inflamm Bowel Dis. 2025 Jun 13;31(6):1630-1636. doi: 10.1093/ibd/izae204. Inflamm Bowel Dis. 2025. PMID: 39284932 Free PMC article.
-
Endoscopic Diagnosis of Nonpedunculated Dysplasia during Surveillance of Ulcerative Colitis: A Survey-Based Multinational Study.Gut Liver. 2020 Sep 15;14(5):611-618. doi: 10.5009/gnl19237. Gut Liver. 2020. PMID: 31842526 Free PMC article.
References
-
- Rutter M, Saunders B, Wilkinson K, et al. Severity of inflammation is a risk factor for colorectal neoplasia in ulcerative colitis. Gastroenterology. 2004;126:451–459. - PubMed
-
- Moher D, Liberati A, Tetzlaff J, Altman DG, PRISMA Group. Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. Int J Surg. 2010;8:336–341. - PubMed
Publication types
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical