PTK7 overexpression in colorectal tumors: Clinicopathological correlation and prognosis relevance
- PMID: 27499181
- PMCID: PMC5022898
- DOI: 10.3892/or.2016.4983
PTK7 overexpression in colorectal tumors: Clinicopathological correlation and prognosis relevance
Abstract
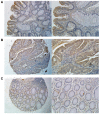
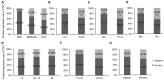
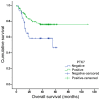
Colorectal cancer (CRC) has one of the highest mortality rates in the worldwide and its incidence has been increasing in recent years. Protein tyrosine kinase-7 (PTK7) is an inactive member of receptor protein tyrosine kinase (RPTK)-like molecules, which is involved in tumorigenesis of a variety of cancers. Our study aimed to investigate expression of PTK7 in colorectal tumors (including benign adenomas and malignant carcinomas), and its potential function in tumorigenesis and prognosis. A total of 209 CRC patients and 28 colonic adenoma patients were included in this study. Reverse transcription polymerase chain reaction (RT-PCR) and quantitative real-time PCR were performed in 14 pairs of fresh frozen tissues to evaluate mRNA expression of PTK7. Expression of PTK7 protein in 209 CRC tissues with paired non-cancerous mucosa and 28 adenoma specimens were tested using immunohistochemistry. The expression difference and its correlation with clinicopathological features and overall survival were assessed by SPSS statistics (version 22). P<0.05 was considered significant. RT-PCR and quantitative real-time PCR showed a higher expression of PTK7 mRNA in CRC compared with non-tumorous mucosa (4.87±3.71 vs. 1.33±1.05; P<0.001). PTK7 expression was significantly higher in adenoma (75%) and CRC (68.3%) than in non-tumorous mucosa (P<0.001). PTK7 expression was correlated with tumor differentiation (P=0.027), lymph node metastasis (P=0.005), distant metastasis (P=0.001) and TNM stage (P=0.028) of CRC patients. Significant correlation between PTK7 overexpression and favorable overall survival of CRC patients was observed (P=0.005). Therefore, it may act as a candidate biomarker to predict the occurrence and prognosis of colorectal tumor.
Figures


References
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Miscellaneous

