Therapeutic Efficacy and Cost Effectiveness of High Cut-Off Dialyzers Compared to Conventional Dialysis in Patients with Cast Nephropathy
- PMID: 27467401
- PMCID: PMC4965060
- DOI: 10.1371/journal.pone.0159942
Therapeutic Efficacy and Cost Effectiveness of High Cut-Off Dialyzers Compared to Conventional Dialysis in Patients with Cast Nephropathy
Abstract
Background: High Cut-Off (HCO) dialysis membranes efficiently reduce serum free light chain (FLC) concentrations and may improve renal recovery and survival from multiple myeloma (MM) associated renal failure with cast nephropathy. However, clinical trials comparing dialysis with HCO versus conventional filters are lacking. The aim of this study was to assess clinical outcomes and economic impact of HCO dialyzers compared to conventional hemodialysis membranes in cast nephropathy.
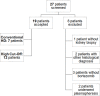
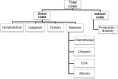
Methods: Multicenter retrospective analysis of 19 patients treated for renal failure from FLC associated cast nephropathy with standard induction chemotherapy (bortezomib/dexamethasone). We compared hemodialysis treatment with High Cut-Off (n = 12) versus conventional dialyzers (n = 7). Primary endpoint was survival; secondary endpoints were renal recovery, renal function and treatment costs.
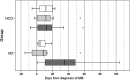
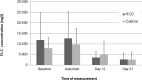
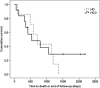
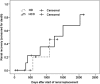
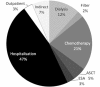
Results: At 12 months, patient survival was 25% in the HCO group versus 0% in controls (p = NS). A tendency towards faster renal recovery (p = 0.066) and better renal function at 3, 6 and 12 months (p = 0.109) after diagnosis of MM was noted in the HCO group. Complete renal response rate was achieved in 10.5 and 0% of HCO and control patients, respectively, partial renal response in 15.8 and 5.3%, and minor renal response in 26.3 and 15.8%, respectively. Both patient survival and renal recovery were significantly correlated with the extent of free light chain (FLC) reduction in serum. Median treatment costs were CHF 230'000 and 223'000 (p = NS) in the HCO and control group, respectively.
Conclusions: Hemodialysis treatment with HCO membranes for cast nephropathy tended towards better survival as well as faster and better recovery of renal function versus conventional dialyzers. Moreover, total medical costs were comparable between groups. In the absence of results from randomized prospective trials on this topic, the use of HCO dialyzers in patients with renal failure from cast nephropathy may be recommended. Prospective randomized trials are required.
Conflict of interest statement
Figures
Similar articles
-
High cutoff versus high-flux haemodialysis for myeloma cast nephropathy in patients receiving bortezomib-based chemotherapy (EuLITE): a phase 2 randomised controlled trial.Lancet Haematol. 2019 Apr;6(4):e217-e228. doi: 10.1016/S2352-3026(19)30014-6. Epub 2019 Mar 11. Lancet Haematol. 2019. PMID: 30872075 Clinical Trial.
-
Effectiveness of IHD with Adsorptive PMMA Membrane in Myeloma Cast Nephropathy: A Cohort Study.Am J Nephrol. 2017;46(5):355-363. doi: 10.1159/000481461. Epub 2017 Oct 10. Am J Nephrol. 2017. PMID: 29017155
-
Thirteen treated of acute renal failure secondary to multiple myeloma with high cut off filters.Nefrologia. 2016 Jul-Aug;36(4):418-26. doi: 10.1016/j.nefro.2016.03.011. Epub 2016 May 31. Nefrologia. 2016. PMID: 27255910 English, Spanish.
-
Treatment of acute kidney injury with cast nephropathy.Clin Nephrol. 2014 Jul;82(1):1-6. doi: 10.5414/CN108293. Clin Nephrol. 2014. PMID: 24725380 Review.
-
Management options for cast nephropathy in multiple myeloma.Curr Opin Nephrol Hypertens. 2010 Nov;19(6):550-5. doi: 10.1097/MNH.0b013e32833ef72c. Curr Opin Nephrol Hypertens. 2010. PMID: 20827195 Review.
Cited by
-
Extracorporeal light-chain elimination in myeloma with simple medium cutoff membrane hemodialysis: a retrospective cohort study.Front Oncol. 2023 Sep 8;13:1193504. doi: 10.3389/fonc.2023.1193504. eCollection 2023. Front Oncol. 2023. PMID: 37746285 Free PMC article.
-
Serum free light chain level at diagnosis in myeloma cast nephropathy-a multicentre study.Blood Cancer J. 2020 Mar 3;10(3):28. doi: 10.1038/s41408-020-0295-4. Blood Cancer J. 2020. PMID: 32127527 Free PMC article.
-
Histological Findings in Kidney Biopsies of Patients with Monoclonal Gammopathy-Always a Surprise.Diagnostics (Basel). 2022 Aug 7;12(8):1912. doi: 10.3390/diagnostics12081912. Diagnostics (Basel). 2022. PMID: 36010261 Free PMC article.
-
Impact of hemodialysis on the prognosis of multiple myeloma: A nationwide population-based study and single-institute analysis.Oncol Lett. 2018 Aug;16(2):1991-2002. doi: 10.3892/ol.2018.8857. Epub 2018 May 31. Oncol Lett. 2018. PMID: 30008893 Free PMC article.
-
Effect of High-Cutoff Hemodialysis vs Conventional Hemodialysis on Hemodialysis Independence Among Patients With Myeloma Cast Nephropathy: A Randomized Clinical Trial.JAMA. 2017 Dec 5;318(21):2099-2110. doi: 10.1001/jama.2017.17924. JAMA. 2017. PMID: 29209721 Free PMC article. Clinical Trial.
References
-
- Bladé J, Fernández-Llama P, Bosch F, Montolíu J, Lens XM, Montoto S, et al. Renal failure in multiple myeloma: presenting features and predictors of outcome in 94 patients from a single institution. Arch Intern Med. 1998;158(17):1889–93. . - PubMed
-
- Dimopoulos MA, Delimpasi S, Katodritou E, Vassou A, Kyrtsonis MC, Repousis P, et al. Significant improvement in the survival of patients with multiple myeloma presenting with severe renal impairment after the introduction of novel agents. Ann Oncol. 2014;25(1):195–200. 10.1093/annonc/mdt483 . - DOI - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Miscellaneous

