Clinical Outcomes of Gamma Knife Radiosurgery for Metastatic Brain Tumors from Gynecologic Cancer : Prognostic Factors in Local Treatment Failure and Survival
- PMID: 27446522
- PMCID: PMC4954889
- DOI: 10.3340/jkns.2016.59.4.392
Clinical Outcomes of Gamma Knife Radiosurgery for Metastatic Brain Tumors from Gynecologic Cancer : Prognostic Factors in Local Treatment Failure and Survival
Abstract
Objective: Brain metastases in gynecologic cancer (ovarian, endometrial, and cervical cancer) patients are rare, and the efficacy of Gamma Knife Radiosurgery (GKRS) to treat these had not been evaluated. We assessed the efficacy of GKRS and prognostic factors for tumor control and survival in brain metastasis from gynecologic cancers.
Methods: This retrospective study was approved by the institutional review board. From May 1995 to October 2012, 26 women (mean age 51.3 years, range 27-70 years) with metastatic brain tumors from gynecologic cancer were treated with GKRS. We reviewed their outcomes, radiological responses, and clinical status.
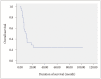
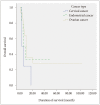
Results: In total 24 patients (59 lesions) were available for follow-up imaging. The median follow-up time was 9 months. The mean treated tumor volume at the time of GKRS was 8185 mm(3) (range 10-19500 mm(3)), and the median dose delivered to the tumor margin was 25 Gy (range, 10-30 Gy). A local tumor control rate was 89.8% (53 of 59 tumors). The median overall survival was 9.5 months after GKRS (range, 1-102 months). Age-associated multivariate analysis indicated that the Karnofsky performance status (KPS), the recursive partitioning analysis (RPA) classification, and the number of treated lesions were significant prognostic factors for overall survival (HR=0.162, p=0.008, HR=0.107, p=0.038, and HR=2.897, p=0.045, respectively).
Conclusion: GKRS is safe and effective for the management of brain metastasis from gynecologic cancers. The clinical status of the patient is important in determining the overall survival time.
Keywords: Brain metastases; Gamma Knife Radiosurgery; Gynecologic cancer; Prognostic factor; Survival.
Figures

References
-
- Bindal RK, Sawaya R, Leavens ME, Lee JJ. Surgical treatment of multiple brain metastases. J Neurosurg. 1993;79:210–216. - PubMed
-
- Bradley JD, Paulus R, Graham MV, Ettinger DS, Johnstone DW, Pilepich MV, et al. Phase II trial of postoperative adjuvant paclitaxel/carboplatin and thoracic radiotherapy in resected stage II and IIIA non-small-cell lung cancer : promising long-term results of the Radiation Therapy Oncology Group--RTOG 9705. J Clin Oncol. 2005;23:3480–3487. - PubMed
-
- Brown JV, 3rd, Goldstein BH, Duma CM, Rettenmaier MA, Micha JP. Gamma-knife radiosurgery for the treatment of ovarian cancer metastatic to the brain. Gynecol Oncol. 2005;97:858–861. - PubMed
-
- Chen PG, Lee SY, Barnett GH, Vogelbaum MA, Saxton JP, Fleming PA, et al. Use of the Radiation Therapy Oncology Group recursive partitioning analysis classification system and predictors of survival in 19 women with brain metastases from ovarian carcinoma. Cancer. 2005;104:2174–2180. - PubMed
LinkOut - more resources
Full Text Sources
Other Literature Sources

