Quantifying reperfusion of the ischemic region on whole-brain computed tomography perfusion
- PMID: 27461903
- PMCID: PMC5464706
- DOI: 10.1177/0271678X16661338
Quantifying reperfusion of the ischemic region on whole-brain computed tomography perfusion
Abstract
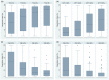
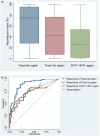
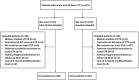
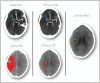
To derive the reperfusion index best predicting clinical outcome of ischemic stroke patients, we retrospectively analysed the acute and 24-h computed tomography perfusion data of 116 patients, collected from two centres equipped with whole-brain computed tomography perfusion. Reperfusion index was defined by the percentage of the ischemic region reperfused from acute to 24-h computed tomography perfusion. Recanalization was graded by arterial occlusive lesion system. Receiver operator characteristic analysis was performed to assess the prognostic value of reperfusion and recanalization in predicting good clinical outcome, defined as modified Rankin Score of 0-2 at 90 days. Among previous reported reperfusion measurements, reperfusion of the Tmax>6 s region resulted in higher prognostic value than recanalization at predicting good clinical outcome (area under the curve = 0.88 and 0.74, respectively, p = 0.002). Successful reperfusion of the Tmax>6 s region (≥60%) had 89% sensitivity and 78% specificity in predicting good clinical outcome. A reperfusion index defined by Tmax>2 s or by mean transit time>145% had much lower area under the curve in comparison to Tmax>6 s measurement (p < 0.001 and p = 0.003, respectively), and had no significant difference to recanalization at predicting clinical outcome (p = 0.58 and 0.63, respectively). In conclusion, reperfusion index calculated by Tmax>6 s is a stronger predictor of clinical outcome than recanalization or other reperfusion measures.
Keywords: Acute stroke; brain imaging; brain ischemia; cerebral blood flow measurement; reperfusion.
Figures

Similar articles
-
Prediction of Clinical Outcome After Acute Ischemic Stroke: The Value of Repeated Noncontrast Computed Tomography, Computed Tomographic Angiography, and Computed Tomographic Perfusion.Stroke. 2017 Sep;48(9):2593-2596. doi: 10.1161/STROKEAHA.117.017835. Epub 2017 Jul 17. Stroke. 2017. PMID: 28716981
-
Perfusion computed tomography thresholds defining ischemic penumbra and infarct core: studies in a rat stroke model.Int J Stroke. 2015 Jun;10(4):553-9. doi: 10.1111/ijs.12147. Epub 2013 Oct 21. Int J Stroke. 2015. PMID: 24138577
-
Good Clinical and Radiological Correlation from Standard Perfusion Computed Tomography Accurately Identifies Salvageable Tissue in Ischemic Stroke.J Stroke Cerebrovasc Dis. 2016 May;25(5):1062-1069. doi: 10.1016/j.jstrokecerebrovasdis.2016.01.009. Epub 2016 Feb 5. J Stroke Cerebrovasc Dis. 2016. PMID: 26856462
-
Early postischemic hyperperfusion: pathophysiologic insights from positron emission tomography.J Cereb Blood Flow Metab. 1999 May;19(5):467-82. doi: 10.1097/00004647-199905000-00001. J Cereb Blood Flow Metab. 1999. PMID: 10326714 Review.
-
MR and CT monitoring of recanalization, reperfusion, and penumbra salvage: everything that recanalizes does not necessarily reperfuse!Stroke. 2009 Mar;40(3 Suppl):S24-7. doi: 10.1161/STROKEAHA.108.526814. Epub 2008 Dec 8. Stroke. 2009. PMID: 19064812 Review.
Cited by
-
Imaging After Thrombolysis and Thrombectomy: Rationale, Modalities and Management Implications.Curr Neurol Neurosci Rep. 2019 Jul 6;19(8):57. doi: 10.1007/s11910-019-0970-7. Curr Neurol Neurosci Rep. 2019. PMID: 31278596 Review.
-
Bridging Thrombolysis Before Endovascular Therapy in Stroke Patients With Faster Core Growth.Neurology. 2023 May 16;100(20):e2083-e2092. doi: 10.1212/WNL.0000000000207154. Epub 2023 Mar 24. Neurology. 2023. PMID: 36963842 Free PMC article.
-
What Is the "Optimal" Target Mismatch Criteria for Acute Ischemic Stroke?Front Neurol. 2021 Jan 13;11:590766. doi: 10.3389/fneur.2020.590766. eCollection 2020. Front Neurol. 2021. PMID: 33584495 Free PMC article.
-
A non-human primate model of stroke reproducing endovascular thrombectomy and allowing long-term imaging and neurological read-outs.J Cereb Blood Flow Metab. 2021 Apr;41(4):745-760. doi: 10.1177/0271678X20921310. Epub 2020 May 19. J Cereb Blood Flow Metab. 2021. PMID: 32428423 Free PMC article.
-
Crossed cerebellar diaschisis in acute ischemic stroke: Impact on morphologic and functional outcome.J Cereb Blood Flow Metab. 2017 Nov;37(11):3615-3624. doi: 10.1177/0271678X16686594. Epub 2017 Jan 13. J Cereb Blood Flow Metab. 2017. PMID: 28084869 Free PMC article.
References
-
- Rha JH, Saver JL. The impact of recanalization on ischemic stroke outcome: a meta-analysis. Stroke 2007; 38: 967–973. - PubMed
-
- Eilaghi A, Brooks J, d'Esterre C, et al. Reperfusion is a stronger predictor of good clinical outcome than recanalization in ischemic stroke. Radiology 2013; 269: 240–248. - PubMed
-
- De Silva DA, Fink JN, Christensen S, et al. Assessing reperfusion and recanalization as markers of clinical outcomes after intravenous thrombolysis in the echoplanar imaging thrombolytic evaluation trial (EPITHET). Stroke 2009; 40: 2872–2874. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Molecular Biology Databases

